Type 4 renal tubular acidosis and uric acid nephrolithiasis: two faces of the same coin?
- PMID: 36683539
- PMCID: PMC9881823
- DOI: 10.1097/MNH.0000000000000859
Type 4 renal tubular acidosis and uric acid nephrolithiasis: two faces of the same coin?
Abstract
Purpose of review: The present review summarizes findings of recent studies examining the epidemiology, pathophysiology, and treatment of type 4 renal tubular acidosis (RTA) and uric acid nephrolithiasis, two conditions characterized by an abnormally acidic urine.
Recent findings: Both type 4 RTA and uric acid nephrolithiasis disproportionately occur in patients with type 2 diabetes and/or chronic kidney disease. Biochemically, both conditions are associated with reduced renal ammonium excretion resulting in impaired urinary buffering and low urine pH. Reduced ammoniagenesis is postulated to result from hyperkalemia in type 4 RTA and from insulin resistance and fat accumulation in the renal proximal tubule in uric acid nephrolithiasis. The typical biochemical findings of hyperkalemia and systemic acidosis of type 4 RTA are rarely reported in uric acid stone formers. Additional clinical differences between the two conditions include findings of higher urinary uric acid excretion and consequent urinary uric acid supersaturation in uric acid stone formers but not in type 4 RTA.
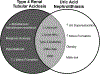
Summary: Type 4 RTA and uric acid nephrolithiasis share several epidemiological, clinical, and biochemical features. Although both conditions may be manifestations of diabetes mellitus and thus have a large at-risk population, the means to the shared biochemical finding of overly acidic urine are different. This difference in pathophysiology may explain the dissimilarity in the prevalence of kidney stone formation.
Copyright © 2022 Wolters Kluwer Health, Inc. All rights reserved.
Conflict of interest statement
Figures
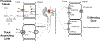
Similar articles
-
Uric acid stone disease: lessons from recent human physiologic studies.Curr Opin Nephrol Hypertens. 2020 Jul;29(4):407-413. doi: 10.1097/MNH.0000000000000610. Curr Opin Nephrol Hypertens. 2020. PMID: 32398609 Review.
-
Renal ammonium excretion after an acute acid load: blunted response in uric acid stone formers but not in patients with type 2 diabetes.Am J Physiol Renal Physiol. 2013 Nov 15;305(10):F1498-503. doi: 10.1152/ajprenal.00374.2013. Epub 2013 Sep 11. Am J Physiol Renal Physiol. 2013. PMID: 24026180 Free PMC article.
-
Renal tubular acidosis in recurrent renal stone formers.Eur Urol. 1984;10(1):55-9. doi: 10.1159/000463513. Eur Urol. 1984. PMID: 6698089
-
The syndrome of distal (type 1) renal tubular acidosis. Clinical and laboratory findings in 58 cases.Medicine (Baltimore). 1988 Mar;67(2):84-99. doi: 10.1097/00005792-198803000-00002. Medicine (Baltimore). 1988. PMID: 3127650
-
Metabolic syndrome and uric acid nephrolithiasis.Semin Nephrol. 2008 Mar;28(2):174-80. doi: 10.1016/j.semnephrol.2008.01.010. Semin Nephrol. 2008. PMID: 18359398 Review.
Cited by
-
Pediatric adrenocortical carcinoma complicated by uric acid nephrolithiasis: a unique case report.BMC Urol. 2025 Apr 30;25(1):109. doi: 10.1186/s12894-025-01801-y. BMC Urol. 2025. PMID: 40307791 Free PMC article.
References
-
- Wrong OM, Unwin RJ. Renal tubular acidosis: ‘RTA is no accident’. Clinical Medicine. 2012;12(Suppl 6):s22–s5.
-
- Batlle D, Arruda J. Hyperkalemic Forms of Renal Tubular Acidosis: Clinical and Pathophysiological Aspects. Adv Chronic Kidney Dis. 2018;25(4):321–33. - PubMed
-
- Karet FE. Mechanisms in hyperkalemic renal tubular acidosis. J Am Soc Nephrol. 2009;20(2):251–4. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

