Effects of β-blockers on all-cause mortality in patients with diabetes and coronary heart disease: A systematic review and meta-analysis
- PMID: 36776555
- PMCID: PMC9911879
- DOI: 10.3389/fcell.2023.1076107
Effects of β-blockers on all-cause mortality in patients with diabetes and coronary heart disease: A systematic review and meta-analysis
Abstract
Beta-blockers have been considered as an effective treatment in secondary prevention of coronary heart disease (CHD). However, there is still disputed whether β-blockers can increase all-cause mortality in patients with coronary heart disease and diabetes mellitus (DM). Here, our systematic review and meta-analysis is aiming to assess the effects of β-blockers on all-cause mortality in patients with coronary heart disease and diabetes mellitus. Four databases (PubMed, Embase, Cochrane Library and Web of Science) and other sources were searched to collect randomized controlled trials (RCTs) and cohort studies related to the treatment of β-blockers for coronary heart disease and diabetes mellitus patients. We further evaluated quality of evidence using the grading of recommendations assessment, development, and evaluation (GRADE) approach. Finally, a total of 16,188 records were identified, and four randomized controlled trials and six cohort studies (206,490 patients) were included. Random effects analysis revealed that β-blockers combined with routine treatment (RT) significantly decreased all-cause mortality in patients with coronary heart disease and diabetes mellitus compared with RT in control group (RR 0.59, 95% CI 0.47 to 0.75; p < 0.000 01; I2 = 72%). Subgroup analysis of all-cause mortality by the subtype of diabetes mellitus and definite MI patients (RR 0.54, 95% CI 0.45 to 0.65, p < 0.000 01, I2 = 29%) and the subtype of randomized controlled trials (RR 0.49, 95% CI 0.32 to 0.76, p = 0.001, I2 = 0%) indicated a relatively small heterogeneity and stable results. β-blockers application significantly reduced cardiovascular death as well (RR 0.56, 95% CI 0.42 to 0.74; p < 0.000 1; I2 = 0%). Our meta-analysis provided critical evidence of β-blockers treatment for patients with coronary heart disease (especially MI type) and diabetes mellitus, and discussed the advantages and potential metabolic risks for the clinical use of β-blockers. This study suggested that β-blockers application may improve all-cause mortality and cardiovascular death in coronary heart disease (especially MI type) and diabetes mellitus patients. However, given a small number of included studies, the aforementioned conclusion should be confirmed in a multi-center, large-scale, and strictly designed trial.
Keywords: all-cause mortality; beta-blockers; coronary heart disease; diabetes mellitus; systematic review.
Copyright © 2023 Chen, Tian, Estau and Li.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
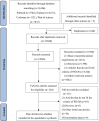





References
-
- Arnold S. V., Bhatt D. L., Barsness G. W., Beatty A. L., Deedwania P. C., Inzucchi S. E., et al. (2020). Clinical management of stable coronary artery disease in patients with type 2 diabetes mellitus: A scientific statement from the American heart association. Circulation 141 (19), e779–e806. 10.1161/CIR.0000000000000766 - DOI - PubMed
-
- Bangalore S., Bhatt D. L., Steg P. G., Weber M. A., Boden W. E., Hamm C. W., et al. (2014). β-Blockers and cardiovascular events in patients with and without myocardial infarction: Post hoc analysis from the CHARISMA trial. Circ. Cardiovasc Qual. Outcomes 7 (6), 872–881. 10.1161/CIRCOUTCOMES.114.001073 - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources

