Crosstalk between Inflammation and Hemorrhage/Coagulation Disorders in Primary Blast Lung Injury
- PMID: 36830720
- PMCID: PMC9953683
- DOI: 10.3390/biom13020351
Crosstalk between Inflammation and Hemorrhage/Coagulation Disorders in Primary Blast Lung Injury
Abstract
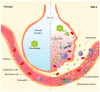
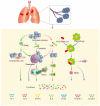
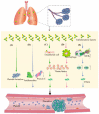
Primary blast lung injury (PBLI), caused by exposure to high-intensity pressure waves from explosions in war, terrorist attacks, industrial production, and life explosions, is associated with pulmonary parenchymal tissue injury and severe ventilation insufficiency. PBLI patients, characterized by diffused intra-alveolar destruction, including hemorrhage and inflammation, might deteriorate into acute respiratory distress syndrome (ARDS) with high mortality. However, due to the absence of guidelines about PBLI, emergency doctors and rescue teams treating PBLI patients rely on experience. The goal of this review is to summarize the mechanisms of PBLI and their cross-linkages, exploring potential diagnostic and therapeutic targets of PBLI. We summarize the pathophysiological performance and pharmacotherapy principles of PBLI. In particular, we emphasize the crosstalk between hemorrhage and inflammation, as well as coagulation, and we propose early control of hemorrhage as the main treatment of PBLI. We also summarize several available therapy methods, including some novel internal hemostatic nanoparticles to prevent the vicious circle of inflammation and coagulation disorders. We hope that this review can provide information about the mechanisms, diagnosis, and treatment of PBLI for all interested investigators.
Keywords: acute lung injury; blast injuries; blood coagulation; hemorrhage; inflammation; therapeutics.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
References
Publication types
MeSH terms
Grants and funding
- TJUWYY2022002/The Scientific Research Translational Foundation of Wenzhou Safety (Emergency) Institute of Tianjin University
- BLB19J006/the Key Project of Applied Basic Research of the Logistics Support Department of the Chinese People's Liberation Army
- 32000877/National Natural Science Foundation of China
LinkOut - more resources
Full Text Sources
Medical
Research Materials

