Cognitive behavior therapy vs. control conditions, other psychotherapies, pharmacotherapies and combined treatment for depression: a comprehensive meta-analysis including 409 trials with 52,702 patients
- PMID: 36640411
- PMCID: PMC9840507
- DOI: 10.1002/wps.21069
Cognitive behavior therapy vs. control conditions, other psychotherapies, pharmacotherapies and combined treatment for depression: a comprehensive meta-analysis including 409 trials with 52,702 patients
Abstract
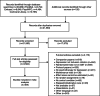
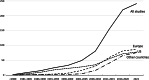
Cognitive behavior therapy (CBT) is by far the most examined type of psychological treatment for depression and is recommended in most treatment guide-lines. However, no recent meta-analysis has integrated the results of randomized trials examining its effects, and its efficacy in comparison with other psychotherapies, pharmacotherapies and combined treatment for depression remains uncertain. We searched PubMed, PsycINFO, Embase and the Cochrane Library to identify studies on CBT, and separated included trials into several subsets to conduct random-effects meta-analyses. We included 409 trials (518 comparisons) with 52,702 patients, thus conducting the largest meta-analysis ever of a specific type of psychotherapy for a mental disorder. The quality of the trials was found to have increased significantly over time (with increasing numbers of trials with low risk of bias, less waitlist control groups, and larger sample sizes). CBT had moderate to large effects compared to control conditions such as care as usual and waitlist (g=0.79; 95% CI: 0.70-0.89), which remained similar in sensitivity analyses and were still significant at 6-12 month follow-up. There was no reduction of the effect size of CBT according to the publication year (<2001 vs. 2001-2010 vs. >2011). CBT was significantly more effective than other psychotherapies, but the difference was small (g=0.06; 95% CI: 0-0.12) and became non-significant in most sensitivity analyses. The effects of CBT did not differ significantly from those of pharmacotherapies at the short term, but were significantly larger at 6-12 month follow-up (g=0.34; 95% CI: 0.09-0.58), although the number of trials was small, and the difference was not significant in all sensitivity analyses. Combined treatment was more effective than pharmacotherapies alone at the short (g=0.51; 95% CI: 0.19-0.84) and long term (g=0.32; 95% CI: 0.09-0.55), but it was not more effective than CBT alone at either time point. CBT was also effective as unguided self-help intervention (g=0.45; 95% CI: 0.31-0.60), in institutional settings (g=0.65; 95% CI: 0.21-1.08), and in children and adolescents (g=0.41; 95% CI: 0.25-0.57). We can conclude that the efficacy of CBT in depression is documented across different formats, ages, target groups, and settings. However, the superiority of CBT over other psychotherapies for depression does not emerge clearly from this meta-analysis. CBT appears to be as effective as pharmacotherapies at the short term, but more effective at the longer term.
Keywords: Depression; Internet-based interventions; antidepressants; cognitive behavior therapy; combined treatment; meta-analysis; psychotherapies.
© 2023 World Psychiatric Association.
Figures
References
-
- World Health Organization . World mental health report: transforming mental health for all. Geneva: World Health Organization, 2022.
-
- Herrman H, Patel V, Kieling C et al. Time for united action on depression: a Lancet‐World Psychiatric Association Commission. Lancet 2022;399:957‐1022. - PubMed
-
- Cuijpers P, Vogelzangs N, Twisk J et al. Comprehensive meta‐analysis of excess mortality in depression in the general community versus patients with specific illnesses. Am J Psychiatry 2014;171:453‐62. - PubMed
-
- Chisholm D, Sweeny K, Sheehan P et al. Scaling‐up treatment of depression and anxiety: a global return on investment analysis. Lancet Psychiatry 2016;3:415‐24. - PubMed
LinkOut - more resources
Full Text Sources
Medical