Perioperative changes in fluid distribution and haemodynamics in acute high-risk abdominal surgery
- PMID: 36647120
- PMCID: PMC9841944
- DOI: 10.1186/s13054-023-04309-9
Perioperative changes in fluid distribution and haemodynamics in acute high-risk abdominal surgery
Abstract
Background: Understanding the pathophysiology of fluid distribution in acute high-risk abdominal (AHA) surgery is essential in optimizing fluid management. There is currently no data on the time course and haemodynamic implications of fluid distribution in the perioperative period and the differences between the surgical pathologies.
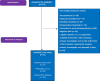
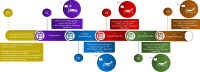
Methods: Seventy-three patients undergoing surgery for intestinal obstruction, perforated viscus, and anastomotic leakage within a well-defined perioperative regime, including intraoperative goal-directed therapy, were included in this prospective, observational study. From 0 to 120 h, we measured body fluid volumes and hydration status by bioimpedance spectroscopy (BIA), fluid balance (input vs. output), preload dependency defined as a > 10% increase in stroke volume after preoperative fluid challenge, and post-operatively evaluated by passive leg raise.
Results: We observed a progressive increase in fluid balance and extracellular volume throughout the study, irrespective of surgical diagnosis. BIA measured variables indicated post-operative overhydration in 36% of the patients, increasing to 50% on the 5th post-operative day, coinciding with a progressive increase of preload dependency, from 12% immediately post-operatively to 58% on the 5th post-operative day and irrespective of surgical diagnosis. Patients with overhydration were less haemodynamically stable than those with normo- or dehydration.
Conclusion: Despite increased fluid balance and extracellular volumes, preload dependency increased progressively during the post-operative period. Our observations indicate a post-operative physiological incoherence between changes in the extracellular volume compartment and inadequate physiological preload control in patients undergoing AHA surgery. Considering the increasing overhydration during the observational period, our findings show that an indiscriminate correction of preload dependency with intravenous fluid bolus could lead to overhydration. Trial registration clinicaltrials.gov. (NCT03997721), Registered 23 May 2019, first participant enrolled 01 June 2019.
Keywords: Emergency laparotomy; Fluid administration; Goal-directed therapy; Haemodynamics; Overhydration; Preload dependency.
© 2023. The Author(s).
Conflict of interest statement
All authors declare no competing interests related to the submitted work.
Figures


References
-
- Malbrain MLNG, Marik PE, Witters I, Cordemans C, Kirkpatrick AW, Roberts DJ, et al. Fluid overload, de-resuscitation, and outcomes in critically ill or injured patients: a systematic review with suggestions for clinical practice. Anaesthesiol Intensive Ther. 2014;46:361–380. doi: 10.5603/AIT.2014.0060. - DOI - PubMed
-
- Edwards MR, Forbes G, MacDonald N, Berdunov V, Mihaylova B, Dias P, et al. Optimisation of perioperative cardiovascular management to improve surgical outcome II (OPTIMISE II) trial: study protocol for a multicentre international trial of cardiac output-guided fluid therapy with low-dose inotrope infusion compared with usual car. BMJ Open. 2019;9:e023455. doi: 10.1136/bmjopen-2018-023455. - DOI - PMC - PubMed
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Medical

