Interrelation between miRNAs Expression Associated with Redox State Fluctuations, Immune and Inflammatory Response Activation, and Neonatal Outcomes in Complicated Pregnancy, Accompanied by Placental Insufficiency
- PMID: 36670868
- PMCID: PMC9854567
- DOI: 10.3390/antiox12010006
Interrelation between miRNAs Expression Associated with Redox State Fluctuations, Immune and Inflammatory Response Activation, and Neonatal Outcomes in Complicated Pregnancy, Accompanied by Placental Insufficiency
Abstract
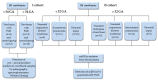
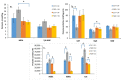
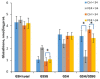
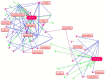
Redox disbalance in placental cells leads to the hyperproduction of reactive oxygen species (ROS), it mediates the dysregulation of the maternal immune tolerance to a semi-allogenic fetus, inducing pro-inflammatory reactions, and it plays a central role in perinatal complications and neonatal disease programming. Microvesicles, which provide transplacental communication between a mother and fetus, contain microRNAs (miRNAs) that are sensitive to oxidative stress (OS) mediators and can control the balance of ROS production and utilization in target cells. In the context of this paradigm, we evaluated the markers of redox balance—MDA and 4-HNE for OS and GPx, and SOD, CAT, and GSH for the antioxidant system in the cord blood plasma of newborns diagnosed with fetal growth restriction (FGR)—by using polarography, spectrophotometry, and Western blotting. The expression of miRNAs associated with OS, immune and inflammatory responses in the blood plasma of newborns with intrauterine pneumonia (IP), neonatal sepsis (NS) and respiratory distress syndrome (RDS) was evaluated by a quantitative RT-PCR. Significant differences in the MDA level and reduced GPx and CAT activity were co-found for early-onset FGR (i.e., <34 gestational age). Significant correlations were found with a low birth weight by Apgar scores with reduced levels of antioxidant enzymes. Indeed, the level of OS markers increased in early-onset FGR in newborns with an extremely low body weight and high echogenicity of the periventricular zones, and reduced in late-onset FGR in newborns with IP, hyperbilirubinemia, intraventricular hemorrhage (IVH) and cerebral cysts. A prognostic model (AUC = 1; cutoff—0.5) was developed to assess the risk of IVH in newborns diagnosed with FGR based on the assessment of the OS markers (i.e., MDA + 4 HNE + CAT + GSH). A significant increase in the miR-127-3p expression was found in the plasma of newborns with NS (<32 GA; p ≤ 0.03 and >32 GA; p ≤ 0.009), IP (>32 GA; p ≤ 0.0001), and RDS (>32 GA; p ≤ 0.03). At the same time, the expression of miR-25-3p (p ≤ 0.03) was increased only in newborns with NS (>32 GA; p ≤ 0.03). The risk of developing IVH for premature newborns with IP (AUC = 0.8; cutoff—0.6) and NS (AUC = 0.68; cutoff—0.49) was assessed based on the miR-25-3p and miR-127-3p expression. Several key transcription factors were identified as the targets of studied miRNA since they are involved in the regulation of OS (NRF2), signaling and activation of the immune response (PRDM1, CCL26) and, also, inflammatory responses (NFKB1). The study of these miRNAs showed that they are involved in the modulation of processes leading to perinatal complications. Moreover, miR-127-3p is related to pro-inflammatory reactions and the formation of the macrophage phenotype in newborns with IP, NS, and RDS, while miR-25-3p is associated with an inhibition of macrophage migration and activation of antioxidant enzymes, which may prevent the development of oxidative damage in newborns with NS.
Keywords: immune response; inflammatory; microRNA/miRNA; newborn; oxidative stress; perinatal outcomes; placental dysfunction.
Conflict of interest statement
The authors declare no conflict of interest.
Figures


Similar articles
-
MiRNAs Regulating Oxidative Stress: A Correlation with Doppler Sonography of Uteroplacental Complex and Clinical State Assessments of Newborns in Fetal Growth Restriction.J Clin Med. 2020 Oct 8;9(10):3227. doi: 10.3390/jcm9103227. J Clin Med. 2020. PMID: 33050114 Free PMC article.
-
Vaginal miR-210-3p as a potential biomarker for pregnancies complicated by early fetal growth restriction: A proof-of-concept case-control study.Placenta. 2025 Apr;163:8-15. doi: 10.1016/j.placenta.2025.02.015. Epub 2025 Feb 25. Placenta. 2025. PMID: 40023010
-
Increased Levels of hsa-miR-199a-3p and hsa-miR-382-5p in Maternal and Neonatal Blood Plasma in the Case of Placenta Accreta Spectrum.Int J Mol Sci. 2024 Dec 11;25(24):13309. doi: 10.3390/ijms252413309. Int J Mol Sci. 2024. PMID: 39769074 Free PMC article.
-
Risk of Respiratory Distress Syndrome and Efficacy of Glucocorticoids: Are They the Same in the Normally Grown and Growth-Restricted Infant?Reprod Sci. 2016 Nov;23(11):1459-1472. doi: 10.1177/1933719116660842. Epub 2016 Aug 22. Reprod Sci. 2016. PMID: 27549917 Review.
-
Consequences of early-onset preeclampsia on neonatal morbidity and mortality.Minerva Pediatr (Torino). 2023 Feb;75(1):87-97. doi: 10.23736/S2724-5276.22.06714-3. Epub 2022 Apr 4. Minerva Pediatr (Torino). 2023. PMID: 35373936 Review.
Cited by
-
Preeclampsia as a Study Model for Aging: The Klotho Gene Paradigm.Int J Mol Sci. 2025 Jan 22;26(3):902. doi: 10.3390/ijms26030902. Int J Mol Sci. 2025. PMID: 39940672 Free PMC article. Review.
-
Regulation of ferroptosis in osteoarthritis and osteoarthritic chondrocytes by typical MicroRNAs in chondrocytes.Front Med (Lausanne). 2024 Nov 5;11:1478153. doi: 10.3389/fmed.2024.1478153. eCollection 2024. Front Med (Lausanne). 2024. PMID: 39564502 Free PMC article. Review.
-
Decidual macrophages and Hofbauer cells in fetal growth restriction.Front Immunol. 2024 Jun 28;15:1379537. doi: 10.3389/fimmu.2024.1379537. eCollection 2024. Front Immunol. 2024. PMID: 39007150 Free PMC article. Review.
-
Analysis of lactate metabolism-related genes and their association with immune infiltration in septic shock via bioinformatics method.Front Genet. 2023 Jul 26;14:1223243. doi: 10.3389/fgene.2023.1223243. eCollection 2023. Front Genet. 2023. PMID: 37564869 Free PMC article.
References
-
- Ilekis J.V., Tsilou E., Fisher S., Abrahams V.M., Soares M.J., Cross J.C., Zamudio S., Illsley N.P., Myatt L., Colvis C., et al. Placental Origins of Adverse Pregnancy Outcomes: Potential Molecular Targets: An Executive Workshop Summary of the Eunice Kennedy Shriver National Institute of Child Health and Human Development. Am. J. Obstet. Gynecol. 2016;215:S1–S46. doi: 10.1016/j.ajog.2016.03.001. - DOI - PMC - PubMed
-
- Burton G.J., Yung H.-W., Cindrova-Davies T., Charnock-Jones D.S. Placental Endoplasmic Reticulum Stress and Oxidative Stress in the Pathophysiology of Unexplained Intrauterine Growth Restriction and Early Onset Preeclampsia. Placenta. 2009;30:43–48. doi: 10.1016/j.placenta.2008.11.003. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

