Acute Effects of Ketamine on Intracranial Pressure in Children With Severe Traumatic Brain Injury
- PMID: 36825892
- PMCID: PMC11441348
- DOI: 10.1097/CCM.0000000000005806
Acute Effects of Ketamine on Intracranial Pressure in Children With Severe Traumatic Brain Injury
Abstract
Objectives: The acute cerebral physiologic effects of ketamine in children have been incompletely described. We assessed the acute effects of ketamine on intracranial pressure (ICP) and cerebral perfusion pressure (CPP) in children with severe traumatic brain injury (TBI).
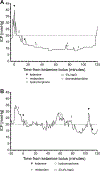
Design: In this retrospective observational study, patients received bolus doses of ketamine for sedation or as a treatment for ICP crisis (ICP > 20 mm Hg for > 5 min). Administration times were synchronized with ICP and CPP recordings at 1-minute intervals logged in an automated database within the electronic health record. ICP and CPP were each averaged in epochs following drug administration and compared with baseline values. Age-based CPP thresholds were subtracted from CPP recordings and compared with baseline values. Trends in ICP and CPP over time were assessed using generalized least squares regression.
Setting: A 30-bed tertiary care children's hospital PICU.
Patients: Children with severe TBI who underwent ICP monitoring.
Interventions: None.
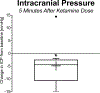
Measurements and main results: We analyzed data from 33 patients, ages 1 month to 16 years, 22 of whom received bolus doses of ketamine, with 127 doses analyzed. Demographics, patient, and injury characteristics were similar between patients who did versus did not receive ketamine boluses. In analysis of the subset of ketamine doses used only for sedation, there was no significant difference in ICP or CPP from baseline. Eighteen ketamine doses were given during ICP crises in 11 patients. ICP decreased following these doses and threshold-subtracted CPP rose.
Conclusions: In this retrospective, exploratory study, ICP did not increase following ketamine administration. In the setting of a guidelines-based protocol, ketamine was associated with a reduction in ICP during ICP crises. If these findings are reproduced in a larger study, ketamine may warrant consideration as a treatment for intracranial hypertension in children with severe TBI.
Copyright © 2023 by the Society of Critical Care Medicine and Wolters Kluwer Health, Inc. All Rights Reserved.
Conflict of interest statement
Dr. Betters’ institution received funding from the National Institutes of Health (R61HL151951). Dr. Wellons disclosed the off-label product use of ketamine for intracranial pressure. Dr. Slaughter received funding from the Department of Pediatrics for statistical support. The remaining authors have disclosed that they do not have any potential conflicts of interest.
Figures
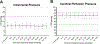

Comment in
-
The Evolution of Ketamine in Severe Pediatric Traumatic Brain Injury, From Contraband to Promising Neuroprotectant?Crit Care Med. 2023 May 1;51(5):677-680. doi: 10.1097/CCM.0000000000005826. Epub 2023 Apr 13. Crit Care Med. 2023. PMID: 37052437 No abstract available.
References
-
- Dewan MC, Mummareddy N, Wellons JC 3rd, Bonfield CM. Epidemiology of Global Pediatric Traumatic Brain Injury: Qualitative Review. World Neurosurg. 2016;91:497–509.e1. - PubMed
-
- Centers for Disease Control and Prevention. National Center for Health Statistics: Mortality Data on CDC WONDER. Accessed 2022. Available from: https://wonder.cdc.gov/mcd.html.
-
- Kochanek PM, Tasker RC, Carney N, Totten AM, Adelson PD, Selden NR, et al. Guidelines for the Management of Pediatric Severe Traumatic Brain Injury, Third Edition: Update of the Brain Trauma Foundation Guidelines. Pediatr Crit Care Med. 2019;20(3S Suppl 1):S1–s82. - PubMed
-
- O’Lynnger TM, Shannon CN, Le TM, Greeno A, Chung D, Lamb FS, et al. Standardizing ICU management of pediatric traumatic brain injury is associated with improved outcomes at discharge. J Neurosurg Pediatr. 2016;17(1):19–26. - PubMed
-
- Shein SL, Ferguson NM, Kochanek PM, Bayir H, Clark RS, Fink EL, et al. Effectiveness of Pharmacological Therapies for Intracranial Hypertension in Children With Severe Traumatic Brain Injury--Results From an Automated Data Collection System Time-Synched to Drug Administration. Pediatr Crit Care Med. 2016;17(3):236–45. - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

