Effectiveness, complications, and reproductive outcomes after cesarean scar pregnancy management: a retrospective cohort study
- PMID: 36691399
- PMCID: PMC9860491
- DOI: 10.1016/j.xagr.2022.100143
Effectiveness, complications, and reproductive outcomes after cesarean scar pregnancy management: a retrospective cohort study
Abstract
Background: There is a dramatic rise in cesarean deliveries worldwide, leading to higher complication rates in subsequent pregnancies. One of these complications is a cesarean scar pregnancy. During the last decades, treatment options for cesarean scar pregnancies have changed, and less invasive interventions have been employed to preserve fertility and reduce morbidity. However, the optimal treatment approach and the influence of various treatments on reproductive outcomes have to be determined.
Objective: This study aimed to evaluate the short- and long-term outcomes after cesarean scar pregnancy management.
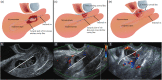
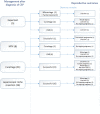
Study design: We conducted a retrospective cohort study of women determined to have a cesarean scar pregnancy from 2010 to 2021 at a tertiary referral center, the Amsterdam University Medical Center, in the Netherlands. Outcomes of the following management strategies were compared: expectant management, methotrexate, curettage with temporary cervical cerclage, or a laparoscopic niche resection. We performed a curettage if the cesarean scar pregnancy did not cross the serosal line of the uterus, and a laparoscopic niche resection was performed if the cesarean scar pregnancy crossed the serosal line. The main outcomes were treatment efficacy and time to subsequent ongoing pregnancy or pregnancy leading to a live birth.
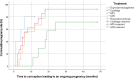
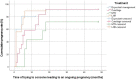
Results: Of the 60 included women, 5 (8.3%) were managed expectantly, 8 (13.3%) were treated with methotrexate, 31 (51.8%) were treated with a curettage, and 16 (26.7%) with a laparoscopic niche resection. The groups were not comparable. The gestational age and human chorionic gonadotropin levels were generally higher in women who received methotrexate or a laparoscopic niche resection. Additional treatment in the conservative group was needed for 4 (80%) women after expectant management and for 7 (87.5%) women after methotrexate treatment. In the surgical group, all 31 women treated with a curettage and all 16 treated with a laparoscopic niche resection did not require additional treatment. The subsequent ongoing pregnancy rate after cesarean scar pregnancy management was 81.1% (30/37) among women who wished to conceive, with a live birth rate of 78.4% (29/37); 1 woman was in her third trimester of pregnancy at the time of analyses. The time between cesarean scar pregnancy management and subsequent ongoing pregnancy was 4 months (interquartile range, 3-6; P=.02) after expectant management, 18 months (interquartile range, 13-22) after initial methotrexate treatment, 5 months (interquartile range, 3-14; P=.01) after a curettage, and 6 months (interquartile range, 4-15; P=.03) after a laparoscopic niche resection.
Conclusion: Surgical treatment of a cesarean scar pregnancy led to a high success rate without additional interventions, high pregnancy rates with a short time interval between treatment, and subsequent pregnancy leading to an ongoing pregnancy or live birth. Conservative management, both with expectant management and methotrexate treatment, led to high (re)intervention rates. Different management approaches are indicated for different types of cesarean scar pregnancies.
Keywords: cesarean delivery; cesarean scar pregnancy; curettage; expectant; fertility; laparoscopic niche resection; medical; methotrexate; reproductive outcomes; surgery.
© 2022 The Authors.
Figures
Similar articles
-
First-trimester cesarean scar pregnancy: a comparative analysis of treatment options from the international registry.Am J Obstet Gynecol. 2024 Jun;230(6):669.e1-669.e19. doi: 10.1016/j.ajog.2023.10.028. Epub 2023 Oct 21. Am J Obstet Gynecol. 2024. PMID: 37865390
-
Effectiveness of laparoscopic niche resection versus expectant management in patients with unexplained infertility and a large uterine caesarean scar defect (uterine niche): protocol for a randomised controlled trial (the LAPRES study).BMJ Open. 2023 Jul 14;13(7):e070950. doi: 10.1136/bmjopen-2022-070950. BMJ Open. 2023. PMID: 37451732 Free PMC article.
-
Cesarean Scar Pregnancy, Incidence, and Recurrence: Five-Year Experience at a Single Tertiary Care Referral Center.Obstet Gynecol. 2018 Nov;132(5):1285-1295. doi: 10.1097/AOG.0000000000002940. Obstet Gynecol. 2018. PMID: 30303911
-
Reproductive outcomes following cesarean scar pregnancy - a case series and review of the literature.Eur J Obstet Gynecol Reprod Biol. 2016 May;200:102-7. doi: 10.1016/j.ejogrb.2016.02.039. Epub 2016 Mar 8. Eur J Obstet Gynecol Reprod Biol. 2016. PMID: 27014853 Review.
-
Cesarean Scar Ectopic Pregnancy: Current Management Strategies.Obstet Gynecol Surv. 2018 May;73(5):293-302. doi: 10.1097/OGX.0000000000000561. Obstet Gynecol Surv. 2018. PMID: 29850919 Review.
Cited by
-
Efficacy, Safety and Outcomes of the Laparoscopic Management of Cesarean Scar Ectopic Pregnancy as a Single Therapeutic Approach: A Case Series.J Clin Med. 2023 Dec 14;12(24):7673. doi: 10.3390/jcm12247673. J Clin Med. 2023. PMID: 38137743 Free PMC article.
References
-
- Ben Nagi J, Helmy S, Ofili-Yebovi D, Yazbek J, Sawyer E, Jurkovic D. Reproductive outcomes of women with a previous history of caesarean scar ectopic pregnancies. Hum Reprod. 2007;22:2012–2015. - PubMed
-
- Boerma T, Ronsmans C. Global epidemiology of use of and disparities in caesarean sections - authors’ reply. Lancet. 2019;394:25. - PubMed
-
- Timor-Tritsch IE, Monteagudo A. Unforeseen consequences of the increasing rate of cesarean deliveries: early placenta accreta and cesarean scar pregnancy. A review. Am J Obstet Gynecol. 2012;207:14–29. - PubMed
-
- Silver RM. Implications of the first cesarean: perinatal and future reproductive health and subsequent cesareans, placentation issues, uterine rupture risk, morbidity, and mortality. Semin Perinatol. 2012;36:315–323. - PubMed
LinkOut - more resources
Full Text Sources

