End-of-life care in Brazilian Pediatric Intensive Care Units
- PMID: 36963435
- PMCID: PMC10373144
- DOI: 10.1016/j.jped.2023.02.003
End-of-life care in Brazilian Pediatric Intensive Care Units
Abstract
Objective: Most deaths in Pediatric Intensive Care Units involve forgoing life-sustaining treatment. Such deaths required carefully planned end-of-life care built on compassion and focused on palliative care measures. This study aims to assess topics related to the end of life care in Brazilian pediatric intensive care units from the perspective of a multidisciplinary team.
Method: The authors used a tested questionnaire, utilizing Likert-style and open-ended questions. After ethics committee approval, it was sent by email from September to November/2019 to three Pediatric Intensive Care Units in the South and Southeast of Brazil. One unit was exclusively dedicated to oncology patients; the others were mixed units.
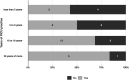
Results: From 144 surveys collected (23% response rate) 136 were analyzed, with 35% physicians, 30% nurses, 21% nurse technicians, and 14% physiotherapists responding. Overall, only 12% reported enough end-of-life care training and 40% reported never having had any, albeit this was not associated with the physician's confidence in forgoing life-sustaining treatment. Furthermore, 60% of physicians and 46% of other professionals were more comfortable with non-escalation than withdrawing therapies, even if this could prolong suffering. All physicians were uncomfortable with palliative extubation; 15% of all professionals have witnessed it. The oncologic team uniquely felt that "resistance from the teams of specialists" was the main barrier to end-of-life care implementation.
Conclusion: Most professionals felt unprepared to forego life-sustaining treatment. Even for terminally ill patients, withholding is preferred over the withdrawal of treatment. Socio-cultural barriers and the lack of adequate training may be contributing to insecurity in the care of terminally ill patients, diverging from practices in other countries.
Keywords: Biomedical ethics; End-of-life care; Palliative care; Pediatric intensive care units; Terminal care.
Copyright © 2023 Sociedade Brasileira de Pediatria. All rights reserved.
Conflict of interest statement
Conflicts of interest The authors declare no conflicts of interest.
Figures
Comment in
-
End-of-life care in Brazilian pediatric intensive care units: challenges and opportunities.J Pediatr (Rio J). 2023 Jul-Aug;99(4):312-314. doi: 10.1016/j.jped.2023.04.002. Epub 2023 May 3. J Pediatr (Rio J). 2023. PMID: 37148909 Free PMC article. No abstract available.
References
-
- Argent A.C. Death and dying over 30 years in the ICU: personal reflection. Pediatr Crit Care Med. 2018;19:S53–S54. - PubMed
-
- Piva J.P. Modes of death and the dying process in Brazilian PICU over the last 30 years: personal reflections. Pediatr Crit Care Med. 2018;19:S59–S60. - PubMed
-
- Namachivayam P., Shann F., Shekerdemian L., Taylor A., van Sloten I., Delzoppo C., et al. Three decades of pediatric intensive care: who was admitted, what happened in intensive care, and what happened afterward. Pediatr Crit Care Med. 2010;11:549–555. - PubMed
-
- Fonseca J.G., Ferreira A.R. Aplicação do Pediatric Index of Mortality 2 em pacientes pediátricos com condição crônica complexa [Application of the Pediatric Index of Mortality 2 in pediatric patients with complex chronic conditions] J Pediatr (Rio J) 2014;90:506–511. Portuguese. - PubMed
-
- Garros D., Rosychuk R.J., Cox P.N. Circumstances surrounding end of life in a pediatric intensive care unit. Pediatrics. 2003;112:e371. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources