Tunneling of Mesh during Ventral Rectopexy: Technical Aspects and Long-Term Functional Results
- PMID: 36615094
- PMCID: PMC9821569
- DOI: 10.3390/jcm12010294
Tunneling of Mesh during Ventral Rectopexy: Technical Aspects and Long-Term Functional Results
Abstract
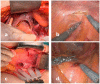
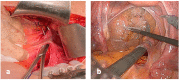
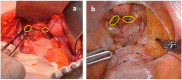
Avoiding the extensive damage of pelvic structures during ventral rectopexy could minimize secondary disfunctions. The objective of our observational study is to assess the safety and functional efficacy of a modified ventral rectopexy. In the modified ventral rectopexy, a retroperitoneal tunnel was created along the right side of rectum, connecting two peritoneal mini-incisions at the Douglas pouch and sacral promontory. The proximal edge of a polypropylene mesh, sutured over the ventral rectum, was pulled up through the retroperitoneal tunnel and fixed to the sacral promontory. In all patients, radiopaque clips were placed on the mesh, making it radiographically "visible". Before surgery and at follow up visits, Altomare, Longo, CCSS, PAC-SYM, and CCFI scores were collected. From March 2010 to September 2021, 117 patients underwent VR. Modified ventral rectopexy was performed in 65 patients, while the standard ventral rectopexy was performed in 52 patients. The open approach was used in 97 cases (55 and 42 patients in modified and standard VR, respectively), while MI surgery was used in 20 cases (10 and 10 patients in modified and standard VR, respectively). A slightly shorter operative time and hospital stay were observed following modified ventral rectopexy (though this was not statistically significant). Similar overall complication rates were registered in the modified vs. standard ventral rectopexies (4.6% vs. 5.8%, p = 0.779). At follow-up, the Longo score (14.0 ± 8.6 vs. 11.0 ± 8.2, p = 0.042) and "delta" values of Altomare (9.2 ± 6.1 vs. 5.9 ± 6.3, p = 0.008) and CCSS (8.4 ± 6.3 vs. 6.1 ± 6.1, p = 0.037) scores were significantly improved in the modified ventral rectopexy group. A similar occurrence of symptoms recurrence was diagnosed in the two groups. Radiopaque clips helped to accurately diagnose mesh detachment/dislocation. The proposed modified VR seems to be feasible and safe. Marking the mesh intraoperatively seems useful.
Keywords: fecal incontinence; obstructed defecation syndrome; pelvic disorders; rectal prolapse; ventral rectopexy.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

Similar articles
-
Bowel function after laparoscopic posterior sutured rectopexy versus ventral mesh rectopexy for rectal prolapse: a double-blind, randomised single-centre study.Lancet Gastroenterol Hepatol. 2016 Dec;1(4):291-297. doi: 10.1016/S2468-1253(16)30085-1. Epub 2016 Oct 4. Lancet Gastroenterol Hepatol. 2016. PMID: 28404199 Clinical Trial.
-
Technical modifications for cost optimization in robot-assisted ventral mesh rectopexy: an initial experience.Tech Coloproctol. 2023 Jul;27(7):551-557. doi: 10.1007/s10151-023-02756-8. Epub 2023 Feb 18. Tech Coloproctol. 2023. PMID: 36802041 Free PMC article.
-
Robot-Assisted Ventral Mesh Rectopexy for Rectal Prolapse: A 5-Year Experience at a Tertiary Referral Center.Dis Colon Rectum. 2017 Nov;60(11):1215-1223. doi: 10.1097/DCR.0000000000000895. Dis Colon Rectum. 2017. PMID: 28991087
-
Robotic vs. laparoscopic ventral mesh rectopexy for external rectal prolapse and rectal intussusception: a systematic review.Tech Coloproctol. 2019 Jun;23(6):529-535. doi: 10.1007/s10151-019-02014-w. Epub 2019 Jun 28. Tech Coloproctol. 2019. PMID: 31254202
-
[Alloplastic material in prolapse surgery : Indications and postoperative outcome of ventral rectopexy].Chirurg. 2017 Feb;88(2):141-146. doi: 10.1007/s00104-016-0264-4. Chirurg. 2017. PMID: 27515904 Review. German.
Cited by
-
Surgical approaches for complete rectal prolapse.World J Gastrointest Surg. 2025 Mar 27;17(3):102043. doi: 10.4240/wjgs.v17.i3.102043. World J Gastrointest Surg. 2025. PMID: 40162412 Free PMC article. Review.
-
Analysis of factors that indicated surgery in 400 patients submitted to a complete diagnostic workup for obstructed defecation syndrome and rectal prolapse using a supervised machine learning algorithm.Tech Coloproctol. 2024 Jun 25;28(1):73. doi: 10.1007/s10151-024-02951-1. Tech Coloproctol. 2024. PMID: 38918256
References
-
- Wijffels N., Cunningham C., Dixon A., Greenslade G., Lindsey I. Laparoscopic ventral rectopexy for external rectal prolapse is safe and effective in the elderly. Does this make perineal procedures obsolete? Color. Dis. Off. J. Assoc. Coloproctol. Great Br. Irel. 2011;13:561–566. doi: 10.1111/j.1463-1318.2010.02242.x. - DOI - PubMed
-
- Mercer-Jones M.A., Brown S.R., Knowles C.H., Williams A.B. Position statement by the Pelvic Floor Society on behalf of the Association of Coloproctology of Great Britain and Ireland on the use of mesh in ventral mesh rectopexy. Color. Dis. 2020;22:1429–1435. doi: 10.1111/codi.13893. - DOI - PMC - PubMed
-
- Auguste T., Dubreuil A., Bost R., Bonaz B., Faucheron J.L. Technical and functional results after laparoscopic rectopexy to the promontory for complete rectal prolapse. Prospective study in 54 consecutive patients. Gastroenterol. Clin. Biol. 2006;30:659–663. doi: 10.1016/S0399-8320(06)73257-2. - DOI - PubMed
LinkOut - more resources
Full Text Sources

