A Prospective Analysis of Vitamin D Levels in Pregnant Women Diagnosed with Gestational Hypertension after SARS-CoV-2 Infection
- PMID: 36836551
- PMCID: PMC9963707
- DOI: 10.3390/jpm13020317
A Prospective Analysis of Vitamin D Levels in Pregnant Women Diagnosed with Gestational Hypertension after SARS-CoV-2 Infection
Abstract
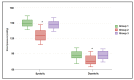
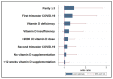
The great majority of existing studies suggests that the prognosis and outcomes of SARS-CoV-2 infections are improved with adequate vitamin D levels, with or without supplementation. Simultaneously, whether vitamin D supplementation during pregnancy lessens the chance of developing gestational hypertension is controversial. The objective of the present research was to evaluate whether vitamin D levels during pregnancy differ substantially among pregnant women who develop gestational hypertension following SARS-CoV-2 infection. The current research was designed as a prospective cohort following the pregnant women admitted to our clinic with COVID-19 until 36 weeks of gestation. Total vitamin D (25(OH)D) levels were measured in the three study groups in which pregnant women with COVID-19 during pregnancy and a diagnosis of hypertension after 20 weeks of gestation were considered the group of cases (GH-CoV). The second group (CoV) included those with COVID-19 and no hypertension, while the third group (GH) included those with hypertension and no COVID-19. It was observed that 64.4% of SARS-CoV-2 infections in the group of cases occurred during the first trimester, compared to 29.2% in the first trimester among the controls who did not develop GH. Normal vitamin D levels were measured at admission in a significantly higher proportion of pregnant women without GH (68.8% in the CoV group vs. 47.9% in the GH-CoV group and 45.8% in the GH group). At 36 weeks of gestation, the median values of 25(OH)D in the CoV group was 34.4 (26.9-39.7) ng/mL compared to 27.9 (16.2-32.4) ng/mL in the GH-CoV group and 29.5 ng/mL (18.4-33.2) in the GH group, while the blood pressure measurements remained over 140 mmHg among the groups who developed GH. There was a statistically significant negative association between serum 25(OH)D levels and systolic blood pressure (rho = -0.295; p-value = 0.031); however, the risk of developing GH was not significantly higher among pregnant women with COVID-19 if the vitamin D levels were insufficient (OR = 1.19; p-value = 0.092) or deficient (OR = 1.26; p-value = 0.057). Although insufficient or deficient vitamin D among pregnant women with COVID-19 was not an independent risk factor for the development of GH, it is likely that an association between first-trimester SARS-CoV-2 infection and low vitamin D plays a key role in developing gestational hypertension.
Keywords: COVID-19; SARS-CoV-2; gestational hypertension; pregnancy infections; vitamin D.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

References
-
- Ford N.D., Cox S., Ko J.Y., Ouyang L., Romero L., Colarusso T., Ferre C.D., Kroelinger C.D., Hayes D.K., Barfield W.D. Hypertensive Disorders in Pregnancy and Mortality at Delivery Hospitalization—United States, 2017–2019. MMWR Morb. Mortal. Wkly. Rep. 2022;71:585–591. doi: 10.15585/mmwr.mm7117a1. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

