The Prognostic Value of the GNRI in Patients with Stomach Cancer Undergoing Surgery
- PMID: 36675816
- PMCID: PMC9861269
- DOI: 10.3390/jpm13010155
The Prognostic Value of the GNRI in Patients with Stomach Cancer Undergoing Surgery
Abstract
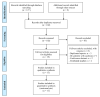
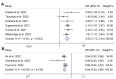
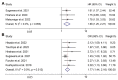
Malnutrition often induces an adverse prognosis in cancer surgery patients. The elderly nutrition risk index (GNRI) is an example of the objective indicators of nutrition-related risks. We performed a meta-analysis to thoroughly examine the evidence for the GNRI in predicting the outcomes of patients undergoing stomach cancer surgery. Eligible articles were retrieved using PubMed, the Cochrane Library, EMBASE, and Google Scholar by 24 October 2022. The clinical outcomes were overall survival (OS), cancer-specific survival (CSS), and post-operative complications. A total of 11 articles with 5593 patients were included in this meta-analysis. The combined forest plot showed that for every unit increase in the preoperative GNRI score in patients with stomach cancer, their postoperative mortality was reduced by 5.6% (HR: 0.944; 95% CI: 0.933−0.956, p < 0.001). The pooled results also demonstrated that a low GNRI was correlated with poor OS (HR: 2.052; 95% CI: 1.726−2.440, p < 0.001) and CSS (HR: 1.684; 95% CI: 1.249−2.270, p = 0.001) in patients who underwent stomach cancer surgery. Postoperative complications were more likely to occur in patients with a low GNRI, as opposed to those with a high GNRI (OR: 1.768; 95% CI: 1.445−2.163, p < 0.001). There was no evidence of significant heterogeneity, and the sensitivity analysis supported the stability and dependability of the above results. the GNRI is a valuable predictor of long-term outcomes and complications in stomach cancer patients undergoing surgery.
Keywords: geriatric nutritional risk index; meta-analysis; prognosis; stomach cancer; surgery.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures



Similar articles
-
Prediction of postoperative complications and survival after laparoscopic gastrectomy using preoperative Geriatric Nutritional Risk Index in elderly gastric cancer patients.Surg Endosc. 2021 Mar;35(3):1202-1209. doi: 10.1007/s00464-020-07487-7. Epub 2020 Mar 9. Surg Endosc. 2021. PMID: 32152675
-
Prognostic Value of Geriatric Nutritional Risk Index in Esophageal Carcinoma: A Systematic Review and Meta-Analysis.Front Nutr. 2022 Mar 25;9:831283. doi: 10.3389/fnut.2022.831283. eCollection 2022. Front Nutr. 2022. PMID: 35399659 Free PMC article.
-
Predictive Value of Geriatric Nutritional Risk Index in Patients with Colorectal Cancer: A Meta-Analysis.Nutr Cancer. 2023;75(1):24-32. doi: 10.1080/01635581.2022.2115521. Epub 2022 Aug 29. Nutr Cancer. 2023. PMID: 36039473
-
Predictive role of preoperative geriatric nutritional risk index for clinical outcomes in surgical gastric cancer patients: A meta-analysis.Front Surg. 2022 Nov 2;9:1020482. doi: 10.3389/fsurg.2022.1020482. eCollection 2022. Front Surg. 2022. PMID: 36406367 Free PMC article. Review.
-
Prognostic value of the geriatric nutritional index in colorectal cancer patients undergoing surgical intervention: A systematic review and meta-analysis.Front Oncol. 2022 Nov 23;12:1066417. doi: 10.3389/fonc.2022.1066417. eCollection 2022. Front Oncol. 2022. PMID: 36518324 Free PMC article.
Cited by
-
Prognostic and clinicopathological role of geriatric nutritional risk index in patients with diffuse large B-cell lymphoma: A meta-analysis.Front Oncol. 2023 Mar 30;13:1169749. doi: 10.3389/fonc.2023.1169749. eCollection 2023. Front Oncol. 2023. PMID: 37064090 Free PMC article.
-
Neutrophil-To-Lymphocyte Ratio as a Prognostic Indicator in Thyroid Cancer.Cancer Control. 2024 Jan-Dec;31:10732748241309048. doi: 10.1177/10732748241309048. Cancer Control. 2024. PMID: 39696882 Free PMC article.
-
CD19 (+) B Cell Combined with Prognostic Nutritional Index Predicts the Clinical Outcomes of Patients with Gastric Cancer Who Underwent Surgery.Cancers (Basel). 2023 Apr 28;15(9):2531. doi: 10.3390/cancers15092531. Cancers (Basel). 2023. PMID: 37173997 Free PMC article.
-
The geriatric nutritional risk index is related to adverse hospitalization outcomes in individuals undergoing cardiac surgery.Sci Rep. 2024 Aug 18;14(1):19126. doi: 10.1038/s41598-024-69668-x. Sci Rep. 2024. PMID: 39155300 Free PMC article.
-
Geriatric nutritional risk index as a predictor for postoperative complications in patients with solid cancers: a meta-analysis.Front Oncol. 2024 Feb 7;14:1266291. doi: 10.3389/fonc.2024.1266291. eCollection 2024. Front Oncol. 2024. PMID: 38384816 Free PMC article.
References
-
- Fukuda Y., Yamamoto K., Hirao M., Nishikawa K., Maeda S., Haraguchi N., Miyake M., Hama N., Miyamoto A., Ikeda M., et al. Prevalence of Malnutrition Among Gastric Cancer Patients Undergoing Gastrectomy and Optimal Preoperative Nutritional Support for Preventing Surgical Site Infections. Ann. Surg. Oncol. 2015;22((Suppl. 3)):S778–S785. doi: 10.1245/s10434-015-4820-9. - DOI - PubMed
Grants and funding
- No. 82172855, 81870442/grants from National Natural Science Foundation of China
- 2021CFB365/Natural Science Foundation of Hubei Province
- 2021JJ30419/Key Project of Natural Science Foundation of Hunan Province
- 2021017/Key Project of Scientific Research Foundation of Hunan Provincial Administration of Traditional Chinese Medicine
LinkOut - more resources
Full Text Sources

