Impact of Pandemic Response on Training Experience of Anesthesiology Residents in an Academic Medical Center: A Retrospective Cohort Study
- PMID: 36756025
- PMCID: PMC9903179
- DOI: 10.7759/cureus.33500
Impact of Pandemic Response on Training Experience of Anesthesiology Residents in an Academic Medical Center: A Retrospective Cohort Study
Abstract
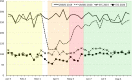
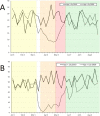
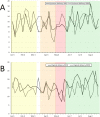
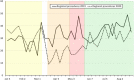
Background The impact of the coronavirus disease 2019 (COVID-19) pandemic substantially altered operations at hospitals that support graduate medical education. We examined the impact of the pandemic on an anesthesiology training program with respect to overall case volume, subspecialty exposure, procedural skill experience, and approaches to airway management. Methods Data for this single center, retrospective cohort study came from an Institutional Review Board approved repository for clinical data. Date ranges were divided into the following phases in 2020: Pre-Pandemic (PP), Early Pandemic (EP), Recovery 1 (R1), and Recovery 2 (R2). All periods were compared to the same period from 2019 for case volume, anesthesia provider type, trainee exposure to Accreditation Council for Graduate Medical Education (ACGME) index case categories, airway technique, and patient variables. Results 15,087 cases were identified, with 5,598 (37.6%) in the PP phase, 1,570 (10.5%) in the EP phase, 1,451 (9.7%) in the R1 phase, and 6,269 (42.1%) in the R2 phase. There was a significant reduction in case volume during the EP phase compared to the corresponding period in 2019 (-55.3%; P < .001) that improved but did not return to baseline by the R2 phase (-17.6%; P < .001). ACGME required minimum cases were reduced during the EP phase compared to 2019 data for pediatric cases (age < 12 y, -72.1%; P < .001 and age < 3 y, -53.5%; P < .006) and cardiopulmonary bypass cases (52.3%, P < .003). Surgical subspecialty case volumes were significantly reduced in the EP phase except for transplant surgery. By the R2 phase, all subspecialty volumes had recovered except for plastic surgery (14.9 vs. 10.5 cases/week; P < .006) and surgical endoscopy (59.2 vs. 40 cases/week; P < .001). Use of video laryngoscopy (VL) and rapid sequence induction and intubation (RSII) also increased from the PP to the EP phase (24.6 vs. 79.6%; P < .001 and 10.3 vs. 52.3%; P < .001, respectively) and remained elevated into the R2 phase (35.2%; P < 0.001 and 23.1%; P < .001, respectively). Conclusions The COVID-19 pandemic produced significant changes in surgical case exposure for a relatively short period. The impact was short-lived, with sufficient remaining time to meet the annual ACGME program minimum case requirements and procedural experiences. The longer-term impact may be a shift towards the increased use of VL and RSII, which became more prevalent during the early phase of the pandemic.
Keywords: academic anesthesiology; accreditation council for graduate medical education (acgme); anesthesia residency; covid 19; procedure training.
Copyright © 2023, Grissom et al.
Conflict of interest statement
The authors have declared financial relationships, which are detailed in the next section.
Figures


References
LinkOut - more resources
Full Text Sources
Miscellaneous
