Healthy and Osteoarthritis-Affected Joints Facing the Cellular Crosstalk
- PMID: 36835530
- PMCID: PMC9964755
- DOI: 10.3390/ijms24044120
Healthy and Osteoarthritis-Affected Joints Facing the Cellular Crosstalk
Abstract
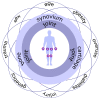
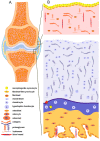
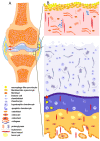
Osteoarthritis (OA) is a chronic, progressive, severely debilitating, and multifactorial joint disease that is recognized as the most common type of arthritis. During the last decade, it shows an incremental global rise in prevalence and incidence. The interaction between etiologic factors that mediate joint degradation has been explored in numerous studies. However, the underlying processes that induce OA remain obscure, largely due to the variety and complexity of these mechanisms. During synovial joint dysfunction, the osteochondral unit undergoes cellular phenotypic and functional alterations. At the cellular level, the synovial membrane is influenced by cartilage and subchondral bone cleavage fragments and extracellular matrix (ECM) degradation products from apoptotic and necrotic cells. These "foreign bodies" serve as danger-associated molecular patterns (DAMPs) that trigger innate immunity, eliciting and sustaining low-grade inflammation in the synovium. In this review, we explore the cellular and molecular communication networks established between the major joint compartments-the synovial membrane, cartilage, and subchondral bone of normal and OA-affected joints.
Keywords: articular cartilage; chondrocytes; molecular signals; osteoarthritis; osteocytes; subchondral bone; synovial membrane; synoviocytes.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
References
-
- Safiri S., Kolahi A.-A., Smith E., Hill C., Bettampadi D., Mansournia M.A., Hoy D., Ashrafi-Asgarabad A., Sepidarkish M., Almasi-Hashiani A., et al. Global, Regional and National Burden of Osteoarthritis 1990-2017: A Systematic Analysis of the Global Burden of Disease Study 2017. Ann. Rheum. Dis. 2020;79:819–828. doi: 10.1136/annrheumdis-2019-216515. - DOI - PubMed
-
- Zheng S., Tu L., Cicuttini F., Zhu Z., Han W., Antony B., Wluka A.E., Winzenberg T., Aitken D., Blizzard L., et al. Depression in Patients with Knee Osteoarthritis: Risk Factors and Associations with Joint Symptoms. BMC Musculoskelet. Disord. 2021;22:40. doi: 10.1186/s12891-020-03875-1. - DOI - PMC - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

