Oncological and functional outcomes of organ-preserving cystectomy versus standard radical cystectomy: A systematic review and meta-analysis
- PMID: 36816151
- PMCID: PMC9931545
- DOI: 10.1002/bco2.189
Oncological and functional outcomes of organ-preserving cystectomy versus standard radical cystectomy: A systematic review and meta-analysis
Abstract
Introduction: Radical cystectomy (RC) is historically considered the gold standard treatment for muscle invasive and high-risk non-muscle invasive bladder cancer. However, this technique leaves the majority of patients of both sexes with poor sexual and urinary function. Organ-sparing cystectomy (OSC) techniques are emerging as an alternative to the standard procedure to preserve these functions, without compromising the oncological outcomes. We present a systematic review and meta-analysis of the published literature.
Methods: MEDLINE, Embase and Web of Science were systematically searched for eligible studies on 6 April 2021. Primary outcomes studied were both oncological outcomes, specifically overall recurrence, and functional outcomes, specifically sexual function, and daytime and nighttime continence. Odds ratios (OR) with 95% confidence intervals (95% CI) were calculated. The PROSPERO registration reference number was CRD42018118897.
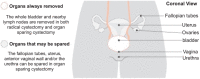
Results: From 13 894 identified abstracts, 19 studies (1886 male and 305 female patients) were eligible for inclusion in this review. These studies included patients who underwent either whole prostate, prostate capsule, seminal vesicle, nerve, uterus, ovary, vagina and fallopian tube sparing techniques. Four studies included only female patients.Thirteen studies reported oncological outcomes, and overall recurrence rate was similar between the two groups (five studies; OR 0.73; 95% CI 0.38-1.40, p = 0.34). Thirteen studies reported on male sexual function. In men, OSC had significantly greater odds of retaining potency (five studies; OR 9.05; 95% CI 5.07-16.16, p < 0.00001). Fourteen studies (13 on males and 1 female) reported urinary outcomes. In men, OSC demonstrated greater odds of daytime (seven studies; OR 2.61; 95% CI 1.74 to 3.92, p < 0.00001) and nighttime continence (seven studies; OR 2.62; 95% CI 1.76 to 3.89, p < 0.00001).
Conclusion: In carefully selected patients, OSC allows the potential to provide better sexual and urinary function without compromising oncological outcomes. There remains, however, a paucity of OSC studies in females. Further studies are required to make recommendations based on robust clinical evidence.
Keywords: continence; cystectomy; functional; oncological; organ sparing; radical; review; sexual; urology.
© 2022 The Authors. BJUI Compass published by John Wiley & Sons Ltd on behalf of BJU International Company.
Conflict of interest statement
All authors declare no conflicts of interest as per the ICMJE COI.
Figures





References
-
- Witjes JA, Bruins M, Cathomas R, Compérat E, Cowan NC, Gakis G, et al. EAU guidelines on muscle‐invasive and metastatic bladder cancer. Edn. presented at EAU Annual Congress Barcelona 2019. ISBN 978‐94‐92671‐04‐2.
-
- Babjuk M, Burger M, Compérat EM , Gontero P, Mostafid A, Palou J, et al. EAU guidelines on nonmuscle‐invasive bladder cancer. Edn. presented at EAU Annual Congress Barcelona 2019. ISBN 978‐94‐92671‐04‐2.
-
- Zippe C, Raina R, Massanyi E, Agarwal A, Jones JS, Ulchaker J, et al. Sexual function after male radical cystectomy in a sexually active population. Urology. 2004;64(4):682–5. - PubMed
-
- Nordström G, Nyman C. Male and female sexual function and activity following ileal conduit urinary diversion. Br J Urol. 1992;70(1):33–9. - PubMed
-
- Ali A, Hayes M, Birch B, Dudderidge T, Somani B. Health related quality of life (HRQoL) after cystectomy: Comparison between orthotopic neobladder and ileal conduit diversion. Eur J Surg Oncol. 2015;41(3):295–9. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous
