Robot-assisted implantation of additively manufactured patient-specific orthopaedic implants: evaluation in a sheep model
- PMID: 36859520
- PMCID: PMC10497442
- DOI: 10.1007/s11548-023-02848-8
Robot-assisted implantation of additively manufactured patient-specific orthopaedic implants: evaluation in a sheep model
Abstract
Purpose: Bone tumours must be surgically excised in one piece with a margin of healthy tissue. The unique nature of each bone tumour case is well suited to the use of patient-specific implants, with additive manufacturing allowing production of highly complex geometries. This work represents the first assessment of the combination of surgical robotics and patient-specific additively manufactured implants.
Methods: The development and evaluation of a robotic system for bone tumour excision, capable of milling complex osteotomy paths, is described. The developed system was evaluated as part of an animal trial on 24 adult male sheep, in which robotic bone excision of the distal femur was followed by placement of patient-specific implants with operative time evaluated. Assessment of implant placement accuracy was completed based on post-operative CT scans.
Results: A mean overall implant position error of 1.05 ± 0.53 mm was achieved, in combination with a mean orientation error of 2.38 ± 0.98°. A mean procedure time (from access to implantation, excluding opening and closing) of 89.3 ± 25.25 min was observed, with recorded surgical time between 58 and 133 min, with this approximately evenly divided between robotic (43.9 ± 15.32) and implant-based (45.4 ± 18.97) tasks.
Conclusions: This work demonstrates the ability for robotics to achieve repeatable and precise removal of complex bone volumes of the type that would allow en bloc removal of a bone tumour. These robotically created volumes can be precisely filled with additively manufactured patient-specific implants, with minimal gap between cut surface and implant interface.
Keywords: Bone tumours; Orthopaedic oncology; Patient-specific implants; Robotic surgery; Surgical robotics.
© 2023. The Author(s).
Conflict of interest statement
Stryker is a partner in the IMCRC initiative. Dave Hill, Tom Williamson, Peter Choong, Martin Leary, Darpan Shidid and Milan Brandt are co-authors on patents or patent applications related to the technology described in this work. Peter Choong provides consulting work with Stryker. Zac Sweeney and Ulrich Buehner were employed by Stryker during the period during which this work was completed. Stewart Ryan, Bill Lozanovski, Endri Kastrati, Arman Namvar, Thierry Beths, Romane Blanchard and Kate Fox declare that they have no competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures

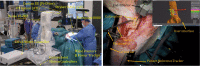






References
-
- Cancer data in Australia, Summary, Australian institute of health and welfare. https://www.aihw.gov.au/reports/cancer/cancer-data-in-australia/contents.... Accessed 30 Aug 2022.
-
- Shidid D, Leary M, Choong P, Brandt M. Just-in-time design and additive manufacture of patient-specific medical implants. Phys Procedia. 2016;83:4–14. doi: 10.1016/j.phpro.2016.08.002. - DOI
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

