Association of Evaluation and Management Payment Policy Changes With Medicare Payment to Physicians by Specialty
- PMID: 36853249
- PMCID: PMC9975918
- DOI: 10.1001/jama.2023.0879
Association of Evaluation and Management Payment Policy Changes With Medicare Payment to Physicians by Specialty
Abstract
Importance: US primary care physicians (PCPs) have lower mean incomes than specialists, likely contributing to workforce shortages. In 2021, the Centers for Medicare & Medicaid Services increased payment for evaluation and management (E/M) services and relaxed documentation requirements. These changes may have reduced the gap between primary care and specialist payment.
Objectives: To simulate the effect of the E/M payment policy change on total Medicare physician payments while holding volume constant and to compare these simulated changes with observed changes in total Medicare payments and E/M coding intensity, before (July-December 2020) and after (July-December 2021) the E/M payment policy change.
Design, setting, and participants: Retrospective observational study of US office-based physicians who were in specialties with 5000 or more physicians billing Medicare and who had 50 or more fee-for-service Medicare visits before and after the E/M payment policy change.
Exposures: E/M payment policy changes.
Main outcomes and measures: Outcomes included physician-level simulated volume-constant payment change, total observed Medicare payment change, and share of high-intensity (ie, level 4 or 5) E/M visits before and after the E/M payment policy change. For each specialty, the median change in each outcome was reported. The payment gap between primary care and specialty physicians was calculated as the difference between total Medicare payments to the median primary care and median specialty physician.
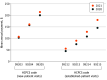
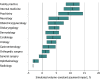
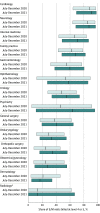
Results: The study population included 180 624 physicians. Repricing 2020 services yielded a simulated volume-constant payment change ranging from a 3.3% (-$4557.0) decrease for the median radiologist to an 11.0% ($3683.1) increase for the median family practice physician. After the E/M payment change, the median high-intensity share of E/M visits increased for physicians of nearly all specialties, ranging from a -4.4 percentage point increase (dermatology) to a 17.8 percentage point increase (psychiatry). The median change in total Medicare payments by specialty ranged from -4.2% (-$1782.9) for general surgery to 12.1% ($3746.9) for family practice. From July-December 2020 to July-December 2021, the payment gap between the median primary care physician and the median specialist shrank by $825.1, from $40 259.8 to $39 434.7 (primary care, $41 193.3 in July-December 2020 and $45 962.4 in July-December 2021; specialist, $81 453.1 in July-December 2020 and $85 397.1 in July-December 2021)-a relative decrease of 2.0%.
Conclusions and relevance: Among US office-based physicians receiving Medicare payments in 2020 and 2021, E/M payment policy changes were associated with changes in Medicare payment by specialty, although the payment gap between primary care physicians and specialists decreased only modestly. The findings may have been influenced by the COVID-19 pandemic, and further research in subsequent years is needed.
Conflict of interest statement
Figures


Comment in
-
Payment, Priorities, and Primary Care: Can Cognitive Work Be Properly Valued?JAMA. 2023 Feb 28;329(8):635-636. doi: 10.1001/jama.2023.0880. JAMA. 2023. PMID: 36853258 No abstract available.
-
Beyond the AJR: Evaluation and Management Payment Policy Changes Redistributed Money From Radiologists to Primary Care Practitioners.AJR Am J Roentgenol. 2024 Jan;222(1):e2329560. doi: 10.2214/AJR.23.29560. Epub 2023 May 10. AJR Am J Roentgenol. 2024. PMID: 37162039 No abstract available.
References
-
- Laugesen MJ. Fixing Medical Prices: How Physicians Are Paid. Harvard University Press; 2016. doi: 10.4159/9780674545380 - DOI
-
- Zuckerman S, Shartzer A, Berenson RA, Marks K, Das S, Brandt C. Analysis of Disparities in Physician Compensation: A Report by the Urban Institute and SullivanCotter for the Medicare Payment Advisory Commission. Medicare Payment Advisory Commission. Published January 2019. Accessed January 27, 2023. https://www.medpac.gov/document/http-www-medpac-gov-docs-default-source-...
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

