Spinal oncologic paraparesis: Analysis of neurological and surgical outcomes in patients with intramedullary, extramedullary, and extradural tumors
- PMID: 36686806
- PMCID: PMC9846080
- DOI: 10.3389/fonc.2022.1003084
Spinal oncologic paraparesis: Analysis of neurological and surgical outcomes in patients with intramedullary, extramedullary, and extradural tumors
Abstract
Objectives: Paraparesis due to oncologic lesions of the spine warrants swift neurosurgical intervention to prevent permanent disability and hence maintain independence of affected patients. Clinical parameters that predict a favorable outcome after surgical intervention could aid decision-making in emergency situations.
Methods: Patients who underwent surgical intervention for paraparesis (grade of muscle strength <5 according to the British Medical Research Council grading system) secondary to spinal neoplasms between 2006 and 2020 were included in a single-center retrospective analysis. Pre- and postoperative clinical data were collected. The neurological status was assessed using the modified McCormick Disability Scale (mMcC) Score. In a univariate analysis, patients with favorable (discharge mMcC improved or stable at <3) and non-favorable outcome (discharge mMcC deteriorated or stable at >2) and different tumor anatomical compartments were statistically compared.
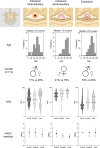
Results: 117 patients with oncologic paraparesis pertaining to intramedullary lesions (n=17, 15%), intradural extramedullary (n=24, 21%) and extradural lesions (n=76, 65%) with a mean age of 65.3 ± 14.6 years were included in the analysis. Thoracic tumors were the most common (77%), followed by lumbar and cervical tumors (13% and 12%, respectively). Surgery was performed within a mean of 36±60 hours of admission across all tumors and included decompression over a median of 2 segments (IQR:1-3) and mostly subtotal tumor resection (n=83, 71%). Surgical and medical complications were documented in 9% (n=11) and 7% (n=8) of cases, respectively. The median hospital length-of-stay was 9 (7-13) days. Upon discharge, the median mMcC score had improved from 3 to 2 (p<0.0001). At last follow-up (median 180; IQR 51-1080 days), patients showed an improvement in their mean Karnofsky Performance Score (KPS) from 51.7±18.8% to 65.3±20.4% (p<0.001). Localization in the intramedullary compartment, a high preoperative mMcC score, in addition to bladder and bowel dysfunction were associated with a non-favorable outcome (p<0.001).
Conclusion: The data presented on patients with spinal oncologic paraparesis provide a risk-benefit narrative that favors surgical intervention across all etiologies. At the same time, they outline clinical factors that confer a less-favorable outcome like intramedullary tumor localization, a high McCormick score and/or bladder and bowel abnormalities at admission.
Keywords: McCormick score; intramedullary tumors; paraparesis; spinal ependymomas; spinal metastases.
Copyright © 2023 Alhalabi, Heene, Landré, Neumann, Scherer, Ishak, Kiening, Zweckberger, Unterberg and Younsi.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
LinkOut - more resources
Full Text Sources

