Imaging patterns of wall thickening type of gallbladder cancer
- PMID: 36683868
- PMCID: PMC9850297
- DOI: 10.5114/ceh.2022.122285
Imaging patterns of wall thickening type of gallbladder cancer
Abstract
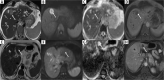
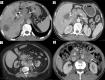
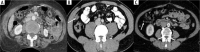
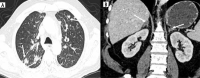
Gallbladder cancer (GBC) has a high incidence in certain geographical regions. Morphologically, GBC presents as a mass replacing the gallbladder, a polypoidal lesion, or wall thickening. The incidence of preoperative diagnosis of wall thickening type of GBC is less well studied. The patterns of mural involvement and extramural spread are not well described in the literature. Additionally, wall thickening in the gallbladder does not always indicate malignancy and can be secondary to inflammatory or benign gallbladder diseases and extracholecystic causes and systemic pathologies. Objective reporting of gallbladder wall thickening will help us appreciate GBC's early features. In this review, we illustrate the imaging patterns of wall thickening type of GBC.
Keywords: gallbladder; malignancy; wall thickening.
Copyright © 2022 Clinical and Experimental Hepatology.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

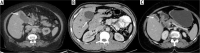
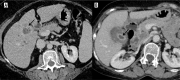
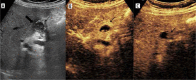
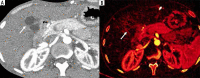
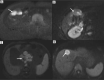
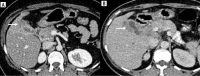

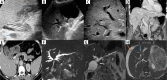
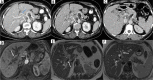
Similar articles
-
Update on the Role of Imaging in the Diagnosis, Staging, and Prognostication of Gallbladder Cancer.Indian J Radiol Imaging. 2024 Aug 26;35(2):218-233. doi: 10.1055/s-0044-1789243. eCollection 2025 Apr. Indian J Radiol Imaging. 2024. PMID: 40297115 Free PMC article. Review.
-
Imaging-based algorithmic approach to gallbladder wall thickening.World J Gastroenterol. 2020 Oct 28;26(40):6163-6181. doi: 10.3748/wjg.v26.i40.6163. World J Gastroenterol. 2020. PMID: 33177791 Free PMC article. Review.
-
Proposal for a new morphological "combined type" of gallbladder cancer: description of radiopathological characteristics and comparison with other morphological types.Abdom Radiol (NY). 2024 Mar;49(3):703-709. doi: 10.1007/s00261-023-04090-x. Epub 2023 Nov 16. Abdom Radiol (NY). 2024. PMID: 37973653
-
Role of dual energy computed tomography in evaluation of suspected wall thickening type of gallbladder cancer.Clin Exp Hepatol. 2022 Mar;8(1):92-95. doi: 10.5114/ceh.2022.114188. Epub 2022 Mar 23. Clin Exp Hepatol. 2022. PMID: 35415252 Free PMC article.
-
Gallbladder carcinoma: causes of misdiagnosis at CT.Clin Radiol. 2016 Jan;71(1):e96-109. doi: 10.1016/j.crad.2015.10.016. Epub 2015 Nov 18. Clin Radiol. 2016. PMID: 26602932 Review.
Cited by
-
Update on the Role of Imaging in the Diagnosis, Staging, and Prognostication of Gallbladder Cancer.Indian J Radiol Imaging. 2024 Aug 26;35(2):218-233. doi: 10.1055/s-0044-1789243. eCollection 2025 Apr. Indian J Radiol Imaging. 2024. PMID: 40297115 Free PMC article. Review.
-
Outcomes of Self-expandable Metal Stents in Patients With Unresectable Gallbladder Cancer Undergoing Percutaneous Biliary Drainage.J Clin Exp Hepatol. 2024 May-Jun;14(3):101348. doi: 10.1016/j.jceh.2024.101348. Epub 2024 Jan 27. J Clin Exp Hepatol. 2024. PMID: 38389867 Free PMC article.
-
Dual-energy CT in differentiating benign gallbladder wall thickening from wall thickening type of gallbladder cancer.Eur Radiol. 2025 Jan;35(1):84-92. doi: 10.1007/s00330-024-10904-3. Epub 2024 Jul 9. Eur Radiol. 2025. PMID: 38980414
-
Agreement of Gallbladder Reporting and Data System for Gallbladder Wall Thickening at Ultrasonography: A Multireader Validation Study.J Clin Exp Hepatol. 2024 Jul-Aug;14(4):101393. doi: 10.1016/j.jceh.2024.101393. Epub 2024 Mar 5. J Clin Exp Hepatol. 2024. PMID: 38550799 Free PMC article.
-
Aseptic Abscess of the Gallbladder Mimicking Gallbladder Carcinoma after Surgery for Ulcerative Colitis.Intern Med. 2025 Jul 1;64(13):1984-1992. doi: 10.2169/internalmedicine.4411-24. Epub 2024 Dec 5. Intern Med. 2025. PMID: 39631865 Free PMC article.
References
-
- Randi G, Franceschi S, La Vecchia C. Gallbladder cancer worldwide: Geographical distribution and risk factors. Int J Cancer 2006; 118: 1591-1602. - PubMed
-
- Amin MB, Edge SB, Greene FL, et al. . (Eds.). AJCC Cancer Staging Manual [Internet]. Springer International Publishing, Cham: 2017. (cited 2022 Jan 15). Available from: http://link.springer.com/10.1007/978-3-319-40618-3 - DOI
-
- Levy AD, Murakata LA, Rohrmann CA. Gallbladder carcinoma: radiologic-pathologic correlation. Radiographics 2001; 21: 295-314. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
