Temporomandibular Joint Osteoarthritis: Pathogenic Mechanisms Involving the Cartilage and Subchondral Bone, and Potential Therapeutic Strategies for Joint Regeneration
- PMID: 36613615
- PMCID: PMC9820477
- DOI: 10.3390/ijms24010171
Temporomandibular Joint Osteoarthritis: Pathogenic Mechanisms Involving the Cartilage and Subchondral Bone, and Potential Therapeutic Strategies for Joint Regeneration
Abstract
The temporomandibular joint (TMJ) is a specialized synovial joint that is crucial for the movement and function of the jaw. TMJ osteoarthritis (TMJ OA) is the result of disc dislocation, trauma, functional overburden, and developmental anomalies. TMJ OA affects all joint structures, including the articular cartilage, synovium, subchondral bone, capsule, ligaments, periarticular muscles, and sensory nerves that innervate the tissues. The present review aimed to illustrate the main pathomechanisms involving cartilage and bone changes in TMJ OA and some therapeutic options that have shown potential restorative properties regarding these joint structures in vivo. Chondrocyte loss, extracellular matrix (ECM) degradation, and subchondral bone remodeling are important factors in TMJ OA. The subchondral bone actively participates in TMJ OA through an abnormal bone remodeling initially characterized by a loss of bone mass, followed by reparative mechanisms that lead to stiffness and thickening of the condylar osteochondral interface. In recent years, such therapies as intraarticular platelet-rich plasma (PRP), hyaluronic acid (HA), and mesenchymal stem cell-based treatment (MSCs) have shown promising results with respect to the regeneration of joint structures or the protection against further damage in TMJ OA. Nevertheless, PRP and MSCs are more frequently associated with cartilage and/or bone repair than HA. According to recent findings, the latter could enhance the restorative potential of other therapies (PRP, MSCs) when used in combination, rather than repair TMJ structures by itself. TMJ OA is a complex disease in which degenerative changes in the cartilage and bone develop through intricate mechanisms. The regenerative potential of such therapies as PRP, MSCs, and HA regarding the cartilage and subchondral bone (alone or in various combinations) in TMJ OA remains a matter of further research, with studies sometimes obtaining discrepant results.
Keywords: bone remodeling; chondrocyte death; osteoarthritis; regenerative therapy; temporomandibular joint.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

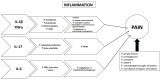
References
-
- Gomes L.R., Gomes M.R., Jung B., Paniagua B., Ruellas A.C., Gonçalves J.R., Styner M.A., Wolford L.M., Cevidanes L. Diagnostic Index of Three-Dimensional Osteoarthritic Changes in Temporomandibular Joint Condylar Morphology. J. Med. Imaging. 2015;2:1. doi: 10.1117/1.JMI.2.3.034501. - DOI - PMC - PubMed
-
- Haigler M.C., Abdulrehman E., Siddappa S., Kishore R., Padilla M., Enciso R. Use of platelet-rich plasma, platelet-rich growth factor with arthrocentesis or arthroscopy to treat temporomandibular joint osteoarthritis: Systematic review with meta-analyses. J. Am. Dent. Assoc. 2018;149:940–952. doi: 10.1016/j.adaj.2018.07.025. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

