Different monoclonal antibodies and immunosuppressants administration in patients with neuromyelitis optica spectrum disorder: a Bayesian network meta-analysis
- PMID: 36884069
- PMCID: PMC10188410
- DOI: 10.1007/s00415-023-11641-1
Different monoclonal antibodies and immunosuppressants administration in patients with neuromyelitis optica spectrum disorder: a Bayesian network meta-analysis
Abstract
Background: A variety of novel monoclonal antibodies and immunosuppressant have been proved effective in treating Neuromyelitis Optica Spectrum Disorder (NMOSD). This network meta-analysis compared and ranked the efficacy and tolerability of currently used monoclonal antibodies and immunosuppressive agents in NMOSD.
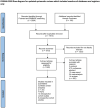
Methods: Electronic database including PubMed, Embase and Cochrane Library were searched for relevant studies evaluating monoclonal antibodies and immunosuppressants in patients with NMOSD. The primary outcome measures were annualized relapse rate (ARR), relapse rate, the Expanded Disability Status Scale (EDSS) score, and total adverse events (AEs).
Results: We identified 25 studies with 2919 patients in our meta-analysis. For the primary outcome, rituximab (RTX) (SUCRA: 0.02) ranked first in reduction ARR with a significant difference compared with azathioprine (AZA) (MD - 0.34, 95% CrI - 0.55 to - 0.12) and mycophenolate mofetil (MMF) (MD -0.38, 95% CrI - 0.63 to - 0.14). Tocilizumab (SUCRA: 0.05) ranked first in relapse rate, which was superior to satralizumab (lnOR - 25.4, 95% CrI - 74.4 to - 2.49) and inebilizumab (lnOR - 24.86, 95% CrI - 73.75 to - 1.93). MMF (SUCRA: 0.27) had the fewest AEs followed by RTX (SUCRA: 0.35), both of which showed a significant difference compared with AZA and corticosteroids (MMF vs AZA: lnOR - 1.58, 95% CrI - 2.48 to - 0.68; MMF vs corticosteroids: lnOR - 1.34, 95% CrI - 2.3 to - 0.37) (RTX vs AZA: lnOR - 1.34, 95% CrI - 0.37 to - 2.3; RTX vs corticosteroids: lnOR - 2.52, 95% CrI - 0.32 to - 4.86). In EDSS score, no statistical difference was found between different interventions.
Conclusion: RTX and tocilizumab showed better efficacy than traditional immunosuppressants in reducing relapse. For safety, MMF and RTX had fewer AEs. However, studies with larger sample size on newly developed monoclonal antibodies are warranted in the future.
Keywords: AZA; Meta-analysis; Neuromyelitis optica spectrum disorder; RTX; Relapse.
© 2023. The Author(s).
Conflict of interest statement
All authors declare that there were no competing interests.
Figures





Similar articles
-
Evaluation of effect of empirical attack-preventive immunotherapies in neuromyelitis optica spectrum disorders: An update systematic review and meta -analysis.J Neuroimmunol. 2022 Feb 15;363:577790. doi: 10.1016/j.jneuroim.2021.577790. Epub 2021 Dec 16. J Neuroimmunol. 2022. PMID: 34959021
-
Comparison of efficacy and tolerability of azathioprine, mycophenolate mofetil, and lower dosages of rituximab among patients with neuromyelitis optica spectrum disorder.J Neurol Sci. 2018 Feb 15;385:192-197. doi: 10.1016/j.jns.2017.12.034. Epub 2017 Dec 30. J Neurol Sci. 2018. PMID: 29406904
-
Efficacy and safety of modified reduced-dose rituximab in Chinese patients with neuromyelitis optica spectrum disorder: A retrospective cohort study.J Neurol Sci. 2021 Oct 15;429:117616. doi: 10.1016/j.jns.2021.117616. Epub 2021 Aug 12. J Neurol Sci. 2021. PMID: 34450520
-
Immunotherapy for neuromyelitis optica spectrum disorder: a comparative analysis of efficacy and safety of azathioprine, mycophenolate mofetil, tacrolimus, and rituximab.Front Neurol. 2025 Apr 28;16:1559118. doi: 10.3389/fneur.2025.1559118. eCollection 2025. Front Neurol. 2025. PMID: 40356634 Free PMC article.
-
Effectiveness and tolerability of immunosuppressants and monoclonal antibodies in preventive treatment of neuromyelitis optica spectrum disorders: A systematic review and network meta-analysis.Mult Scler Relat Disord. 2019 Oct;35:246-252. doi: 10.1016/j.msard.2019.08.009. Epub 2019 Aug 9. Mult Scler Relat Disord. 2019. PMID: 31425902
Cited by
-
Treatment access and satisfaction on disease-modifying therapies of neuromyelitis optica spectrum disorder patients in China: a cross-sectional survey.Ther Adv Neurol Disord. 2024 Mar 23;17:17562864241239105. doi: 10.1177/17562864241239105. eCollection 2024. Ther Adv Neurol Disord. 2024. PMID: 38525489 Free PMC article.
-
A real-world study on the utility of regular rituximab treatment for neuromyelitis optica spectrum disorder.J Neurol. 2025 Feb 11;272(3):194. doi: 10.1007/s00415-025-12937-0. J Neurol. 2025. PMID: 39932569
-
Immunotherapies in neuromyelitis optica: Bayesian network meta-analysis.J Neurol. 2025 Aug 8;272(9):563. doi: 10.1007/s00415-025-13279-7. J Neurol. 2025. PMID: 40775082 Free PMC article.
-
Relapse risk after rituximab discontinuation in neuromyelitis optica spectrum disorders: a multi-center retrospective cohort study.J Neurol. 2025 May 10;272(6):387. doi: 10.1007/s00415-025-13125-w. J Neurol. 2025. PMID: 40348903
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

