Molecular Characteristics of Early-Onset Colorectal Cancer According to Detailed Anatomical Locations: Comparison With Later-Onset Cases
- PMID: 36707929
- PMCID: PMC10065351
- DOI: 10.14309/ajg.0000000000002171
Molecular Characteristics of Early-Onset Colorectal Cancer According to Detailed Anatomical Locations: Comparison With Later-Onset Cases
Abstract
Introduction: Early-onset colorectal cancer diagnosed before the age of 50 years has been increasing. Likely reflecting the pathogenic role of the intestinal microbiome, which gradually changes across the entire colorectal length, the prevalence of certain tumor molecular characteristics gradually changes along colorectal subsites. Understanding how colorectal tumor molecular features differ by age and tumor location is important in personalized patient management.
Methods: Using 14,004 cases with colorectal cancer including 3,089 early-onset cases, we examined microsatellite instability (MSI), CpG island methylator phenotype (CIMP), and KRAS and BRAF mutations in carcinomas of the cecum, ascending colon, transverse colon, descending colon, sigmoid colon, and rectum and compared early-onset cases with later-onset cases.
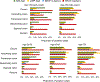
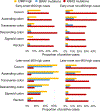
Results: The proportions of MSI-high, CIMP-high, and BRAF -mutated early-onset tumors were lowest in the rectum (8.8%, 3.4%, and 3.5%, respectively) and highest in the ascending colon (46% MSI-high; 15% CIMP-high) or transverse colon (8.6% BRAF -mutated) (all Ptrend <0.001 across the rectum to ascending colon). Compared with later-onset tumors, early-onset tumors showed a higher prevalence of MSI-high status and a lower prevalence of CIMP-high status and BRAF mutations in most subsites. KRAS mutation prevalence was higher in the cecum compared with that in the other subsites in both early-onset and later-onset tumors ( P < 0.001). Notably, later-onset MSI-high tumors showed a continuous decrease in KRAS mutation prevalence from the rectum (36%) to ascending colon (9%; Ptrend <0.001), followed by an increase in the cecum (14%), while early-onset MSI-high cancers showed no such trend.
Discussion: Our findings support biogeographical and pathogenic heterogeneity of colorectal carcinomas in different colorectal subsites and age groups.
Copyright © 2023 by The American College of Gastroenterology.
Conflict of interest statement
A.T.C. previously served as a consultant for Bayer Healthcare and Pfizer Inc. M.G. receives research funding from Bristol-Myers Squibb and Merck. A.T.C. is a Stuart and Suzanne Steele MGH Research Scholar. The other authors declare no potential conflicts of interest. The content is solely the responsibility of the authors and does not necessarily represent the official views of U.S. NIH. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Figures
References
Publication types
MeSH terms
Substances
Grants and funding
- P01 CA087969/CA/NCI NIH HHS/United States
- R01 CA137178/CA/NCI NIH HHS/United States
- U01 CA167551/CA/NCI NIH HHS/United States
- UM1 CA186107/CA/NCI NIH HHS/United States
- UM1 CA167552/CA/NCI NIH HHS/United States
- R00 CA215314/CA/NCI NIH HHS/United States
- 001/WHO_/World Health Organization/International
- R01 CA076366/CA/NCI NIH HHS/United States
- R35 CA197735/CA/NCI NIH HHS/United States
- R01 CA248857/CA/NCI NIH HHS/United States
- P30 CA015704/CA/NCI NIH HHS/United States
- P30 DK043351/DK/NIDDK NIH HHS/United States
- P01 CA055075/CA/NCI NIH HHS/United States
- S10 OD028685/OD/NIH HHS/United States
- R01 CA151993/CA/NCI NIH HHS/United States
- U01 CA167552/CA/NCI NIH HHS/United States
- R01 CA048998/CA/NCI NIH HHS/United States
- U01 CA137088/CA/NCI NIH HHS/United States
- U01 CA084968/CA/NCI NIH HHS/United States
- U01 CA074783/CA/NCI NIH HHS/United States
- R35 CA253185/CA/NCI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

