Validation of a deep-learning-based retinal biomarker (Reti-CVD) in the prediction of cardiovascular disease: data from UK Biobank
- PMID: 36691041
- PMCID: PMC9872417
- DOI: 10.1186/s12916-022-02684-8
Validation of a deep-learning-based retinal biomarker (Reti-CVD) in the prediction of cardiovascular disease: data from UK Biobank
Abstract
Background: Currently in the United Kingdom, cardiovascular disease (CVD) risk assessment is based on the QRISK3 score, in which 10% 10-year CVD risk indicates clinical intervention. However, this benchmark has limited efficacy in clinical practice and the need for a more simple, non-invasive risk stratification tool is necessary. Retinal photography is becoming increasingly acceptable as a non-invasive imaging tool for CVD. Previously, we developed a novel CVD risk stratification system based on retinal photographs predicting future CVD risk. This study aims to further validate our biomarker, Reti-CVD, (1) to detect risk group of ≥ 10% in 10-year CVD risk and (2) enhance risk assessment in individuals with QRISK3 of 7.5-10% (termed as borderline-QRISK3 group) using the UK Biobank.
Methods: Reti-CVD scores were calculated and stratified into three risk groups based on optimized cut-off values from the UK Biobank. We used Cox proportional-hazards models to evaluate the ability of Reti-CVD to predict CVD events in the general population. C-statistics was used to assess the prognostic value of adding Reti-CVD to QRISK3 in borderline-QRISK3 group and three vulnerable subgroups.
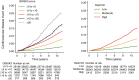
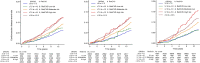
Results: Among 48,260 participants with no history of CVD, 6.3% had CVD events during the 11-year follow-up. Reti-CVD was associated with an increased risk of CVD (adjusted hazard ratio [HR] 1.41; 95% confidence interval [CI], 1.30-1.52) with a 13.1% (95% CI, 11.7-14.6%) 10-year CVD risk in Reti-CVD-high-risk group. The 10-year CVD risk of the borderline-QRISK3 group was greater than 10% in Reti-CVD-high-risk group (11.5% in non-statin cohort [n = 45,473], 11.5% in stage 1 hypertension cohort [n = 11,966], and 14.2% in middle-aged cohort [n = 38,941]). C statistics increased by 0.014 (0.010-0.017) in non-statin cohort, 0.013 (0.007-0.019) in stage 1 hypertension cohort, and 0.023 (0.018-0.029) in middle-aged cohort for CVD event prediction after adding Reti-CVD to QRISK3.
Conclusions: Reti-CVD has the potential to identify individuals with ≥ 10% 10-year CVD risk who are likely to benefit from earlier preventative CVD interventions. For borderline-QRISK3 individuals with 10-year CVD risk between 7.5 and 10%, Reti-CVD could be used as a risk enhancer tool to help improve discernment accuracy, especially in adult groups that may be pre-disposed to CVD.
Keywords: Artificial intelligence; Cardiovascular disease; Deep learning; Retinal imaging; Retinal photograph; Risk stratification; Risk stratification system; UK Biobank.
© 2023. The Author(s).
Conflict of interest statement
T.H.R. was a former scientific adviser and owns stock of Mediwhale Inc. H.K. and G.L. are employees of Mediwhale Inc. T.H.R. and G.L. hold the following patents that might be affected by this study: 10–2018–0166720(KR), 10–2018–0166721(KR), 10–2018–0166722(KR), 62/694,901(US), 62/715,729(US), and 62/776,345 (US). All other authors declare no competing interests.
Figures
Similar articles
-
Pivotal trial of a deep-learning-based retinal biomarker (Reti-CVD) in the prediction of cardiovascular disease: data from CMERC-HI.J Am Med Inform Assoc. 2023 Dec 22;31(1):130-138. doi: 10.1093/jamia/ocad199. J Am Med Inform Assoc. 2023. PMID: 37847669 Free PMC article.
-
Cardiovascular disease risk assessment using a deep-learning-based retinal biomarker: a comparison with existing risk scores.Eur Heart J Digit Health. 2023 Mar 28;4(3):236-244. doi: 10.1093/ehjdh/ztad023. eCollection 2023 May. Eur Heart J Digit Health. 2023. PMID: 37265875 Free PMC article.
-
Independent external validation of the QRISK3 cardiovascular disease risk prediction model using UK Biobank.Heart. 2023 Oct 26;109(22):1690-1697. doi: 10.1136/heartjnl-2022-321231. Heart. 2023. PMID: 37423742 Free PMC article.
-
Development and Validation of Risk Scores for All-Cause Mortality for a Smartphone-Based "General Health Score" App: Prospective Cohort Study Using the UK Biobank.JMIR Mhealth Uhealth. 2021 Feb 16;9(2):e25655. doi: 10.2196/25655. JMIR Mhealth Uhealth. 2021. PMID: 33591285 Free PMC article. Review.
-
United Kingdom Biobank (UK Biobank): JACC Focus Seminar 6/8.J Am Coll Cardiol. 2021 Jul 6;78(1):56-65. doi: 10.1016/j.jacc.2021.03.342. J Am Coll Cardiol. 2021. PMID: 34210415 Review.
Cited by
-
Machine learning-based prediction model for myocardial ischemia under high altitude exposure: a cohort study.Sci Rep. 2024 Jan 6;14(1):686. doi: 10.1038/s41598-024-51202-8. Sci Rep. 2024. PMID: 38182722 Free PMC article.
-
Standardization and clinical applications of retinal imaging biomarkers for cardiovascular disease: a Roadmap from an NHLBI workshop.Nat Rev Cardiol. 2025 Jan;22(1):47-63. doi: 10.1038/s41569-024-01060-8. Epub 2024 Jul 22. Nat Rev Cardiol. 2025. PMID: 39039178 Review.
-
Pivotal trial of a deep-learning-based retinal biomarker (Reti-CVD) in the prediction of cardiovascular disease: data from CMERC-HI.J Am Med Inform Assoc. 2023 Dec 22;31(1):130-138. doi: 10.1093/jamia/ocad199. J Am Med Inform Assoc. 2023. PMID: 37847669 Free PMC article.
-
Prognostic potentials of AI in ophthalmology: systemic disease forecasting via retinal imaging.Eye Vis (Lond). 2024 May 6;11(1):17. doi: 10.1186/s40662-024-00384-3. Eye Vis (Lond). 2024. PMID: 38711111 Free PMC article. Review.
-
Real-world feasibility, accuracy and acceptability of automated retinal photography and AI-based cardiovascular disease risk assessment in Australian primary care settings: a pragmatic trial.NPJ Digit Med. 2025 Feb 24;8(1):122. doi: 10.1038/s41746-025-01436-1. NPJ Digit Med. 2025. PMID: 39994433 Free PMC article.
References
-
- Cardiovascular disease: risk assessment and reduction, including lipid modification [https://www.nice.org.uk/guidance/cg181/resources]. 2014. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

