Trends and In-Hospital Mortality for Perioperative Myocardial Infarction After the Introduction of a Diagnostic Code for Type 2 Myocardial Infarction in the United States Between 2016 and 2018
- PMID: 36795598
- PMCID: PMC10427730
- DOI: 10.1213/ANE.0000000000006404
Trends and In-Hospital Mortality for Perioperative Myocardial Infarction After the Introduction of a Diagnostic Code for Type 2 Myocardial Infarction in the United States Between 2016 and 2018
Abstract
Background: The frequency of perioperative myocardial infarction has been declining; however, previous studies have only described type 1 myocardial infarctions. Here, we evaluate the overall frequency of myocardial infarction with the addition of an International Classification of Diseases 10th revision (ICD-10-CM) code for type 2 myocardial infarction and the independent association with in-hospital mortality.
Methods: A longitudinal cohort study spanning the introduction of the ICD-10-CM diagnostic code for type 2 myocardial infarction using the National Inpatient Sample (NIS) from 2016 to 2018. Hospital discharges that included a primary surgical procedure code for intrathoracic, intraabdominal, or suprainguinal vascular surgery were included. Type 1 and type 2 myocardial infarctions were identified using ICD-10-CM codes. We used segmented logistic regression to estimate change in frequency of myocardial infarctions and multivariable logistic regression to determine the association with in-hospital mortality.
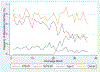
Results: A total of 360,264 unweighted discharges were included, representing 1,801,239 weighted discharges, with median age 59 and 56% female. The overall incidence of myocardial infarction was 0.76% (13,605/1,801,239). Before the introduction of type 2 myocardial infarction code, there was a small baseline decrease in the monthly frequency of perioperative myocardial infarctions (odds ratio [OR], 0.992; 95% confidence interval [CI], 0.984-1.000; P = .042), but no change in the trend after the introduction of the diagnostic code (OR, 0.998; 95% CI, 0.991-1.005; P = .50). In 2018, where there was an entire year where type 2 myocardial infarction was officially a diagnosis, the distribution of myocardial infarction type 1 was 8.8% (405/4580) ST elevation myocardial infarction (STEMI), 45.6% (2090/4580) non-ST elevation myocardial infarction (NSTEMI), and 45.5% (2085/4580) type 2 myocardial infarction. STEMI and NSTEMI were associated with increased in-hospital mortality (OR, 8.96; 95% CI, 6.20-12.96; P < .001 and OR, 1.59; 95% CI, 1.34-1.89; P < .001). A diagnosis of type 2 myocardial infarction was not associated with increased odds of in-hospital mortality (OR, 1.11; 95% CI, 0.81-1.53; P = .50) when accounting for surgical procedure, medical comorbidities, patient demographics, and hospital characteristics.
Conclusions: The frequency of perioperative myocardial infarctions did not increase after the introduction of a new diagnostic code for type 2 myocardial infarctions. A diagnosis of type 2 myocardial infarction was not associated with increased in-patient mortality; however, few patients received invasive management that may have confirmed the diagnosis. Further research is needed to identify what type of intervention, if any, may improve outcomes in this patient population.
Copyright © 2023 International Anesthesia Research Society.
Conflict of interest statement
Conflicts of Interest: See Disclosures at the end of the article.
Figures

Similar articles
-
Are there sex differences in the effect of type 2 diabetes in the incidence and outcomes of myocardial infarction? A matched-pair analysis using hospital discharge data.Cardiovasc Diabetol. 2021 Apr 22;20(1):81. doi: 10.1186/s12933-021-01273-y. Cardiovasc Diabetol. 2021. PMID: 33888124 Free PMC article.
-
Presentation, management and mortality after a first MI in people with and without asthma: A study using UK MINAP data.Chron Respir Dis. 2018 Feb;15(1):60-70. doi: 10.1177/1479972317702140. Epub 2017 Apr 10. Chron Respir Dis. 2018. PMID: 28393591 Free PMC article.
-
In-Hospital Bleeding Outcomes of Myocardial Infarction in the Era of Warfarin and Direct Oral Anticoagulants for Atrial Fibrillation in the United States: A Report From the National Cardiovascular Data Registry Acute Coronary Treatment and Intervention Outcomes Network Registry.J Am Heart Assoc. 2019 Apr 16;8(8):e011606. doi: 10.1161/JAHA.118.011606. J Am Heart Assoc. 2019. PMID: 30955406 Free PMC article.
-
Temporal Trends and Outcomes of Mechanical Complications in Patients With Acute Myocardial Infarction.JACC Cardiovasc Interv. 2019 Sep 23;12(18):1825-1836. doi: 10.1016/j.jcin.2019.04.039. JACC Cardiovasc Interv. 2019. PMID: 31537282
-
Racial Disparities in Diagnostic Evaluation and Revascularization in Patients With Acute Myocardial Infarction-A 15-Year Longitudinal Study.Curr Probl Cardiol. 2023 Aug;48(8):101733. doi: 10.1016/j.cpcardiol.2023.101733. Epub 2023 Apr 10. Curr Probl Cardiol. 2023. PMID: 37040853 Review.
Cited by
-
Frequency and Impact of Cardiology Evaluation Following Perioperative Myocardial Infarction.Clin Cardiol. 2025 Mar;48(3):e70120. doi: 10.1002/clc.70120. Clin Cardiol. 2025. PMID: 40116161 Free PMC article.
-
Perioperative Mortality: A Retrospective Cohort Study of 75,446 Noncardiac Surgery Patients.Mayo Clin Proc Innov Qual Outcomes. 2024 Aug 21;8(5):435-442. doi: 10.1016/j.mayocpiqo.2024.07.002. eCollection 2024 Oct. Mayo Clin Proc Innov Qual Outcomes. 2024. PMID: 39263428 Free PMC article.
References
-
- Devereaux PJ, Biccard BM, Sigamani A, et al. Association of Postoperative High-Sensitivity Troponin Levels With Myocardial Injury and 30-Day Mortality Among Patients Undergoing Noncardiac Surgery. Jama. 2017;317(16):1642–1651. - PubMed
-
- Botto F, Alonso-Coello P, Chan MT, et al. Myocardial injury after noncardiac surgery: a large, international, prospective cohort study establishing diagnostic criteria, characteristics, predictors, and 30-day outcomes. Anesthesiology. 2014;120(3):564–578. - PubMed
-
- Thygesen K, Alpert JS, Jaffe AS, et al. Fourth Universal Definition of Myocardial Infarction (2018). Journal of the American College of Cardiology. 2018;72(18):2231–2264. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

