Relationship of Glucose, C-peptide, Leptin, and BDNF in Maternal and Umbilical Vein Blood in Type-1 Diabetes
- PMID: 36771307
- PMCID: PMC9919383
- DOI: 10.3390/nu15030600
Relationship of Glucose, C-peptide, Leptin, and BDNF in Maternal and Umbilical Vein Blood in Type-1 Diabetes
Abstract
The study aimed to determine the relationship between glucose, C-peptide, brain-derived neurotrophic factor (BDNF), and leptin between mother and fetus and neonatal weight.
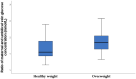
Methods: In the prospective observational cohort study, we included 66 women with type-1 diabetes mellitus (T1DM). According to the z-score for neonatal weight, patients were divided into healthy-weight neonates (n = 42) and overweight neonates (n = 24). The maternal blood samples were taken during pregnancy and cesarean section when the umbilical vein blood sample was also withdrawn. The maternal vein sera were analyzed for fasting glucose, C-reactive protein (CRP), leptin, BDNF, TSH, FT3, and FT4. The umbilical vein sera were analyzed for glucose, C-peptide, leptin, TSH, thyroid-stimulating protein (FT3), free thyroxine (FT4), and BDNF concentration. The neonatologist measured the skinfold thickness on the third day of neonatal life.
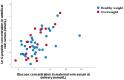
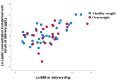
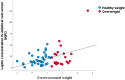
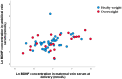
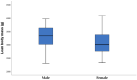
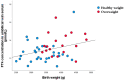
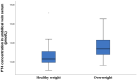
Results: A strong correlation was confirmed between maternal and umbilical vein glucose concentration and maternal glucose and C-peptide in umbilical vein blood. A negative correlation was found between the concentration of BDNF in the umbilical vein and glucose in maternal blood. A strong correlation was seen between BMI and maternal blood leptin concentration, neonatal fat body mass, and umbilical vein blood leptin concentration. Higher BMI elevated BDNF, and TSH increase the odds for overweight neonates in the first trimester of pregnancy. Maternal higher leptin concentration in the first trimester decrease the odds of overweight neonates.
Conclusions: Maternal glucose concentrations affect the fetus's glucose, C-peptide, and BDNF concentrations. Leptin levels increase in maternal blood due to increased body mass index, and in the neonate, fat body mass is responsible for increased leptin concentrations.
Keywords: BDNF; C-peptide; CRP; leptin; pregnancy; skinfold thickness; thyroid hormones; type-1 diabetes mellitus.
Conflict of interest statement
The authors declare no conflict of interest.
Figures


References
-
- Holt R.I.G., DeVries J.H., Hess-Fischl A., Hirsch I.B., Kirkman M.S., Klupa T., Ludwig B., Nørgaard K., Pettus J., Renard E., et al. The Management of Type 1 Diabetes in Adults. A Consensus Report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD) Diabetes Care. 2021;44:2589–2625. doi: 10.2337/dci21-0043. - DOI - PubMed
-
- Kruit H., Mertsalmi S., Rahkonen L. Planned vaginal and planned cesarean delivery outcomes in pregnancies complicated with pregestational type 1 diabetes - A three-year academic tertiary hospital cohort study. BMC Pregnancy Childbirth. 2022;22:173. doi: 10.1186/s12884-022-04510-8. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

