Cardiovascular and metabolic characters of KCNJ5 somatic mutations in primary aldosteronism
- PMID: 36950676
- PMCID: PMC10025475
- DOI: 10.3389/fendo.2023.1061704
Cardiovascular and metabolic characters of KCNJ5 somatic mutations in primary aldosteronism
Abstract
Background: Primary aldosteronism (PA) is the leading cause of curable endocrine hypertension, which is associated with a higher risk of cardiovascular and metabolic insults compared to essential hypertension. Aldosterone-producing adenoma (APA) is a major cause of PA, which can be treated with adrenalectomy. Somatic mutations are the main pathogenesis of aldosterone overproduction in APA, of which KCNJ5 somatic mutations are most common, especially in Asian countries. This article aimed to review the literature on the impacts of KCNJ5 somatic mutations on systemic organ damage.
Evidence acquisition: PubMed literature research using keywords combination, including "aldosterone-producing adenoma," "somatic mutations," "KCNJ5," "organ damage," "cardiovascular," "diastolic function," "metabolic syndrome," "autonomous cortisol secretion," etc.
Results: APA patients with KCNJ5 somatic mutations are generally younger, female, have higher aldosterone levels, lower potassium levels, larger tumor size, and higher hypertension cure rate after adrenalectomy. This review focuses on the cardiovascular and metabolic aspects of KCNJ5 somatic mutations in APA patients, including left ventricular remodeling and diastolic function, abdominal aortic thickness and calcification, arterial stiffness, metabolic syndrome, abdominal adipose tissue, and correlation with autonomous cortisol secretion. Furthermore, we discuss modalities to differentiate the types of mutations before surgery.
Conclusion: KCNJ5 somatic mutations in patients with APA had higher left ventricular mass (LVM), more impaired diastolic function, thicker aortic wall, lower incidence of metabolic syndrome, and possibly a lower incidence of concurrent autonomous cortisol secretion, but better improvement in LVM, diastolic function, arterial stiffness, and aortic wall thickness after adrenalectomy compared to patients without KCNJ5 mutations.
Keywords: KCNJ5; adrenocortical adenoma; autonomous cortisol secretion (ACS); cardiovascular system; metabolic syndrome; somatic mutation.
Copyright © 2023 Chang, Lee, Chen, Tsai, Chang, Liao, Pan, Peng, Chou, Lu, Wu, Hung, Lin and TAIPAI study group.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

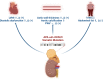
References
-
- Mulatero P, Monticone S, Deinum J, Amar L, Prejbisz A, Zennaro MC, et al. . Genetics, prevalence, screening and confirmation of primary aldosteronism: A position statement and consensus of the working group on endocrine hypertension of the European society of hypertension. J Hypertens (2020) 38(10):1919–28. doi: 10.1097/hjh.0000000000002510 - DOI - PubMed
-
- Parasiliti-Caprino M, Lopez C, Prencipe N, Lucatello B, Settanni F, Giraudo G, et al. . Prevalence of primary aldosteronism and association with cardiovascular complications in patients with resistant and refractory hypertension. J hypertens (2020) 38(9):1841–8. doi: 10.1097/hjh.0000000000002441 - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

