Leukocyte Count and Coronary Artery Disease Events in People With Human Immunodeficiency Virus: A Longitudinal Study
- PMID: 36688465
- PMCID: PMC10249993
- DOI: 10.1093/cid/ciad033
Leukocyte Count and Coronary Artery Disease Events in People With Human Immunodeficiency Virus: A Longitudinal Study
Abstract
Background: People with human immunodeficiency virus (HIV; PWH) have increased cardiovascular risk. Higher leukocyte count has been associated with coronary artery disease (CAD) events in the general population. It is unknown whether the leukocyte-CAD association also applies to PWH.
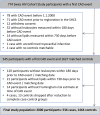
Methods: In a case-control study nested within the Swiss HIV Cohort Study, we obtained uni- and multivariable odds ratios (OR) for CAD events, based on traditional and HIV-related CAD risk factors, leukocyte count, and confounders previously associated with leukocyte count.
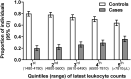
Results: We included 536 cases with a first CAD event (2000-2021; median age, 56 years; 87% male; 84% with suppressed HIV RNA) and 1464 event-free controls. Cases had higher latest leukocyte count before CAD event than controls (median [interquartile range], 6495 [5300-7995] vs 5900 [4910-7200]; P < .01), but leukocytosis (>11 000/µL) was uncommon (4.3% vs 2.1%; P = .01). In the highest versus lowest leukocyte quintile at latest time point before CAD event, participants had univariable CAD-OR = 2.27 (95% confidence interval, 1.63-3.15) and multivariable adjusted CAD-OR = 1.59 (1.09-2.30). For comparison, univariable CAD-OR for dyslipidemia, diabetes, and recent abacavir exposure were 1.58 (1.29-1.93), 2.19 (1.59-3.03), and 1.73 (1.37-2.17), respectively. Smoking and, to a lesser degree, alcohol and ethnicity attenuated the leukocyte-CAD association. Leukocytes measured up to 8 years before the event were significantly associated with CAD events.
Conclusions: PWH in Switzerland with higher leukocyte counts have an independently increased risk of CAD events, to a degree similar to traditional and HIV-related risk factors.
Keywords: HIV infection; coronary artery disease; leukocytes; multivariable analysis; white blood cells.
© The Author(s) 2023. Published by Oxford University Press on behalf of Infectious Diseases Society of America.
Conflict of interest statement
Potential conflicts of interest. B. L. received personal fees from Kantonsspital Baselland (for consultancy and statistical analyses), Liestal, Switzerland, during the conduct of the study, and reports personal fees from Gilead Switzerland SARL for lectures and ViiV for advisory board service, outside the submitted work. I. C. S.'s institution received a lecture fee from ViiV, outside the submitted work. P. R., through his institution, has received independent scientific grant support from Gilead, ViiV, Merck (all investigator-initiated study grants), and Janssen, honorarium paid to institution for lecture (content fully under author's control) from Merck & Co and has served on scientific advisory boards for Gilead, ViiV, and Merck, for which his institution has received remuneration. E. B. has received consulting fees from Gilead, MSD, ViiV, Pfizer, and AbbVie and travel support from Gilead, MSD, ViiV Healthcare, Abbvie, and Pfizer AG, and reports grants or contracts from Merck Sharp & Dohme and participation on a Data Safety Monitoring Board or Advisory Board with Merck Sharp & Dohme, Gilead Sciences, ViiV Healthcare, Pfizer AG, Ely Lilly, and Moderna, all paid to their institution and all outside the submitted work. D. L. B. received honoraria for advisory boards from Gilead, ViiV, and MSD and consulting fees from ViiV, Gilead, MSD, Pfizer, and Astra Zeneka. M. C. reports grants/support from Gilead, MSD, and ViiV, payment for expert testimony from Gilead, MSD, and ViiV, and travel support from Gilead, all paid to their institution and all outside the submitted work. R. K. reports grants/support from Gilead, paid to their institution, and grants or contracts from Swiss National Science Foundation, National Institutes of Health, outside the submitted work. H. F. G., outside this study, reports grants from Gilead (unrestricted research grant), the National Institutes of Health and the Yvonne Jacob Foundation (Swiss National Science Foundation, Swiss HIV Cohort Study), all paid to their institution; personal fees as an advisor/consultant for Merck, ViiV, and Gilead, and data and safety monitoring board remuneration from Merck, paid to their institution, and a travel grant from Gilead Sciences, paid to author, and paid participation on a Data Safety Monitoring Board or Advisory Board for Merck, Gilead Sciences, ViiV, Janssen, Johnson and Johnson, Novartis, and GSK, all outside the submitted work. P. E. T.'s institution reports unrestricted and educational grants from Gilead, ViiV, and MSD, and advisory fees from Gilead and ViiV, and payment or honoraria for lectures, presentations, speakers bureaus, manuscript writing or educational events from Gilead, ViiV, MSD, and Daiichi Sankyo, all outside the submitted work. C. M. reports speaker honoraria from MSD, ViiV, and Pfizer, unrelated to this work. All other authors report no potential conflicts. All authors have submitted the ICMJE Form for Disclosure of Potential Conflicts of Interest. Conflicts that the editors consider relevant to the content of the manuscript have been disclosed.
Figures


Similar articles
-
Telomere Length, Traditional Risk Factors, Factors Related to Human Immunodeficiency Virus (HIV) and Coronary Artery Disease Events in Swiss Persons Living With HIV.Clin Infect Dis. 2021 Oct 5;73(7):e2070-e2076. doi: 10.1093/cid/ciaa1034. Clin Infect Dis. 2021. PMID: 32725240
-
Coronary Artery Disease-Associated and Longevity-Associated Polygenic Risk Scores for Prediction of Coronary Artery Disease Events in Persons Living With Human Immunodeficiency Virus: The Swiss HIV Cohort Study.Clin Infect Dis. 2021 Nov 2;73(9):1597-1604. doi: 10.1093/cid/ciab521. Clin Infect Dis. 2021. PMID: 34091660
-
Polygenic Risk Scores for Prediction of Subclinical Coronary Artery Disease in Persons With Human Immunodeficiency Virus (HIV): The Swiss HIV Cohort Study.Clin Infect Dis. 2023 Jan 6;76(1):48-56. doi: 10.1093/cid/ciac758. Clin Infect Dis. 2023. PMID: 36097729
-
Contribution of genetic background, traditional risk factors, and HIV-related factors to coronary artery disease events in HIV-positive persons.Clin Infect Dis. 2013 Jul;57(1):112-21. doi: 10.1093/cid/cit196. Epub 2013 Mar 26. Clin Infect Dis. 2013. PMID: 23532479 Free PMC article.
-
Factors associated with the development of coronary artery disease in people with HIV.Sex Health. 2023 Oct;20(5):470-474. doi: 10.1071/SH23043. Sex Health. 2023. PMID: 37394729
Cited by
-
Accelerated aging in people living with HIV: The neuroimmune feedback model.Brain Behav Immun Health. 2024 Feb 5;36:100737. doi: 10.1016/j.bbih.2024.100737. eCollection 2024 Mar. Brain Behav Immun Health. 2024. PMID: 38356933 Free PMC article.
-
Types of Myocardial Infarction in People With HIV in Switzerland.Open Forum Infect Dis. 2025 Jun 19;12(7):ofaf357. doi: 10.1093/ofid/ofaf357. eCollection 2025 Jul. Open Forum Infect Dis. 2025. PMID: 40698031 Free PMC article.
References
-
- El-Sadr WM, Lundgren J, Neaton JD, et al. . CD4+ count-guided interruption of antiretroviral treatment. N Engl J Med 2006; 355:2283–96. - PubMed
-
- Lang S, Mary-Krause M, Simon A, et al. . HIV replication and immune status are independent predictors of the risk of myocardial infarction in HIV-infected individuals. Clin Infect Dis 2012; 55:600–7. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

