Epidemiology and outcomes of early-onset AKI in COVID-19-related ARDS in comparison with non-COVID-19-related ARDS: insights from two prospective global cohort studies
- PMID: 36604753
- PMCID: PMC9814373
- DOI: 10.1186/s13054-022-04294-5
Epidemiology and outcomes of early-onset AKI in COVID-19-related ARDS in comparison with non-COVID-19-related ARDS: insights from two prospective global cohort studies
Erratum in
-
Correction : Epidemiology and outcomes of early-onset AKI in COVID-19-related ARDS in comparison with non-COVID-19-related ARDS: insights from two prospective global cohort studies.Crit Care. 2023 May 26;27(1):202. doi: 10.1186/s13054-023-04487-6. Crit Care. 2023. PMID: 37237395 Free PMC article. No abstract available.
Abstract
Background: Acute kidney injury (AKI) is a frequent and severe complication of both COVID-19-related acute respiratory distress syndrome (ARDS) and non-COVID-19-related ARDS. The COVID-19 Critical Care Consortium (CCCC) has generated a global data set on the demographics, management and outcomes of critically ill COVID-19 patients. The LUNG-SAFE study was an international prospective cohort study of patients with severe respiratory failure, including ARDS, which pre-dated the pandemic.
Methods: The incidence, demographic profile, management and outcomes of early AKI in patients undergoing invasive mechanical ventilation for COVID-19-related ARDS were described and compared with AKI in a non-COVID-19-related ARDS cohort.
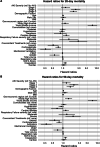
Results: Of 18,964 patients in the CCCC data set, 1699 patients with COVID-19-related ARDS required invasive ventilation and had relevant outcome data. Of these, 110 (6.5%) had stage 1, 94 (5.5%) had stage 2, 151 (8.9%) had stage 3 AKI, while 1214 (79.1%) had no AKI within 48 h of initiating invasive mechanical ventilation. Patients developing AKI were older and more likely to have hypertension or chronic cardiac disease. There were geo-economic differences in the incidence of AKI, with lower incidence of stage 3 AKI in European high-income countries and a higher incidence in patients from middle-income countries. Both 28-day and 90-day mortality risk was increased for patients with stage 2 (HR 2.00, p < 0.001) and stage 3 AKI (HR 1.95, p < 0.001). Compared to non-COVID-19 ARDS, the incidence of shock was reduced with lower cardiovascular SOFA score across all patient groups, while hospital mortality was worse in all groups [no AKI (30 vs 50%), Stage 1 (38 vs 58%), Stage 2 (56 vs 74%), and Stage 3 (52 vs 72%), p < 0.001]. The time profile of onset of AKI also differed, with 56% of all AKI occurring in the first 48 h in patients with COVID-19 ARDS compared to 89% in the non-COVID-19 ARDS population.
Conclusion: AKI is a common and serious complication of COVID-19, with a high mortality rate, which differs by geo-economic location. Important differences exist in the profile of AKI in COVID-19 versus non-COVID-19 ARDS in terms of their haemodynamic profile, time of onset and clinical outcomes.
Keywords: 28-day mortality; 90-day mortality; ARDS; Acute kidney injury; COVID-19; Cohort study; Outcome.
© 2023. The Author(s).
Conflict of interest statement
A/Prof Li Bassi received research support from Fisher & Paykel outside the submitted work. Dr McNicholas has provided consultancy to Teleflex. Prof. Brodie receives research support from ALung Technologies, and he has been on the medical advisory boards for Baxter, Abiomed, Xenios and Hemovent. Prof. Laffey reports consulting fees from Baxter and Cala Medical, both outside the submitted work. Prof. Fraser receives research support from Fisher & Paykel outside the submitted work.
Figures