Methylprednisolone versus intravenous immunoglobulins in children with paediatric inflammatory multisystem syndrome temporally associated with SARS-CoV-2 (PIMS-TS): an open-label, multicentre, randomised trial
- PMID: 36746174
- PMCID: PMC9897729
- DOI: 10.1016/S2352-4642(23)00020-2
Methylprednisolone versus intravenous immunoglobulins in children with paediatric inflammatory multisystem syndrome temporally associated with SARS-CoV-2 (PIMS-TS): an open-label, multicentre, randomised trial
Erratum in
-
Correction to Lancet Child Adolesc Health 2023; 7: 238-48.Lancet Child Adolesc Health. 2023 Apr;7(4):e10. doi: 10.1016/S2352-4642(23)00060-3. Lancet Child Adolesc Health. 2023. PMID: 36948662 Free PMC article. No abstract available.
Abstract
Background: The emergence of paediatric inflammatory multisystem syndrome temporally associated with SARS-CoV-2 (PIMS-TS) led to the widespread use of anti-inflammatory treatments in the absence of evidence from randomised controlled trials (RCTs). We aimed to assess the effectiveness of intravenous methylprednisolone compared with intravenous immunoglobulins.
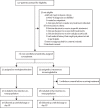
Methods: This is an open-label, multicentre, two-arm RCT done at ten hospitals in Switzerland in children younger than 18 years hospitalised with PIMS-TS (defined as age <18 years; fever and biochemical evidence of inflammation, and single or multiorgan dysfunction; microbiologically proven or putative contact with SARS-CoV-2; and exclusion of any other probable disease). Patients were randomly assigned 1:1 to intravenous methylprednisolone (10 mg/kg per day for 3 days) or intravenous immunoglobulins (2 g/kg as a single dose). The primary outcome was length of hospital stay censored at day 28, death, or discharge. Secondary outcomes included proportion and duration of organ support. Analyses were done by intention-to-treat. The study was registered with Swiss National Clinical Trials Portal (SNCTP000004720) and ClinicalTrials.gov (NCT04826588).
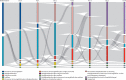
Findings: Between May 21, 2021, and April 15, 2022, 75 patients with a median age of 9·1 years (IQR 6·2-12·2) were included in the intention-to-treat population (37 in the methylprednisolone group and 38 in the intravenous immunoglobulins group). The median length of hospital stay was 6·0 days (IQR 4·0-8·0) in the methylprednisolone group and 6·0 days (IQR 5·0-8·8) in the intravenous immunoglobulins group (estimated effect size -0·037 of the log10 transformed times, 95% CI -0·13 to 0·065, p=0·42). Fewer patients in the methylprednisolone group (ten [27%] of 37) required respiratory support compared with the intravenous immunoglobulin group (21 [55%] of 38, p=0·025). Need and duration of inotropes, admission to intensive care units, cardiac events after baseline, and major bleeding and thrombotic events were not significantly different between the study groups.
Interpretation: In this RCT, treatment with methylprednisolone in children with PIMS-TS did not significantly affect the length of hospital stay compared with intravenous immunoglobulins. Intravenous methylprednisolone could be an acceptable first-line treatment in children with PIMS-TS.
Funding: NOMIS Foundation, Vontobel Foundation, and Gaydoul Foundation.
Copyright © 2023 Elsevier Ltd. All rights reserved.
Conflict of interest statement
Declaration of interests LJS was supported by grants from the NOMIS Foundation, the Vontobel Foundation, and the Gaydoul Foundation for this study. Swiss PedNet (https://www.swisspednet.ch/) provided infrastructure support for study coordination and monitoring. AA was supported by the Swiss National Science Foundation grant CRSK-3_190977/1 during the study period. JAB received grant support paid to the institution from the European and Developing Countries Clinical Trials Partnership (PediCaP, RIA2017MC-2023), Horizon 2020 (NeoIPC, grant 965328), the Swiss National Science Foundation (KIDS-STEP, grant 173532), National Institute for Health Research (CAP-IT, project 13/88/11), Wellcome Trust (ADILA, award 13573-10), the Swiss Personalised Health Network (Secretariat for Education Research and Innovation) (SwissPedHealth, award NDS-2021-911), in the past 36 months; consulting fees paid to the institution from Shionogi, Sandoz, Basilea, and GSK; payments to the institution for presentations, lectures, speakers bureaus, manuscript writing or educational events in the past 36 months from Pfizer, Sandoz, and Bayer; participated at independent data monitoring committee boards of Boost-EBOC (Chair, unfunded), Avenir trial (member, expenses), Lakana trial (member, unfunded), in the past 36 months; is the vice president of the SwissPedNet (unpaid) and leadership of Severe Bacterial Infection and Antimicrobial Resistance working group of the Penta Foundation (unpaid). TW gave presentations for Novartis (payment to the institution) in the past 36 months. MB received an unrestricted Grant in the past 36 months from DOMARENA Foundation and Consulting fees by MSD; receives payment for Post Graduate Education in Paediatric Infectious Diseases; received support for the European Society For Paediatric Infectious Diseases (ESPID) Annual Meeting as Chair of Educational Committee; is Chair of the ESPID Education Committee and board members of SwissPedNet. All other authors declare no competing interests.
Figures

Comment in
-
Methylprednisolone or Intravenous Immunoglobulin in Children with Paediatric Inflammatory Multisystem Syndrome Temporally Associated With SARS-CoV-2 (PIMS-TS)?: Evidence-based Medicine Viewpoint.Indian Pediatr. 2023 Jul 15;60(7):571-574. Indian Pediatr. 2023. PMID: 37424121 No abstract available.
-
Methylprednisolone or Intravenous Immunoglobulin in Children with Paediatric Inflammatory Multisystem Syndrome Temporally Associated With SARS-CoV-2 (PIMS-TS)?: Pediatric Rheumatologist's Viewpoint.Indian Pediatr. 2023 Jul 15;60(7):574-575. Indian Pediatr. 2023. PMID: 37424122 No abstract available.
-
Methylprednisolone or Intravenous Immunoglobulin in Children with Paediatric Inflammatory Multisystem Syndrome Temporally Associated With SARS-CoV-2 (PIMS-TS)?: Pediatrician's Viewpoint.Indian Pediatr. 2023 Jul 15;60(7):575. Indian Pediatr. 2023. PMID: 37424123 No abstract available.
References
Publication types
MeSH terms
Substances
Supplementary concepts
Associated data
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

