Child Opportunity Index and Hospital Utilization in Children With Traumatic Brain Injury Admitted to the PICU
- PMID: 36751518
- PMCID: PMC9894353
- DOI: 10.1097/CCE.0000000000000840
Child Opportunity Index and Hospital Utilization in Children With Traumatic Brain Injury Admitted to the PICU
Abstract
The need to understand how Community-based disparities impact morbidity and mortality in pediatric critical illness, such as traumatic brain injury. Test the hypothesis that ZIP code-based disparities in hospital utilization, including length of stay (LOS) and hospital costs, exist in a cohort of children with traumatic brain injury (TBI) admitted to a PICU using the Child Opportunity Index (COI).
Design: Multicenter retrospective cohort study.
Setting: Pediatric Health Information System (PHIS) database.
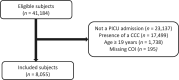
Patients: Children 0-18 years old admitted to a PHIS hospital with a diagnosis of TBI from January 2016 to December 2020 requiring PICU care. To identify the most severely injured children, a study-specific definition of "Complicated TBI" was created based on radiology, pharmacy, and procedure codes.
Interventions: None.
Main outcomes and measures: Using nationally normed ZIP code-level COI data, patients were categorized into COI quintiles. A low COI ZIP code has low childhood opportunity based on weighted indicators within educational, health and environmental, and social and economic domains. Population-averaged generalized estimating equation (GEE) models, adjusted for patient and clinical characteristics examined the association between COI and study outcomes, including hospital LOS and accrued hospital costs. The median age of this cohort of 8,055 children was 58 months (interquartile range [IQR], 8-145 mo). There were differences in patient demographics and rates of Complicated TBI between COI levels. The median hospital LOS was 3.0 days (IQR, 2.0-6.0 d) and in population-averaged GEE models, children living in very low COI ZIP codes were expected to have a hospital LOS 10.2% (95% CI, 4.1-16.8%; p = 0.0142) longer than children living in very high COI ZIP codes. For the 11% of children with a Complicated TBI, the relationship between COI and LOS was lost in multivariable models. COI level was not predictive of accrued hospital costs in this study.
Conclusions: Children with TBI requiring PICU care living in low-opportunity ZIP codes have higher injury severity and longer hospital LOS compared with children living in higher-opportunity ZIP codes. Additional studies are needed to understand why these differences exist.
Keywords: ZIP code; pediatric critical care medicine; social determinants of health; traumatic brain injury.
Copyright © 2023 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of the Society of Critical Care Medicine.
Conflict of interest statement
The authors have disclosed that they do not have any potential conflicts of interest.
Figures
Similar articles
-
Child Opportunity Index and Pediatric Intensive Care Outcomes: A Multicenter Retrospective Study in the United States.Pediatr Crit Care Med. 2024 Apr 1;25(4):323-334. doi: 10.1097/PCC.0000000000003427. Epub 2023 Dec 13. Pediatr Crit Care Med. 2024. PMID: 38088770 Free PMC article.
-
Association Between Social Determinants of Health and Severity of Traumatic Brain Injury in Children: A Retrospective Cohort Study.Am Surg. 2025 May 17:31348251341951. doi: 10.1177/00031348251341951. Online ahead of print. Am Surg. 2025. PMID: 40380933
-
Area-Level Socioeconomic Disadvantage and Post-PICU Outcomes in Children With an Acquired Brain Injury: Single-Center Retrospective Cohort, 2016-2023.Pediatr Crit Care Med. 2025 May 1;26(5):e633-e646. doi: 10.1097/PCC.0000000000003720. Epub 2025 Mar 6. Pediatr Crit Care Med. 2025. PMID: 40047490
-
Child Opportunity Index 2.0 and acute care utilization among children with medical complexity.J Hosp Med. 2022 Apr;17(4):243-251. doi: 10.1002/jhm.12810. Epub 2022 Mar 16. J Hosp Med. 2022. PMID: 35535923 Free PMC article.
-
Association of the Child Opportunity Index and Inpatient Illness Severity in the United States, 2018-2019.Acad Pediatr. 2024 Sep-Oct;24(7):1101-1109. doi: 10.1016/j.acap.2023.12.008. Epub 2023 Dec 28. Acad Pediatr. 2024. PMID: 38159600
Cited by
-
Community and Patient Features and Health Care Point of Entry for Pediatric Concussion.JAMA Netw Open. 2024 Oct 1;7(10):e2442332. doi: 10.1001/jamanetworkopen.2024.42332. JAMA Netw Open. 2024. PMID: 39476230 Free PMC article.
-
Association between social determinants of health and pediatric traumatic brain injury outcomes.Front Neurol. 2024 Mar 14;15:1339255. doi: 10.3389/fneur.2024.1339255. eCollection 2024. Front Neurol. 2024. PMID: 38550344 Free PMC article.
-
Explanatory capacity of measures of community context for paediatric injury hospitalisations in the USA.Inj Prev. 2025 Jun 26:ip-2024-045423. doi: 10.1136/ip-2024-045423. Online ahead of print. Inj Prev. 2025. PMID: 39819764 Free PMC article.
-
Utility of Aprepitant in the Management of Pediatric Patients with Cyclical Vomiting Syndrome.Medicines (Basel). 2024 Dec 11;11(8):21. doi: 10.3390/medicines11080021. Medicines (Basel). 2024. PMID: 39728392 Free PMC article.
-
Health Disparities in the Management and Outcomes of Critically Ill Children and Neonates: A Scoping Review.Crit Care Clin. 2024 Oct;40(4):641-657. doi: 10.1016/j.ccc.2024.05.002. Epub 2024 Jun 22. Crit Care Clin. 2024. PMID: 39218478
References
-
- Sheehan BM, Grigorian A, Gambhir S, et al. : Early tracheostomy for severe pediatric traumatic brain injury is associated with reduced intensive care unit length of stay and total ventilator days. J Intensive Care Med 2020; 35:1346–1351 - PubMed
-
- Howard I, Joseph JG, Natale JE: Pediatric traumatic brain injury: Do racial/ethnic disparities exist in brain injury severity, mortality, or medical disposition? Ethn Dis 2005; 15(4 Suppl 5):S5–S51–S56 - PubMed
-
- Fieldston ES, Zaniletti I, Hall M, et al. : Community household income and resource utilization for common inpatient pediatric conditions. Pediatrics 2013; 132:e1592–e1601 - PubMed
LinkOut - more resources
Full Text Sources