Tracking excess of maternal deaths associated with COVID-19 in Brazil: a nationwide analysis
- PMID: 36635674
- PMCID: PMC9835215
- DOI: 10.1186/s12884-022-05338-y
Tracking excess of maternal deaths associated with COVID-19 in Brazil: a nationwide analysis
Abstract
Background: The COVID-19 pandemic brought a new challenge to maternal mortality in Brazil. Throughout 2020, Brazil registered 549 maternal deaths, mainly in second and third-trimester pregnant women. The objective of this study was to estimate the excess maternal deaths in Brazil caused directly and indirectly by Covid-19 in the year 2020. In addition, we sought to identify clinical, social and health care factors associated with the direct maternal deaths caused by Covid-19.
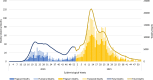
Methods: We performed nationwide analyses based on data from the Mortality Information System (SIM) for general and maternal deaths and the Influenza Epidemiological Surveillance System (SIVEP-Influenza) for estimates of female and maternal deaths due to COVID-19. Two distinct techniques were adopted. First, we describe maternal deaths directly caused by covid-19 and compare them with the historical series of deaths from covid-19 among women of childbearing age (15 to 49 years). Next, we estimated the total excess maternal mortality. Then, we calculated odds ratios for symptoms, comorbidities, social determination proxies and hospital care aspects between COVID-19 maternal deaths and deaths of women of childbearing age who were not pregnant or no maternal deaths. We chose women of childbearing age (15 to 49 years) as a reference because sex and age introduce differentials in the risk of COVID-19 death.
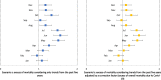
Results: Most maternal deaths occurred during pregnancy compared to postpartum deaths month by month in 2020 (μ = 59.8%, SD = 14.3%). The excess maternal mortality in 2020 in Brazil was 1.40 (95% CI 1.35-1.46). Even considering excess mortality due to COVID-19 for the childbearing age female population (MMR 1.14; 95% CI 1.13-1.15), maternal mortality exceeded the expected number. The odds of being a black woman, living in a rural area and being hospitalized outside the residence municipality among maternal deaths were 44, 61 and 28% higher than the control group. Odds of hospitalization (OR 4.37; 95% CI 3.39-5.37), ICU admission (OR 1.73; 95% CI 1.50-1.98) and invasive ventilatory support use (OR 1.64; CI 95% 1.42-1.86) among maternal deaths were higher than in the control group.
Conclusions: There was excess maternal mortality in 2020 in Brazil. Even with adjustment for the expected excess mortality from Covid-19 in women of childbearing age, the number of maternal deaths exceeds expectations, suggesting that there were deaths among pregnant and postpartum women indirectly caused by the pandemic, compromising access to prenatal care., adequate childbirth and puerperium.
Keywords: Brazil; COVID-19, SARS-CoV2; Maternal mortality.
© 2023. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
References
-
- WHO, UNICEF, UNFPA. UNICEF data warehouse: maternal mortality ratio, Brazil. Available at https://data.unicef.org/resources/data_explorer/unicef_f/?ag=UNICEF&df=G...
-
- Takemoto MLS, Menezes MO, Andreucci CB, Knobel R, Sousa LAR, Katz L, et al. Maternal mortality and COVID-19. J Matern Fetal Neonatal Med. 2020;16:1–7. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous