Osteoimmune regulation underlies oral implant osseointegration and its perturbation
- PMID: 36761175
- PMCID: PMC9902598
- DOI: 10.3389/fimmu.2022.1056914
Osteoimmune regulation underlies oral implant osseointegration and its perturbation
Abstract
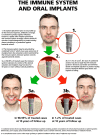
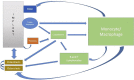
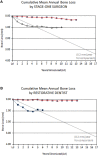
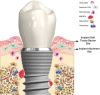
In the field of biomaterials, an endosseous implant is now recognized as an osteoimmunomodulatory but not bioinert biomaterial. Scientific advances in bone cell biology and in immunology have revealed a close relationship between the bone and immune systems resulting in a field of science called osteoimmunology. These discoveries have allowed for a novel interpretation of osseointegration as representing an osteoimmune reaction rather than a classic bone healing response, in which the activation state of macrophages ((M1-M2 polarization) appears to play a critical role. Through this viewpoint, the immune system is responsible for isolating the implant biomaterial foreign body by forming bone around the oral implant effectively shielding off the implant from the host bone system, i.e. osseointegration becomes a continuous and dynamic host defense reaction. At the same time, this has led to the proposal of a new model of osseointegration, the foreign body equilibrium (FBE). In addition, as an oral wound, the soft tissues are involved with all their innate immune characteristics. When implant integration is viewed as an osteoimmune reaction, this has implications for how marginal bone is regulated. For example, while bacteria are constitutive components of the soft tissue sulcus, if the inflammatory front and immune reaction is at some distance from the marginal bone, an equilibrium is established. If however, this inflammation approaches the marginal bone, an immune osteoclastic reaction occurs and marginal bone is removed. A number of clinical scenarios can be envisioned whereby the osteoimmune equilibrium is disturbed and marginal bone loss occurs, such as complications of aseptic nature and the synergistic activation of pro-inflammatory pathways (implant/wear debris, DAMPs, and PAMPs). Understanding that an implant is a foreign body and that the host reacts osteoimmunologically to shield off the implant allows for a distinction to be drawn between osteoimmunological conditions and peri-implant bone loss. This review will examine dental implant placement as an osteoimmune reaction and its implications for marginal bone loss.
Keywords: bone healing; bone regeneration; immune reaction; osteoimmunology; osteomechanobiology; osteometabolics; osteoneurology; revascularization.
Copyright © 2023 Albrektsson, Tengvall, Amengual, Coli, Kotsakis and Cochran.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

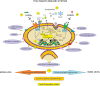
References
-
- Wennerberg A, Albrektsson T, Chrcanovic B. Long-term clinical outcome of implants with different surface modifications. Eur J Oral Implantol (2018) 11 Suppl 1:S123–S36. - PubMed
-
- Trindade R, Albrektsson T, Galli S, Prgomet Z, Tengvall P, Wennerberg A. Osseointegration and foreign body reaction: Titanium implants activate the immune system and suppress bone resorption during the first 4 weeks after implantation. Clin Implant Dent Relat Res (2018) 20(1):82–91. doi: 10.1111/cid.12578 - DOI - PubMed
-
- Albrektsson T, Chrcanovic B, Jacobsson M, Wennerberg A. Osseointegration of implants – A biological and clinical overview. JSM Dental Surg (2017) 2(3):1022–7.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

