Iron Metabolism in Cardiovascular Disease: Physiology, Mechanisms, and Therapeutic Targets
- PMID: 36730380
- PMCID: PMC9907000
- DOI: 10.1161/CIRCRESAHA.122.321667
Iron Metabolism in Cardiovascular Disease: Physiology, Mechanisms, and Therapeutic Targets
Abstract
The cardiovascular system requires iron to maintain its high energy demands and metabolic activity. Iron plays a critical role in oxygen transport and storage, mitochondrial function, and enzyme activity. However, excess iron is also cardiotoxic due to its ability to catalyze the formation of reactive oxygen species and promote oxidative damage. While mammalian cells have several redundant iron import mechanisms, they are equipped with a single iron-exporting protein, which makes the cardiovascular system particularly sensitive to iron overload. As a result, iron levels are tightly regulated at many levels to maintain homeostasis. Iron dysregulation ranges from iron deficiency to iron overload and is seen in many types of cardiovascular disease, including heart failure, myocardial infarction, anthracycline-induced cardiotoxicity, and Friedreich's ataxia. Recently, the use of intravenous iron therapy has been advocated in patients with heart failure and certain criteria for iron deficiency. Here, we provide an overview of systemic and cellular iron homeostasis in the context of cardiovascular physiology, iron deficiency, and iron overload in cardiovascular disease, current therapeutic strategies, and future perspectives.
Keywords: biology; catalysis; electrons; heart; iron; macrophages; metabolism.
Figures


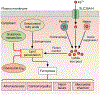
References
-
- Frey PA and Reed GH. The ubiquity of iron. ACS Chem Biol. 2012;7:1477–81. - PubMed
-
- Andrews NC. Disorders of iron metabolism. N Engl J Med. 1999;341:1986–95. - PubMed
-
- Hentze MW, Muckenthaler MU and Andrews NC. Balancing acts: molecular control of mammalian iron metabolism. Cell. 2004;117:285–97. - PubMed
-
- Gudjoncik A, Guenancia C, Zeller M, Cottin Y, Vergely C and Rochette L. Iron, oxidative stress, and redox signaling in the cardiovascular system. Mol Nutr Food Res. 2014;58:1721–38. - PubMed
-
- Jomova K and Valko M. Advances in metal-induced oxidative stress and human disease. Toxicology. 2011;283:65–87. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

