Assessment of Patient Education Delivered at Time of Hospital Discharge
- PMID: 36939674
- PMCID: PMC10028544
- DOI: 10.1001/jamainternmed.2023.0070
Assessment of Patient Education Delivered at Time of Hospital Discharge
Abstract
Importance: Patient education at time of hospital discharge is critical for smooth transitions of care; however, empirical data regarding discharge communication are limited.
Objective: To describe whether key communication domains (medication changes, follow-up appointments, disease self-management, red flags, question solicitation, and teach-back) were addressed at the bedside on the day of hospital discharge, by whom, and for how long.
Design, setting, and participants: This quality improvement study was conducted from September 2018 through October 2019 at inpatient medicine floors in 2 urban, tertiary-care teaching hospitals and purposefully sampled patients designated as "discharge before noon." Data analysis was performed from September 2018 to May 2020.
Exposures: A trained bedside observer documented all content and duration of staff communication with a single enrolled patient from 7 am until discharge.
Main outcomes and measures: Presence of the key communication domains, role of team members, and amount of time spent at the bedside.
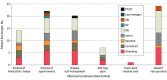
Results: Discharge days for 33 patients were observed. Patients had a mean (SD) age of 63 (18) years; 14 (42%) identified as White, 15 (45%) were female, and 6 (18%) had a preferred language of Spanish. Thirty patients were discharged with at least 1 medication change. Of these patients, 8 (27%) received no verbal instruction on the change, while 16 of 30 (53%) were informed but not told the purpose of the changes. About half of the patients (15 of 31, 48%) were not told the reason for follow-up appointments, and 18 of 33 (55%) were not given instructions on posthospital disease self-management. Most patients (27 of 33, 81%) did not receive guidance on red-flag signs. While over half of the patients (19 of 33, 58%) were asked if they had any questions, only 1 patient was asked to teach back his understanding of the discharge plan. Median (IQR) total time spent with patients on the day of discharge by interns, senior residents, attending physicians, and nurses was 4.0 (0.75-6.0), 1.0 (0-2.0), 3.0 (0.5-7.0), and 22.5 (15.5-30.0) minutes, respectively. Most of the time was spent discussing logistics rather than discharge education.
Conclusions and relevance: In this quality improvement study, patients infrequently received discharge education in key communication domains, potentially leaving gaps in patient knowledge. Interventions to improve the hospital discharge process should address the content, method of delivery, and transparency among team members regarding patient education.
Conflict of interest statement
Figures

Comment in
-
Bridging the Know-Do Gap in Hospital Care Transitions.JAMA Intern Med. 2023 May 1;183(5):424-425. doi: 10.1001/jamainternmed.2023.0069. JAMA Intern Med. 2023. PMID: 36939664 No abstract available.
References
-
- Hesselink G, Flink M, Olsson M, et al. ; European HANDOVER Research Collaborative . Are patients discharged with care? a qualitative study of perceptions and experiences of patients, family members and care providers. BMJ Qual Saf. 2012;21(suppl 1):i39-i49. doi: 10.1136/bmjqs-2012-001165 - DOI - PubMed

