Habitually Skipping Breakfast Is Associated with the Risk of Gastrointestinal Cancers: Evidence from the Kailuan Cohort Study
- PMID: 36869181
- PMCID: PMC10465444
- DOI: 10.1007/s11606-023-08094-7
Habitually Skipping Breakfast Is Associated with the Risk of Gastrointestinal Cancers: Evidence from the Kailuan Cohort Study
Abstract
Background: Habitually skipping breakfast may promote the initiation and progression of gastrointestinal (GI) cancers, which have never been systematically explored in large-scale prospective studies.
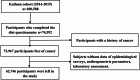
Methods: We prospectively examined the effects of breakfast frequency on the occurrence of GI cancers among 62,746 participants. The hazard ratios (HRs) and 95% confidence intervals (95% CIs) of GI cancers were calculated by Cox regression. The CAUSALMED procedure was used to perform the mediation analyses.
Results: During a median follow-up of 5.61 (5.18 ~ 6.08) years, 369 incident GI cancer cases were identified. Participants who consumed 1-2 times breakfasts per week exhibited an increased risk of stomach (HR = 3.45, 95% CI: 1.06-11.20) and liver cancer (HR = 3.42, 95% CI: 1.22-9.53). Participants who did not eat breakfast had an elevated risk of esophageal (HR = 2.72, 95% CI: 1.05-7.03), colorectal (HR = 2.32, 95% CI: 1.34-4.01), liver (HR = 2.41, 95% CI: 1.23-4.71), gallbladder, and extrahepatic bile duct cancer (HR = 5.43, 95% CI: 1.34-21.93). In the mediation effect analyses, BMI, CRP, and TyG (fasting triglyceride-glucose) index did not mediate the association between breakfast frequency and the risk of GI cancer incidence (all P for mediation effect > 0.05).
Conclusions: Habitually skipping breakfast was associated with a greater risk of GI cancers including esophageal, gastric, colorectal, liver, gallbladder, and extrahepatic bile duct cancer.
Trial registration: Kailuan study, ChiCTR-TNRC-11001489. Registered 24 August, 2011-Retrospectively registered, http://www.chictr.org.cn/showprojen.aspx?proj=8050.
Keywords: Breakfast; Frequency; Gastrointestinal cancer; Prospective.
© 2023. The Author(s).
Conflict of interest statement
The authors declare that they do not have a conflict of interest.
Figures
Similar articles
-
Hepatitis B virus infection and the risk of gastrointestinal cancers among Chinese population: A prospective cohort study.Int J Cancer. 2022 Mar 15;150(6):1018-1028. doi: 10.1002/ijc.33891. Epub 2021 Dec 14. Int J Cancer. 2022. PMID: 34855203 Free PMC article.
-
Associations between hepatitis B virus infection and risk of colorectal Cancer: a population-based prospective study.BMC Cancer. 2021 Oct 18;21(1):1119. doi: 10.1186/s12885-021-08846-w. BMC Cancer. 2021. PMID: 34663268 Free PMC article.
-
Association between metabolic syndrome, C-reactive protein, and the risk of primary liver cancer: a large prospective study.BMC Cancer. 2022 Aug 4;22(1):853. doi: 10.1186/s12885-022-09939-w. BMC Cancer. 2022. PMID: 35927639 Free PMC article.
-
Meta-Analysis of Relation of Skipping Breakfast With Heart Disease.Am J Cardiol. 2019 Sep 15;124(6):978-986. doi: 10.1016/j.amjcard.2019.06.016. Epub 2019 Jun 25. Am J Cardiol. 2019. PMID: 31326073 Review.
-
Association between Periodontal Diseases and the Risk of Site-Specific Gastrointestinal Cancers: A Systematic Review and Meta-Analysis.J Dent Res. 2024 Sep;103(10):962-972. doi: 10.1177/00220345241263768. Epub 2024 Aug 26. J Dent Res. 2024. PMID: 39185624
Cited by
-
MASLD treatment-a shift in the paradigm is imminent.Front Med (Lausanne). 2023 Dec 11;10:1316284. doi: 10.3389/fmed.2023.1316284. eCollection 2023. Front Med (Lausanne). 2023. PMID: 38146424 Free PMC article. Review.
-
Does breakfast skipping alter the serum lipids of university students?BMC Nutr. 2025 Mar 7;11(1):51. doi: 10.1186/s40795-024-00970-7. BMC Nutr. 2025. PMID: 40055812 Free PMC article.
-
Predictive Mortality and Gastric Cancer Risk Using Clinical and Socio-Economic Data: A Nationwide Multicenter Cohort Study.Cancers (Basel). 2024 Dec 25;17(1):30. doi: 10.3390/cancers17010030. Cancers (Basel). 2024. PMID: 39796661 Free PMC article.
-
In utero and childhood exposure to the great Chinese famine and risk of aging in adulthood.Sci Rep. 2024 Oct 23;14(1):25089. doi: 10.1038/s41598-024-77283-z. Sci Rep. 2024. PMID: 39443668 Free PMC article.
-
Meta-analysis of postoperative incision infection risk factors in colorectal cancer surgery.Front Surg. 2024 Aug 13;11:1415357. doi: 10.3389/fsurg.2024.1415357. eCollection 2024. Front Surg. 2024. PMID: 39193402 Free PMC article.
References
-
- Global, regional, and national comparative risk assessment of 84 behavioural, environmental and occupational, and metabolic risks or clusters of risks for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet, 2018. 392(10159): p. 1923–1994. - PMC - PubMed
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous