Does deep neuromuscular blockade provide improved perioperative outcomes in adult patients? A systematic review and meta-analysis of randomized controlled trials
- PMID: 36893114
- PMCID: PMC9997990
- DOI: 10.1371/journal.pone.0282790
Does deep neuromuscular blockade provide improved perioperative outcomes in adult patients? A systematic review and meta-analysis of randomized controlled trials
Abstract
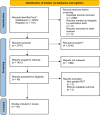
Deep neuromuscular blockade provides better surgical workspace conditions in laparoscopic surgery, but it is still not clear whether it improves perioperative outcomes, not to mention its role in other types of surgeries. We performed this systematic review and meta-analysis of randomized controlled trials to investigate whether deep neuromuscular blockade versus other more superficial levels of neuromuscular blockade provides improved perioperative outcomes in adult patients in all types of surgeries. Medline, Embase, Cochrane Central Register of Controlled Trials, and Google Scholar were searched from inception to June 25, 2022. Forty studies (3271 participants) were included. Deep neuromuscular blockade was associated with an increased rate of acceptable surgical condition (relative risk [RR]: 1.19, 95% confidence interval [CI]: [1.11, 1.27]), increased surgical condition score (MD: 0.52, 95% CI: [0.37, 0.67]), decreased rate of intraoperative movement (RR: 0.19, 95% CI: [0.10, 0.33]), fewer additional measures to improve the surgical condition (RR: 0.63, 95% CI: [0.43, 0.94]), and decreased pain score at 24 h (MD: -0.42, 95% CI: [-0.74, -0.10]). There was no significant difference in the intraoperative blood loss (MD: -22.80, 95% CI: [-48.83, 3.24]), duration of surgery (MD: -0.05, 95% CI: [-2.05, 1.95]), pain score at 48 h (MD: -0.49, 95% CI: [-1.03, 0.05]), or length of stay (MD: -0.05, 95% CI: [-0.19, 0.08]). These indicate that deep neuromuscular blockade improves surgical conditions and prevents intraoperative movement, and there is no sufficient evidence that deep neuromuscular blockade is associated with intraoperative blood loss, duration of surgery, complications, postoperative pain, and length of stay. More high-quality randomized controlled trials are needed, and more attention should be given to complications and the physiological mechanism behind deep neuromuscular blockade and postoperative outcomes.
Copyright: © 2023 Liu et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
Effects of deep neuromuscular block on surgical workspace conditions in laparoscopic bariatric surgery: a systematic review and meta-analysis of randomized controlled trials.Minerva Anestesiol. 2020 Sep;86(9):957-964. doi: 10.23736/S0375-9393.20.14283-4. Epub 2020 Apr 6. Minerva Anestesiol. 2020. PMID: 32251573
-
Low intra-abdominal pressure and deep neuromuscular blockade laparoscopic surgery and surgical space conditions: A meta-analysis.Medicine (Baltimore). 2020 Feb;99(9):e19323. doi: 10.1097/MD.0000000000019323. Medicine (Baltimore). 2020. PMID: 32118762 Free PMC article.
-
Does deep neuromuscular blockade during laparoscopy procedures change patient, surgical, and healthcare resource outcomes? A systematic review and meta-analysis of randomized controlled trials.PLoS One. 2020 Apr 16;15(4):e0231452. doi: 10.1371/journal.pone.0231452. eCollection 2020. PLoS One. 2020. PMID: 32298304 Free PMC article.
-
Deep neuromuscular block to optimize surgical space conditions during laparoscopic surgery: a systematic review and meta-analysis.Br J Anaesth. 2017 Jun 1;118(6):834-842. doi: 10.1093/bja/aex116. Br J Anaesth. 2017. PMID: 28575335
-
Subcuticular sutures for skin closure in non-obstetric surgery.Cochrane Database Syst Rev. 2020 Apr 9;4(4):CD012124. doi: 10.1002/14651858.CD012124.pub2. Cochrane Database Syst Rev. 2020. PMID: 32271475 Free PMC article.
Cited by
-
Deep neuromuscular blockade in adults undergoing an abdominal laparoscopic procedure.Cochrane Database Syst Rev. 2024 Jan 30;1(1):CD013197. doi: 10.1002/14651858.CD013197.pub2. Cochrane Database Syst Rev. 2024. PMID: 38288876 Free PMC article.
-
Equipotent Dose and Cost Comparison of Atracurium and Rocuronium in Laboratory Pigs Anesthetized with Propofol.Animals (Basel). 2025 Jun 23;15(13):1854. doi: 10.3390/ani15131854. Animals (Basel). 2025. PMID: 40646753 Free PMC article.
-
Impact of temperature on EC50 of ropivacaine in axillary brachial plexus blocks: based on Dixon's up-and-down method.Front Med (Lausanne). 2025 Jul 14;12:1591581. doi: 10.3389/fmed.2025.1591581. eCollection 2025. Front Med (Lausanne). 2025. PMID: 40727531 Free PMC article.
-
Deep Neuromuscular Block with Low Pressure Pneumoperitoneum in Laparoscopic Abdominal Surgeries: A Randomized Controlled Trial.Anesth Pain Med. 2024 Oct 8;14(5):e150995. doi: 10.5812/aapm-150995. eCollection 2024 Oct. Anesth Pain Med. 2024. PMID: 40689105 Free PMC article.
-
Optimizing recovery in orthognathic surgery: the cohort study of impact of rocuronium-sugammadex on extubation and perioperative outcomes.Ann Med. 2025 Dec;57(1):2536201. doi: 10.1080/07853890.2025.2536201. Epub 2025 Jul 21. Ann Med. 2025. PMID: 40689722 Free PMC article.
References
-
- Barrio J, Errando CL, San Miguel G, Salas BI, Raga J, Carrión JL, et al.. Effect of depth of neuromuscular blockade on the abdominal space during pneumoperitoneum establishment in laparoscopic surgery. J Clin Anesth. 2016. Nov;34:197–203. doi: 10.1016/j.jclinane.2016.04.017 Epub 2016 May 11. . - DOI - PubMed
-
- Viby-Mogensen J, Howardy-Hansen P, Chraemmer-Jørgensen B, Ording H, Engbaek J, Nielsen A. Posttetanic count (PTC): a new method of evaluating an intense nondepolarizing neuromuscular blockade. Anesthesiology. 1981. Oct;55(4):458–61. . - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources