Geographic disparities in COVID-19 testing and outcomes in Florida
- PMID: 36631768
- PMCID: PMC9832260
- DOI: 10.1186/s12889-022-14450-9
Geographic disparities in COVID-19 testing and outcomes in Florida
Abstract
Background: Understanding geographic disparities in Coronavirus Disease 2019 (COVID-19) testing and outcomes at the local level during the early stages of the pandemic can guide policies, inform allocation of control and prevention resources, and provide valuable baseline data to evaluate the effectiveness of interventions for mitigating health, economic and social impacts. Therefore, the objective of this study was to identify geographic disparities in COVID-19 testing, incidence, hospitalizations, and deaths during the first five months of the pandemic in Florida. METHODS: Florida county-level COVID-19 data for the time period March-July 2020 were used to compute various COVID-19 metrics including testing rates, positivity rates, incidence risks, percent of hospitalized cases, hospitalization risks, case-fatality rates, and mortality risks. High or low risk clusters were identified using either Kulldorff's circular spatial scan statistics or Tango's flexible spatial scan statistics and their locations were visually displayed using QGIS.
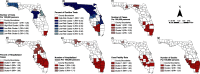
Results: Visual examination of spatial patterns showed high estimates of all COVID-19 metrics for Southern Florida. Similar to the spatial patterns, high-risk clusters for testing and positivity rates and all COVID-19 outcomes (i.e. hospitalizations and deaths) were concentrated in Southern Florida. The distributions of these metrics in the other parts of Florida were more heterogeneous. For instance, testing rates for parts of Northwest Florida were well below the state median (11,697 tests/100,000 persons) but they were above the state median for North Central Florida. The incidence risks for Northwest Florida were equal to or above the state median incidence risk (878 cases/100,000 persons), but the converse was true for parts of North Central Florida. Consequently, a cluster of high testing rates was identified in North Central Florida, while a cluster of low testing rate and 1-3 clusters of high incidence risks, percent of hospitalized cases, hospitalization risks, and case fatality rates were identified in Northwest Florida. Central Florida had low-rate clusters of testing and positivity rates but it had a high-risk cluster of percent of hospitalized cases.
Conclusions: Substantial disparities in the spatial distribution of COVID-19 outcomes and testing and positivity rates exist in Florida, with Southern Florida counties generally having higher testing and positivity rates and more severe outcomes (i.e. hospitalizations and deaths) compared to Northern Florida. These findings provide valuable baseline data that is useful for assessing the effectiveness of preventive interventions, such as vaccinations, in various geographic locations in the state. Future studies will need to assess changes in spatial patterns over time at lower geographical scales and determinants of any identified patterns.
Keywords: COVID-19; Disparities; Florida; Spatial Clusters; USA.
© 2023. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

Similar articles
-
Geographic disparities and temporal changes of diabetes-related mortality risks in Florida: a retrospective study.PeerJ. 2024 Jun 27;12:e17408. doi: 10.7717/peerj.17408. eCollection 2024. PeerJ. 2024. PMID: 38948203 Free PMC article.
-
Geographic disparities and temporal changes in risk of death from myocardial infarction in Florida, 2000-2014.BMC Public Health. 2019 May 3;19(1):505. doi: 10.1186/s12889-019-6850-x. BMC Public Health. 2019. PMID: 31053068 Free PMC article.
-
Geographic disparities and temporal changes of COVID-19 hospitalization risks in North Dakota.Front Public Health. 2023 Mar 16;11:1062177. doi: 10.3389/fpubh.2023.1062177. eCollection 2023. Front Public Health. 2023. PMID: 37006524 Free PMC article.
-
Investigation of geographic disparities and temporal changes of non-gestational diabetes-related emergency department visits in Florida: a retrospective ecological study.PeerJ. 2025 Jan 31;13:e18897. doi: 10.7717/peerj.18897. eCollection 2025. PeerJ. 2025. PMID: 39902319 Free PMC article.
-
Exploiting epidemiological data to understand the epidemiology and factors that influence COVID-19 pandemic in Libya.World J Virol. 2021 Jul 25;10(4):156-167. doi: 10.5501/wjv.v10.i4.156. World J Virol. 2021. PMID: 34367931 Free PMC article. Review.
Cited by
-
Variation in Time Between Testing Positive for COVID-19 and Hospital Admission by Race/Ethnicity and Insurance Status.J Health Care Poor Underserved. 2023;34(4):1290-1304. J Health Care Poor Underserved. 2023. PMID: 38661756 Free PMC article.
-
Health equity in COVID-19 testing among patients of a large national pharmacy chain.Front Public Health. 2024 Sep 11;12:1422914. doi: 10.3389/fpubh.2024.1422914. eCollection 2024. Front Public Health. 2024. PMID: 39324167 Free PMC article.
-
Crash harm before and during the COVID-19 pandemic: Evidence for spatial heterogeneity in Tennessee.Accid Anal Prev. 2023 Apr;183:106988. doi: 10.1016/j.aap.2023.106988. Epub 2023 Jan 25. Accid Anal Prev. 2023. PMID: 36724654 Free PMC article.
-
Overcoming Health Inequities: Spatial Analysis of Seroprevalence and Vaccination Against COVID-19 in Chile.Health Equity. 2024 Aug 26;8(1):558-567. doi: 10.1089/heq.2023.0204. eCollection 2024. Health Equity. 2024. PMID: 40125367 Free PMC article.
-
Spatial patterns and sociodemographic predictors of chronic obstructive pulmonary disease in Florida.PeerJ. 2024 Aug 2;12:e17771. doi: 10.7717/peerj.17771. eCollection 2024. PeerJ. 2024. PMID: 39104363 Free PMC article.
References
-
- The COVID Tracking Project . Data Download. 2021.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

