Calcitriol-enhanced autophagy in gingival epithelium attenuates periodontal inflammation in rats with type 2 diabetes mellitus
- PMID: 36704029
- PMCID: PMC9872194
- DOI: 10.3389/fendo.2022.1051374
Calcitriol-enhanced autophagy in gingival epithelium attenuates periodontal inflammation in rats with type 2 diabetes mellitus
Abstract
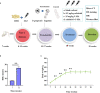
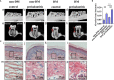
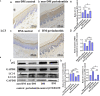
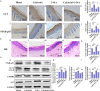
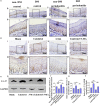
Type 2 diabetes mellitus (T2DM)-associated periodontitis is a common disease with high prevalence, associated with persistent infection and complicated manifestations. Calcitriol (1 alpha, 25-dihydroxyvitamin D3, 1,25D) is the active form of vitamin D that plays a protective role in immune regulation, bone metabolism, and inflammatory response. In this study, we constructed a T2DM model in rats by combining a high-fat diet with low-dose streptozotocin. The periodontitis model in rats was developed by ligation and Porphyromonas gingivalis (ATCC 33277) inoculation. Rats were randomly divided into five groups: non-diabetic blank, diabetic blank, diabetes with calcitriol treatment, diabetes with 3-methyladenine (3-MA) treatment, or diabetes with calcitriol and 3-MA treatment. The diabetic rats exhibited an intense inflammatory response and decreased autophagy compared with the non-diabetic rats. Intraperitoneal injection of calcitriol and autophagy inhibitor (3-MA) allowed us to explore the effect of calcitriol on inflammation in the gingival epithelium and the role of autophagy in this process. Treatment with calcitriol resulted in the decreased expression of NFκB-p65, p62/SQSTM1 and inflammatory response and increased expression of LC3-II/LC3-I. Application of 3-MA significantly suppressed autophagy, which was apparently retrieved by calcitriol. Antibacterial peptide (LL-37) is the only antimicrobial peptide in the cathelicidin family that is found in the human body, and it exhibits a broad spectrum of antibacterial activity and regulates the immune system. In the present study, our findings indicated that calcitriol-enhanced autophagy may attenuated periodontitis and the decrease of LL-37 was rescued by calcitriol treatment in the gingival epithelial cells of T2DM rats. Our study provides evidence for the application of calcitriol as an adjunctive treatment for T2DM-associated periodontitis.
Keywords: LL-37; Porphyromonas gingivalis; autophagy; calcitriol; rats model; type 2 diabetes mellitus.
Copyright © 2023 Wang, Huang, Xu, Li, Ma and Tang.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures


Similar articles
-
25-Hydroxyvitamin D3 -enhanced PTPN2 positively regulates periodontal inflammation through the JAK/STAT pathway in human oral keratinocytes and a mouse model of type 2 diabetes mellitus.J Periodontal Res. 2018 Jun;53(3):467-477. doi: 10.1111/jre.12535. Epub 2018 Mar 8. J Periodontal Res. 2018. PMID: 29516520
-
25-Hydroxyvitamin D3 Alleviates Experimental Periodontitis via Promoting Expression of Cathelicidin in Mice with Type 2 Diabetic Mellitus.J Nutr Sci Vitaminol (Tokyo). 2018;64(5):307-315. doi: 10.3177/jnsv.64.307. J Nutr Sci Vitaminol (Tokyo). 2018. PMID: 30381619
-
Calcitriol decreases live Porphyromonas gingivalis internalized into epithelial cells and monocytes by promoting autophagy.J Periodontol. 2020 Jul;91(7):956-966. doi: 10.1002/JPER.19-0510. Epub 2019 Dec 15. J Periodontol. 2020. PMID: 31774177
-
Autophagy as a potential mechanism underlying the biological effect of 1,25-Dihydroxyvitamin D3 on periodontitis: a narrative review.BMC Oral Health. 2023 Feb 13;23(1):90. doi: 10.1186/s12903-023-02802-9. BMC Oral Health. 2023. PMID: 36782172 Free PMC article. Review.
-
Pathogenic Mechanisms That May Link Periodontal Disease and Type 2 Diabetes Mellitus-The Role of Oxidative Stress.Int J Mol Sci. 2024 Sep 11;25(18):9806. doi: 10.3390/ijms25189806. Int J Mol Sci. 2024. PMID: 39337292 Free PMC article. Review.
Cited by
-
Epigenetic Regulation of Autophagy in Bone Metabolism.Function (Oxf). 2024 Jan 27;5(2):zqae004. doi: 10.1093/function/zqae004. eCollection 2024. Function (Oxf). 2024. PMID: 38486976 Free PMC article. Review.
-
The Role of Vitamin C and Vitamin D in the Pathogenesis and Therapy of Periodontitis-Narrative Review.Int J Mol Sci. 2023 Apr 5;24(7):6774. doi: 10.3390/ijms24076774. Int J Mol Sci. 2023. PMID: 37047746 Free PMC article. Review.
-
The role of autophagy in odontogenesis, dental implant surgery, periapical and periodontal diseases.J Cell Mol Med. 2024 Apr;28(8):e18297. doi: 10.1111/jcmm.18297. J Cell Mol Med. 2024. PMID: 38613351 Free PMC article. Review.
-
The inhibitory effects of 7ND protein on osteoclast differentiation in apical periodontitis.Front Cell Infect Microbiol. 2025 Jun 27;15:1597604. doi: 10.3389/fcimb.2025.1597604. eCollection 2025. Front Cell Infect Microbiol. 2025. PMID: 40654573 Free PMC article.
-
Periodontopathogen-Related Cell Autophagy-A Double-Edged Sword.Inflammation. 2025 Feb;48(1):1-14. doi: 10.1007/s10753-024-02049-8. Epub 2024 May 19. Inflammation. 2025. PMID: 38762837 Review.
References
-
- James SL, Abate D, Abate KH, Abay SM, Abbafati C, Abbasi N, et al. . Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990-2017: a systematic analysis for the global burden of disease study 2017. Lancet (2018) 392(10159):1789–858. doi: 10.1016/S0140-6736(18)32279-7 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases

