Kimura's disease: A clinicopathological study of 23 cases
- PMID: 36643844
- PMCID: PMC9835107
- DOI: 10.3389/fmed.2022.1069102
Kimura's disease: A clinicopathological study of 23 cases
Abstract
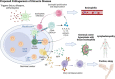
Introduction: Kimura's disease (KD) is an uncommon lymphoproliferative fibroinflammatory disorder. Patients present with head and neck subcutaneous nodules with or without lymphadenopathy. Peripheral blood eosinophilia and elevated serum immunoglobulin E (IgE) levels are typical. This study was designed to delineate the clinicopathological features, pattern of care, and disease course of 23 Taiwanese patients with KD.
Methods: We retrospectively analyzed the clinical data of 23 consecutive cases (16 male and 7 female; age at diagnosis: 12-77 years) of KD diagnosed at our institution from 2015 to 2020.
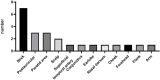
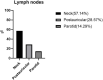
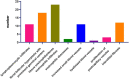
Results: The median time from presentation to diagnosis was 1 month. Twenty-one patients presented with unilateral or bilateral head and neck masses. The remaining two presented with right flank and right arm lesions, respectively. Peripheral blood eosinophilia was observed in nine, and elevated IgE levels were observed in four. All were diagnosed using either excisional or core-needle biopsy. Seven patients underwent fine needle aspiration without a diagnostic yield. Salivary gland and lymph node involvement was observed in three and seven patients, respectively. Most lesions showed tissue eosinophilia (100%) and florid follicular hyperplasia (78.26%). Three cases had histological KD-IgG4-RD overlap and three had comorbid IgG4-RD were recognized. Thirteen patients underwent surgical resection, one received adjuvant therapy, and two received prednisolone monotherapy.
Conclusion: KD should be considered in patients with subcutaneous masses, eosinophilia, and elevated IgE levels. Biopsy remains the gold standard of diagnosis. Increased recruitment of IgG4+ plasma cells is a common feature. Consideration of IgG4-RD in all KD patients may be prudent.
Keywords: IgG4-related disease; Kimura’s disease; Taiwan; eosinophilia; pathology.
Copyright © 2022 Lee, Yu and Chan.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
-
- Kimm H, Szeto C. Eosinophilic hyperplastic lymphogranuloma, comparison with Mikulicz’s disease. Proc Chin Med Soc. (1937) 1:329.
-
- Kimura T, Yoshimura S, Ishikawa E. On the unusual granulation combined with hyperplastic changes of lymphatic tissues. Trans Soc Pathol Jpn. (1948) 37:179–80.
-
- King R, Tan B, Craig F, George T, Horny H, Kelemen K, et al. Reactive eosinophil proliferations in tissue and the lymphocytic variant of hypereosinophilic syndrome: 2019 society for hematopathology/European association for haematopathology workshop report. Am J Clin Pathol. (2020) 155:211–38. 10.1093/ajcp/aqaa227 - DOI - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

