Locking the Revolving Door: Racial Disparities in Cardiovascular Disease
- PMID: 36942617
- PMCID: PMC10227271
- DOI: 10.1161/JAHA.122.025271
Locking the Revolving Door: Racial Disparities in Cardiovascular Disease
Erratum in
-
Correction to: Locking the Revolving Door: Racial Disparities in Cardiovascular Disease.J Am Heart Assoc. 2023 Apr 18;12(8):e027676. doi: 10.1161/JAHA.122.027676. Epub 2023 Apr 7. J Am Heart Assoc. 2023. PMID: 37026547 Free PMC article. No abstract available.
Abstract
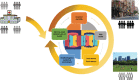
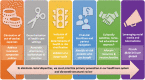
Racial disparities in cardiovascular disease are unjust, systematic, and preventable. Social determinants are a primary cause of health disparities, and these include factors such as structural and overt racism. Despite a number of efforts implemented over the past several decades, disparities in cardiovascular disease care and outcomes persist, pervading more the outpatient rather than the inpatient setting, thus putting racial and ethnic minority groups at risk for hospital readmissions. In this article, we discuss differences in care and outcomes of racial and ethnic minority groups in both of these settings through a review of registries. Furthermore, we explore potential factors that connote a revolving door phenomenon for those whose adverse outpatient environment puts them at risk for hospital readmissions. Additionally, we review promising strategies, as well as actionable items at the policy, clinical, and educational levels aimed at locking this revolving door.
Keywords: cardiovascular disease; disparities; racial.
Figures

Similar articles
-
Race, Racism, and Cardiovascular Health: Applying a Social Determinants of Health Framework to Racial/Ethnic Disparities in Cardiovascular Disease.Circ Cardiovasc Qual Outcomes. 2022 Jan;15(1):e007917. doi: 10.1161/CIRCOUTCOMES.121.007917. Epub 2022 Jan 18. Circ Cardiovasc Qual Outcomes. 2022. PMID: 35041484 Review.
-
Racial Disparities in Cardiovascular Risk and Cardiovascular Care in Women.Curr Cardiol Rep. 2022 Sep;24(9):1197-1208. doi: 10.1007/s11886-022-01738-w. Epub 2022 Jul 8. Curr Cardiol Rep. 2022. PMID: 35802234 Review.
-
Reducing racial and ethnic disparities in cardiovascular outcomes among cancer survivors.Curr Oncol Rep. 2024 Oct;26(10):1205-1212. doi: 10.1007/s11912-024-01578-7. Epub 2024 Jul 13. Curr Oncol Rep. 2024. PMID: 39002054 Review.
-
The Groundwater of Racial and Ethnic Disparities Research: A Statement From Circulation: Cardiovascular Quality and Outcomes.Circ Cardiovasc Qual Outcomes. 2021 Feb;14(2):e007868. doi: 10.1161/CIRCOUTCOMES.121.007868. Epub 2021 Feb 11. Circ Cardiovasc Qual Outcomes. 2021. PMID: 33567860 Free PMC article.
-
Racial and ethnic disparities in cardiometabolic disease and COVID-19 outcomes in White, Black/African American, and Latinx populations: Social determinants of health.Prog Cardiovasc Dis. 2022 Mar-Apr;71:4-10. doi: 10.1016/j.pcad.2022.04.004. Epub 2022 Apr 28. Prog Cardiovasc Dis. 2022. PMID: 35490870 Free PMC article. Review.
Cited by
-
Disparities in statin use following identification of coronary artery calcium.Am J Prev Cardiol. 2025 Apr 11;22:100990. doi: 10.1016/j.ajpc.2025.100990. eCollection 2025 Jun. Am J Prev Cardiol. 2025. PMID: 40290415 Free PMC article.
-
Addressing Unmet Needs in Cardiovascular Care: A Focus on Centers for Medicaid and Medicare Services' Efforts to Integrate Social Determinants of Health Into Health Care.JACC Adv. 2025 Jun;4(6 Pt 1):101813. doi: 10.1016/j.jacadv.2025.101813. Epub 2025 May 19. JACC Adv. 2025. PMID: 40393280 Free PMC article. No abstract available.
-
Creating diverse and inclusive scientific practices for research datasets and dissemination.Imaging Neurosci (Camb). 2024 Jul 12;2:imag-2-00216. doi: 10.1162/imag_a_00216. eCollection 2024. Imaging Neurosci (Camb). 2024. PMID: 40800266 Free PMC article.
-
Race as a Component of Cardiovascular Disease Risk Prediction Algorithms.Curr Cardiol Rep. 2023 Oct;25(10):1131-1138. doi: 10.1007/s11886-023-01938-y. Epub 2023 Aug 15. Curr Cardiol Rep. 2023. PMID: 37581773 Review.
-
Coexistence of Standard Modifiable, Other Classical, and Novel and Classical Atherosclerotic Cardiovascular Disease Risk Factors in Middle Eastern Young Women.Vasc Health Risk Manag. 2024 Jul 8;20:313-322. doi: 10.2147/VHRM.S468209. eCollection 2024. Vasc Health Risk Manag. 2024. PMID: 39005236 Free PMC article.
References
-
- Heckler, M . United States Department of Health and Human Services . Report of the Secretary's Task Force on Black and Minority Health. Washington DC: Department of Health and Human Services. National Library of Medicine; 1985. Accessed March 28, 2021. https://minorityhealth.hhs.gov/assets/pdf/checked/1/ANDERSON.pdf
-
- Smedley BD, Stith AY, Nelson AR, eds. Study charge and committee assumptions ‐ defining racial and ethnic health care disparities. In: Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care. Washington, DC: National Academies Press; 2003. - PubMed
-
- Bernstein A, Bilheimer LT, Makuc DM. Health, United States, 2011; with special feature on socioeconomic status and health. National Center for Health Statistics (U.S.); 2012. DHHS publication; no. 2012‐1232. Accessed February 27, 2023. https://stacks.cdc.gov/view/cdc/13680 - PubMed
-
- Yancy CW, Wang TY, Ventura HO, Pina IL, Vijayaraghavan K, Ferdinand KC, Hall LL, Credo Advisory Group . The coalition to reduce racial and ethnic disparities in cardiovascular disease outcomes (credo): why credo matters to cardiologists. J Am Coll Cardiol. 2011;57:245–252. doi: 10.1016/j.jacc.2010.09.027 - DOI - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

