Characteristics, management, and blood pressure control in patients with apparent resistant hypertension in the US
- PMID: 36846680
- PMCID: PMC9950828
- DOI: 10.1016/j.heliyon.2023.e13258
Characteristics, management, and blood pressure control in patients with apparent resistant hypertension in the US
Abstract
Background: Per treatment guidelines, resistant hypertension is defined as uncontrolled blood pressure (BP) while taking 3 concomitant antihypertensives (AHTs) or controlled BP while taking ≥4 AHTs. Characteristics, AHT therapy use, and BP control were analyzed in US patients with hypertension who were prescribed ≥3 classes of AHT medications.
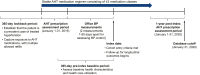
Methods: This retrospective analysis of the Optum® Electronic Health Record Database evaluated patients ≥18 years of age with a diagnosis of hypertension classified based on the number of prescribed AHT medication classes (3, 4, or ≥5). For the primary analysis, uncontrolled hypertension was defined as systolic BP (SBP) ≥140 mmHg or diastolic BP (DBP) ≥90 mmHg. For secondary analyses, uncontrolled hypertension was defined as SBP ≥130 mmHg or DBP ≥80 mmHg.
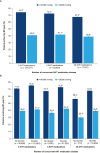
Results: 207,705 patients with hypertension and concurrent use of ≥3 AHT medication classes were included. Diuretics, beta blockers, ACE inhibitors and/or ARBs, and CCBs were the most prescribed classes; thiazides and thiazide-like agents were the most prescribed diuretics. Among patients who were prescribed 3, 4, or ≥5 AHT medication classes, approximately 70% achieved a BP goal of <140/90 mmHg; approximately 40% achieved BP <130/80 mmHg. After ≥1 year of follow-up, the number of concurrent AHT medication classes was unchanged from baseline in the majority of patients and the prevalence of uncontrolled hypertension (≥140/90 mmHg) was similar.
Conclusions: This study illustrates suboptimal BP control in many patients with apparent resistant hypertension despite the use of multidrug regimens and suggests a need for new drug classes and regimens that effectively manage resistant hypertension.
© 2023 The Authors.
Conflict of interest statement
The authors declare the following conflict of interests: EMA, ESO, DM, AAK, WC, and LH are employees of Janssen and may be Johnson & Johnson stockholders. DAT is an employee of Idorsia Pharmaceuticals and is an Idorsia stockholder. NSA has provided consultancy advice to Janssen.
Figures


References
-
- Forouzanfar M.H., Liu P., Roth G.A., et al. Global burden of hypertension and systolic blood pressure of at least 110 to 115 mm Hg, 1990-2015. JAMA. 2017;317(2):165–182. - PubMed
-
- Noubiap J.J., Nansseu J.R., Nyaga U.F., Sime P.S., Francis I., Bigna J.J. Global prevalence of resistant hypertension: a meta-analysis of data from 3.2 million patients. Heart. 2019;105(2):98–105. - PubMed
-
- Persell S.D. Prevalence of resistant hypertension in the United States, 2003-2008. Hypertension. 2011;57(6):1076–1080. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

