Predictive markers related to local and systemic inflammation in severe COVID-19-associated ARDS: a prospective single-center analysis
- PMID: 36631778
- PMCID: PMC9832419
- DOI: 10.1186/s12879-023-07980-z
Predictive markers related to local and systemic inflammation in severe COVID-19-associated ARDS: a prospective single-center analysis
Abstract
Background: As the COVID-19 pandemic strains healthcare systems worldwide, finding predictive markers of severe courses remains urgent. Most research so far was limited to selective questions hindering general assumptions for short- and long-term outcome.
Methods: In this prospective single-center biomarker study, 47 blood- and 21 bronchoalveolar lavage (BAL) samples were collected from 47 COVID-19 intensive care unit (ICU) patients upon admission. Expression of inflammatory markers toll-like receptor 3 (TLR3), heme oxygenase-1 (HO-1), interleukin (IL)-6, IL-8, leukocyte counts, procalcitonin (PCT) and carboxyhemoglobin (CO-Hb) was compared to clinical course. Clinical assessment comprised acute local organ damage, acute systemic damage, mortality and outcome after 6 months.
Results: PCT correlated with acute systemic damage and was the best predictor for quality of life (QoL) after 6 months (r = - 0.4647, p = 0.0338). Systemic TLR3 negatively correlated with impaired lung function (ECMO/ECLS: r = - 0.3810, p = 0.0107) and neurological short- (RASS mean: r = 0.4474, p = 0.0023) and long-term outcome (mRS after 6 m: r = - 0.3184, p = 0.0352). Systemic IL-8 correlated with impaired lung function (ECMO/ECLS: r = 0.3784, p = 0.0161) and neurological involvement (RASS mean: r = - 0.5132, p = 0.0007). IL-6 in BAL correlated better to the clinical course than systemic IL-6. Using three multivariate regression models, we describe prediction models for local and systemic damage as well as QoL. CO-Hb mean and max were associated with higher mortality.
Conclusions: Our predictive models using the combination of Charlson Comorbidity Index, sex, procalcitonin, systemic TLR3 expression and IL-6 and IL-8 in BAL were able to describe a broad range of clinically relevant outcomes in patients with severe COVID-19-associated ARDS. Using these models might proof useful in risk stratification and predicting disease course in the future. Trial registration The trial was registered with the German Clinical Trials Register (Trial-ID DRKS00021522, registered 22/04/2020).
Keywords: BAL; COVID-19; Carboxyhemoglobin; ICU; IL-6; IL-8; Outcome assessment; Quality of Life; TLR3.
© 2023. The Author(s).
Conflict of interest statement
NS received research support from the German Research Foundation (DFG). The remaining authors declare that they have no conflict of interest.
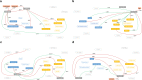
Figures




Similar articles
-
Safety and Efficacy of Imatinib for Hospitalized Adults with COVID-19: A structured summary of a study protocol for a randomised controlled trial.Trials. 2020 Oct 28;21(1):897. doi: 10.1186/s13063-020-04819-9. Trials. 2020. PMID: 33115543 Free PMC article.
-
Effect of dexamethasone in patients with ARDS and COVID-19 - prospective, multi-centre, open-label, parallel-group, randomised controlled trial (REMED trial): A structured summary of a study protocol for a randomised controlled trial.Trials. 2021 Mar 1;22(1):172. doi: 10.1186/s13063-021-05116-9. Trials. 2021. PMID: 33648568 Free PMC article.
-
[Changes in plasma interleukin-33 concentration in sepsis and its correlation with seriousness of sepsis].Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2015 Feb;27(2):138-42. doi: 10.3760/cma.j.issn.2095-4352.2015.02.012. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2015. PMID: 25665614 Chinese.
-
Strategies to DAMPen COVID-19-mediated lung and systemic inflammation and vascular injury.Transl Res. 2021 Jun;232:37-48. doi: 10.1016/j.trsl.2020.12.008. Epub 2020 Dec 20. Transl Res. 2021. PMID: 33358868 Free PMC article. Review.
-
Is it infection or rather vascular inflammation? Game-changer insights and recommendations from patterns of multi-organ involvement and affected subgroups in COVID-19.Cardiovasc Endocrinol Metab. 2020 Jun 11;9(3):110-120. doi: 10.1097/XCE.0000000000000211. eCollection 2020 Sep. Cardiovasc Endocrinol Metab. 2020. PMID: 32803145 Free PMC article. Review.
Cited by
-
Discovery, validation, and prodrug design of an ACE2 activator for treating bacterial infection-induced lung inflammation.J Control Release. 2023 Dec;364:1-11. doi: 10.1016/j.jconrel.2023.10.025. Epub 2023 Oct 21. J Control Release. 2023. PMID: 37858626 Free PMC article.
-
Research progress on the pathogenesis of AKI complicated by ECMO.Clin Exp Nephrol. 2025 Jan;29(1):10-20. doi: 10.1007/s10157-024-02559-7. Epub 2024 Sep 28. Clin Exp Nephrol. 2025. PMID: 39340702 Free PMC article. Review.
-
Multisystem Inflammatory Syndrome in an Adult on Hemodialysis with Markedly Elevated Procalcitonin and Ferritin Levels.Intern Med. 2023 Sep 1;62(17):2571-2575. doi: 10.2169/internalmedicine.1832-23. Epub 2023 Jun 21. Intern Med. 2023. PMID: 37344434 Free PMC article.
-
Stratification of COVID-19 Patients with Moderate-to-Severe Hypoxemic Respiratory Failure for Response to High-Flow Nasal Cannula: A Retrospective Observational Study.Medicina (Kaunas). 2023 Dec 29;60(1):71. doi: 10.3390/medicina60010071. Medicina (Kaunas). 2023. PMID: 38256332 Free PMC article.
-
Cytosolic nucleic acid sensing as driver of critical illness: mechanisms and advances in therapy.Signal Transduct Target Ther. 2025 Mar 19;10(1):90. doi: 10.1038/s41392-025-02174-2. Signal Transduct Target Ther. 2025. PMID: 40102400 Free PMC article. Review.
References
-
- WHO Coronavirus (COVID-19) Dashboard. https://covid19.who.int. Accessed 24th September 2022.
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials

