Continuous multi-day tracking of post-myocardial infarction recovery of cardiac electrical stability and autonomic tone using electrocardiogram patch monitors
- PMID: 36630149
- PMCID: PMC9833356
- DOI: 10.1111/anec.13035
Continuous multi-day tracking of post-myocardial infarction recovery of cardiac electrical stability and autonomic tone using electrocardiogram patch monitors
Abstract
Background: Sudden cardiac death (SCD) risk is elevated following acute myocardial infarction (MI). The time course of SCD susceptibility post-MI requires further investigation.
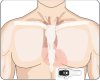
Methods: In this observational cohort study, we employed state-of-the-art noninvasive ECG techniques to track the daily time course of cardiac electrical instability and autonomic function following ST-segment elevation myocardial infarction (STEMI) and non-STEMI (NSTEMI). Preventice BodyGuardian MINI-EL Holters continuously recorded ECGs for 7 days at hospital discharge and at 40 days for STEMI (N = 5) or at 90 days for NSTEMI patients (N = 5). Cardiac electrical instability was assessed by T-wave alternans (TWA) and T-wave heterogeneity (TWH); autonomic tone was determined by rMSSD-heart rate variability (HRV).
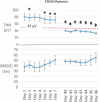
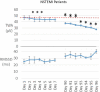
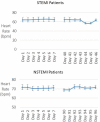
Results: TWA was severely elevated (≥60 μV) in STEMI patients (80 ± 10.3 μV) at discharge and throughout the first recording period but declined by 50% to 40 ± 2.3 μV (p = .03) by Day 40 and remained in the normal range (<47 μV). TWH, a related phenomenon analyzed from 12-lead ECGs, was reduced by 63% in the five STEMI patients from discharge to normal (<80 μV) at follow-up (105 ± 27.3 to 39 ± 3.3 μV, p < .04) but increased by 65% in a STEMI case (89 to 147 μV), who received a wearable defibrillator vest and later implantable cardioverter defibrillator. In NSTEMI patients, TWA was borderline abnormal (47 ± 3.3 μV) at discharge and declined by 19% to normal (38 ± 1.2 μV) by Day 90 (p = .05). An overall reciprocal increase in rMSSD-HRV suggested recovery of vagal tone.
Conclusions: This study provides proof-of-principle for tracking post-MI SCD risk in individual patients with implications for personalized therapy.
Keywords: ST-elevation myocardial infarction; T-wave alternans; T-wave heterogeneity; heart rate variability; non-ST-elevation myocardial infarction.
© 2022 The Authors. Annals of Noninvasive Electrocardiology published by Wiley Periodicals LLC.
Conflict of interest statement
None of the authors has a conflict of interest. Drs. Verrier and Varma are members of the Editorial Board of Annals of Noninvasive Electrocardiology. To avoid bias, they were excluded from all editorial decision‐making related to the acceptance of this article for publication.
Figures


Similar articles
-
Ambulatory ECG-based T-wave alternans monitoring for risk assessment and guiding medical therapy: mechanisms and clinical applications.Prog Cardiovasc Dis. 2013 Sep-Oct;56(2):172-85. doi: 10.1016/j.pcad.2013.07.002. Epub 2013 Sep 21. Prog Cardiovasc Dis. 2013. PMID: 24215749
-
Ambulatory ECG-based T-wave alternans and heart rate turbulence can predict cardiac mortality in patients with myocardial infarction with or without diabetes mellitus.Cardiovasc Diabetol. 2012 Sep 6;11:104. doi: 10.1186/1475-2840-11-104. Cardiovasc Diabetol. 2012. PMID: 22950360 Free PMC article.
-
T-wave alternans and heart rate variability: a comparison in patients with myocardial infarction with or without diabetes mellitus.Ann Noninvasive Electrocardiol. 2011 Jul;16(3):232-8. doi: 10.1111/j.1542-474X.2011.00437.x. Ann Noninvasive Electrocardiol. 2011. PMID: 21762250 Free PMC article.
-
Arrhythmias After Acute Myocardial Infarction.Yale J Biol Med. 2023 Mar 31;96(1):83-94. doi: 10.59249/LSWK8578. eCollection 2023 Mar. Yale J Biol Med. 2023. PMID: 37009192 Free PMC article. Review.
-
Secondary electrocardiographic stratification of NSTEMI to identify an acutely occluded culprit artery.Physiol Meas. 2023 Jul 17;44(7). doi: 10.1088/1361-6579/acddc8. Physiol Meas. 2023. PMID: 37307848 Review.
Cited by
-
Wearable Devices for Arrhythmia Detection: Advancements and Clinical Implications.Sensors (Basel). 2025 Apr 30;25(9):2848. doi: 10.3390/s25092848. Sensors (Basel). 2025. PMID: 40363284 Free PMC article. Review.
References
-
- Cohagan, B. , & Brandis, D. (2022). Torsades de Pointes [Internet]. StatPearls Publishing. - PubMed
-
- Hoshida, K. , Miwa, Y. , Miyakoshi, M. , Tsukada, T. , Yusu, S. , Yoshino, H. , & Ikeda, T. (2013). Simultaneous assessment of T‐wave alternans and heart rate turbulence on Holter electrocardiograms as predictors for serious cardiac events in patients after myocardial infarction. Circulation Journal, 77(2), 432–438. 10.1253/circj.cj-12-0789 - DOI - PubMed
-
- Kenttä, T. V. , Nearing, B. D. , Porthan, K. , Tikkanen, J. T. , Viitasalo, M. , Nieminen, M. S. , Salomaa, V. , Oikarinen, L. , Huikuri, H. V. , & Verrier, R. L. (2016). Prediction of sudden cardiac death with automated high throughput analysis of heterogeneity in standard resting 12‐lead electrocardiogram. Heart Rhythm, 13, 713–720. 10.1016/j.hrthm.2015.11.035 - DOI - PubMed
-
- Kramer, J. M. , Hammill, B. , Anstrom, K. J. , Fetterolf, D. , Snyder, R. , Charde, J. P. , Hoffman, B. S. , Allen LaPointe, N. , & Peterson, E. (2006). National evaluation of adherence to beta‐blocker therapy for 1 year after acute myocardial infarction in patients with commercial health insurance. American Heart Journal, 152(3), 454.e1‐8. 10.1016/j.ahj.2006.02.030 - DOI - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

