Do Patients with Bronchiectasis Have an Increased Risk of Developing Lung Cancer? A Systematic Review
- PMID: 36836816
- PMCID: PMC9961135
- DOI: 10.3390/life13020459
Do Patients with Bronchiectasis Have an Increased Risk of Developing Lung Cancer? A Systematic Review
Abstract
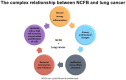
Background: Initial evidence supports the hypothesis that patients with non-cystic fibrosis bronchiectasis (NCFB) have a higher risk of lung cancer. We systematically reviewed the available literature to define the characteristics of lung malignancies in patients with bronchiectasis and the characteristics of patients who develop bronchiectasis-associated lung cancer.
Method: This study was performed based on the PRISMA guidelines. The review protocol was registered in PROSPERO.
Results: The frequency rates of lung cancer in patients with NCFB ranged from 0.93% to 8.0%. The incidence rate was 3.96. Cancer more frequently occurred in the elderly and males. Three studies found an overall higher risk of developing lung cancer in the NCFB population compared to the non-bronchiectasis one, and adenocarcinoma was the most frequently reported histological type. The effect of the co-existence of NCFB and COPD was unclear.
Conclusions: NCFB is associated with a higher risk of developing lung cancer than individuals without NCFB. This risk is higher for males, the elderly, and smokers, whereas concomitant COPD's effect is unclear.
Keywords: COPD; bronchiectasis; hazard risk; lung cancer.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

References
-
- McDonnell M.J., Aliberti S., Goeminne P.C., Restrepo M.I., Finch S., Pesci A., Dupont L.J., Fardon T.C., Wilson R., Loebinger M.R., et al. Comorbidities and the risk of mortality in patients with bronchiectasis: An international multicentre cohort study. Lancet Respir. Med. 2016;4:969–979. doi: 10.1016/S2213-2600(16)30320-4. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources

