Neuromodulation in patients with refractory angina pectoris: a review
- PMID: 36632476
- PMCID: PMC9825802
- DOI: 10.1093/ehjopen/oeac083
Neuromodulation in patients with refractory angina pectoris: a review
Abstract
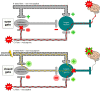
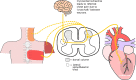
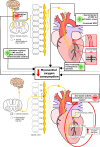
The number of patients with coronary artery disease (CAD) who have persisting angina pectoris despite optimal medical treatment known as refractory angina pectoris (RAP) is growing. Current estimates indicate that 5-10% of patients with stable CAD have RAP. In absolute numbers, there are 50 000-100 000 new cases of RAP each year in the USA and 30 000-50 000 new cases each year in Europe. The term RAP was formulated in 2002. RAP is defined as a chronic disease (more than 3 months) characterized by diffuse CAD in the presence of proven ischaemia which is not amendable to a combination of medical therapy, angioplasty, or coronary bypass surgery. There are currently few treatment options for patients with RAP. One such last-resort treatment option is spinal cord stimulation (SCS) with a Class of recommendation IIB, level of evidence B in the 2019 European Society of Cardiology guidelines for the diagnosis and management of chronic coronary syndromes. The aim of this review is to give an overview of neuromodulation as treatment modality for patients with RAP. A comprehensive overview is given on the history, proposed mechanism of action, safety, efficacy, and current use of SCS.
Keywords: Coronary artery disease; Refractory angina pectoris; Spinal cord stimulation.
© The Author(s) 2022. Published by Oxford University Press on behalf of the European Society of Cardiology.
Conflict of interest statement
Conflict of interest: No conflict of interest to declare.
Figures






References
-
- Mannheimer C, Camici P, Chester MR, Collins A, DeJongste M, Eliasson T, Follath F, Hellemans I, Herlitz J, Lüscher T, Pasic M, Thelle D. The problem of chronic refractory angina. Report from the ESC joint study group on the treatment of refractory angina. Eur Heart J 2002;23:355–370. - PubMed
-
- Henry TD, Satran D, Jolicoeur EM. Treatment of refractory angina in patients not suitable for revascularization. Nat Rev Cardiol 2013;11:78–95. - PubMed
-
- Riley RF, Kereiakes DJ, Henry TD. More data than options for the “no-option” refractory angina patient in the United States. Circ Res 2019;124:1689–1691. - PubMed
-
- Knuuti J, Wijns W, Saraste A, Capodanno D, Barbato E, Funck-Brentano C, Prescott E, Storey RF, Deaton C, Cuisset T, Agewall S, Dickstein K, Edvardsen T, Escaned J, Gersh BJ, Svitil P, Gilard M, Hasdai D, Hatala R, Mahfoud F, Masip J, Muneretto C, Valgimigli M, Achenbach S, Bax JJ, Group ESD, Neumann F-J, Sechtem U, Banning AP, Bonaros N, Bueno H, Bugiardini R, Chieffo A, Crea F, Czerny M, Delgado V, Dendale P, Flachskampf FA, Gohlke H, Grove EL, James S, Katritsis D, Landmesser U, Lettino M, Matter CM, Nathoe H, Niessner A, Patrono C, Petronio AS, Pettersen SE, Piccolo R, Piepoli MF, Popescu BA, Räber L, Richter DJ, Roffi M, Roithinger FX, Shlyakhto E, Sibbing D, Silber S, Simpson IA, Sousa-Uva M, Vardas P, Witkowski A, Zamorano JL, Achenbach S, Agewall S, Barbato E, Bax JJ, Capodanno D, Cuisset T, Deaton C, Dickstein K, Edvardsen T, Escaned J, Funck-Brentano C, Gersh BJ, Gilard M, Hasdai D, Hatala R, Mahfoud F, Masip J, Muneretto C, Prescott E, Saraste A, Storey RF, Svitil P, Valgimigli M, Windecker S, Aboyans V, Baigent C, Collet J-P, Dean V, Delgado V, Fitzsimons D, Gale CP, Grobbee D, Halvorsen S, Hindricks G, Iung B, Jüni P, Katus HA, Landmesser U, Leclercq C, Lettino M, Lewis BS, Merkely B, Mueller C, Petersen S, Petronio AS, Richter DJ, Roffi M, Shlyakhto E, Simpson IA, Sousa-Uva M, Touyz RM, Benkhedda S, Metzler B, Sujayeva V, Cosyns B, Kusljugic Z, Velchev V, Panayi G, Kala P, Haahr-Pedersen SA, Kabil H, Ainla T, Kaukonen T, Cayla G, Pagava Z, Woehrle J, Kanakakis J, Tóth K, Gudnason T, Peace A, Aronson D, Riccio C, Elezi S, Mirrakhimov E, Hansone S, Sarkis A, Babarskiene R, Beissel J, Maempel AJC, Revenco V, de Grooth GJ, Pejkov H, Juliebø V, Lipiec P, Santos J, Chioncel O, Duplyakov D, Bertelli L, Dikic AD, Studenčan M, Bunc M, Alfonso F, Bäck M, Zellweger M, Addad F, Yildirir A, Sirenko Y, Clapp B. 2019 ESC guidelines for the diagnosis and management of chronic coronary syndromes. Eur Heart J 2020;41:407–477. - PubMed
-
- Thomson S. Neuromodulation, or neuromodulatory effect 2013. https://www.neuromodulation.com/Neuromodulation-Defined
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

