PARP inhibition utilized in combination therapy with Olaparib-Temozolomide to achieve disease stabilization in a rare case of BRCA1-mutant, metastatic myxopapillary ependymoma
- PMID: 36698626
- PMCID: PMC9869186
- DOI: 10.1177/20363613231152333
PARP inhibition utilized in combination therapy with Olaparib-Temozolomide to achieve disease stabilization in a rare case of BRCA1-mutant, metastatic myxopapillary ependymoma
Abstract
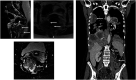
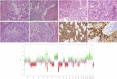
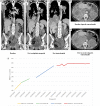
Myxopapillary ependymoma (MPE) is a primary tumor of the central nervous system (CNS), characteristically an indolent malignancy involving the spinal conus medullaris, Filum terminale or cauda equina. We present a rare case of MPE, recurrent in the pelvic soft tissue with eventual pleural and intra-pulmonary metastasis. Refractory to repeated gross resection, adjuvant radiotherapy, platinum-based chemotherapy and temozolomide exploitation of mutant somatic BRCA1 status with the addition of a poly (ADP-ribose); polymerase inhibitor (PARPi) in a novel combination regimen with olaparib-temozolomide (OT) has achieved stable radiological disease after 10 cycles.
Keywords: Oncology; PARP inhibitor; ependymoma.
© The Author(s) 2023.
Conflict of interest statement
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: D.C. reports grants from the NIHR, MedImmune/AstraZeneca, Clovis, Eli Lilly, 4SC, Bayer, Celgene, Roche and Leap Therapeutics, and he is on the scientific advisory board of OVIBIO. I.C. reports grants from Eli Lilly and Janssen-Cilag; he is on the scientific advisory board of Eli Lilly, Bristol Meyers Squibb, MSD, Bayer, Roche, Merck-Serono, Five Prime Therapeutics, Astra-Zeneca, OncXerna, Pierre Fabre, Boehringer Ingelheim, Incyte, Astella, GSK, Sotio, Eisai and Daiichi-Sankyo; and he receives honoraria from Eli Lilly and Servier. The remaining authors report no conflicts of interest. The views expressed are those of the authors and not necessarily those of the UK NIHR or the Department of Health and Social Care.
Figures
Similar articles
-
Primary multifocal myxopapillary ependymoma of the filum terminale.J Neurosurg Sci. 2016 Dec;60(4):424-9. Epub 2015 Jul 8. J Neurosurg Sci. 2016. PMID: 26154385
-
Primary Seeding of Myxopapillary Ependymoma: Different Disease in Adult Population? Case Report and Review of Literature.World Neurosurg. 2017 Mar;99:812.e21-812.e26. doi: 10.1016/j.wneu.2016.12.022. Epub 2016 Dec 29. World Neurosurg. 2017. PMID: 28040529 Review.
-
Concomitant localization of a myxopapillary ependymoma at the middle thoracic part of the spinal cord and at the distal part of the filum terminale. Case report.J Neurosurg Sci. 2008 Sep;52(3):87-91. J Neurosurg Sci. 2008. PMID: 18636054
-
Spinal myxopapillary ependymoma with interval drop metastasis presenting as cauda equina syndrome: case report and review of literature.J Spine Surg. 2016 Sep;2(3):216-221. doi: 10.21037/jss.2016.08.06. J Spine Surg. 2016. PMID: 27757435 Free PMC article.
-
Remarkable efficacy of temozolomide for relapsed spinal myxopapillary ependymoma with multiple recurrence and cerebrospinal dissemination: a case report and literature review.Eur Spine J. 2018 Jul;27(Suppl 3):421-425. doi: 10.1007/s00586-017-5413-z. Epub 2017 Dec 21. Eur Spine J. 2018. PMID: 29270703 Review.
Cited by
-
Extra-neural metastases of recurrent myxopapillary ependymoma: A patient case and literature review.Surg Neurol Int. 2025 May 16;16:182. doi: 10.25259/SNI_190_2025. eCollection 2025. Surg Neurol Int. 2025. PMID: 40469371 Free PMC article.
-
The Role of Radiotherapy, Chemotherapy, and Targeted Therapies in Adult Intramedullary Spinal Cord Tumors.Cancers (Basel). 2024 Aug 6;16(16):2781. doi: 10.3390/cancers16162781. Cancers (Basel). 2024. PMID: 39199553 Free PMC article. Review.
References
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

