A Closer Look at Opioid-Induced Adrenal Insufficiency: A Narrative Review
- PMID: 36902007
- PMCID: PMC10003084
- DOI: 10.3390/ijms24054575
A Closer Look at Opioid-Induced Adrenal Insufficiency: A Narrative Review
Abstract
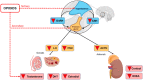
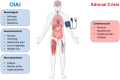
Among several opioid-associated endocrinopathies, opioid-associated adrenal insufficiency (OIAI) is both common and not well understood by most clinicians, particularly those outside of endocrine specialization. OIAI is secondary to long-term opioid use and differs from primary adrenal insufficiency. Beyond chronic opioid use, risk factors for OIAI are not well known. OIAI can be diagnosed by a variety of tests, such as the morning cortisol test, but cutoff values are not well established and it is estimated that only about 10% of patients with OIAI will ever be properly diagnosed. This may be dangerous, as OIAI can lead to a potentially life-threatening adrenal crisis. OIAI can be treated and for patients who must continue opioid therapy, it can be clinically managed. OIAI resolves with opioid cessation. Better guidance for diagnosis and treatment is urgently needed, particularly in light of the fact that 5% of the United States population has a prescription for chronic opioid therapy.
Keywords: adrenal crisis; adrenal insufficiency; chronic pain; endocrine; hypothalamic-pituitary-adrenal axis; opioid use disorder; opioids; pituitary.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

References
-
- Boudreau D., Von Korff M., Rutter C.M., Saunders K., Ray G.T., Sullivan M.D., Campbell C.I., Merrill J.O., Silverberg M.J., Banta-Green C., et al. Trends in long-term opioid therapy for chronic non-cancer pain. Pharmacoepidemiol. Drug Saf. 2009;18:1166–1175. doi: 10.1002/pds.1833. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

