The Relationship of Continuity of Care, Polypharmacy and Medication Appropriateness: A Systematic Review of Observational Studies
- PMID: 36972012
- PMCID: PMC10232587
- DOI: 10.1007/s40266-023-01022-8
The Relationship of Continuity of Care, Polypharmacy and Medication Appropriateness: A Systematic Review of Observational Studies
Abstract
Introduction: Worldwide, polypharmacy and medication appropriateness-related outcomes (MARO) are growing public health concerns associated with potentially inappropriate prescribing, adverse health effects, and avoidable costs to health systems. Continuity of care (COC) is a cornerstone of high-quality care that has been shown to improve patient-relevant outcomes. However, the relationship between COC and polypharmacy/MARO has not been systematically explored.
Objective: The aim of this systematic review was to investigate the operationalization of COC, polypharmacy, and MARO as well as the relationship between COC and polypharmacy/MARO.
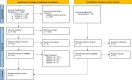
Methods: We performed a systematic literature search in PubMed, Embase, and CINAHL. Quantitative observational studies investigating the associations between COC and polypharmacy and/or COC and MARO by applying multivariate regression analysis techniques were eligible. Qualitative or experimental studies were not included. Information on the definition and operationalization of COC, polypharmacy, and MARO and reported associations was extracted. COC measures were assigned to the relational, informational, or management dimension of COC and further classified as objective standard, objective non-standard, or subjective. Risk of bias was assessed by using the NIH Quality Assessment Tool for Observational Cohort and Cross-Sectional Studies.
Results: Twenty-seven studies were included. Overall, substantial differences existed in terms of the COC dimensions and related COC measures. Relational COC was investigated in each study, while informational and management COC were only covered among three studies. The most frequent type of COC measure was objective non-standard (n = 16), followed by objective standard (n = 11) and subjective measures (n = 3). The majority of studies indicated that COC is strongly associated with both polypharmacy and MARO, such as potentially inappropriate medication (PIM), potentially inappropriate drug combination (PIDC), drug-drug interaction (DDI), adverse drug events (ADE), unnecessary drug use, duplicated medication, and overdose. More than half of the included studies (n = 15) had a low risk of bias, while five studies had an intermediate and seven studies a high risk of bias.
Conclusions: Differences regarding the methodological quality of included studies as well as the heterogeneity in terms of the operationalization and measurement of COC, polypharmacy, and MARO need to be considered when interpreting the results. Yet, our findings suggest that optimizing COC may be helpful in reducing polypharmacy and MARO. Therefore, COC should be acknowledged as an important risk factor for polypharmacy and MARO, and the importance of COC should be considered when designing future interventions targeting these outcomes.
© 2023. The Author(s).
Conflict of interest statement
David Lampe, John Grosser, Daniel Gensorowsky, Julian Witte, Wolfgang Greiner, Christiane Muth, Marjan van den Akker, and Truc Sophia Dinh declare that they have no conflict of interest.
Figures



Similar articles
-
Medication Appropriateness, Polypharmacy, and Drug-Drug Interactions in Ambulatory Elderly Patients with Cardiovascular Diseases at Tikur Anbessa Specialized Hospital, Ethiopia.Clin Interv Aging. 2022 Apr 16;17:509-517. doi: 10.2147/CIA.S358633. eCollection 2022. Clin Interv Aging. 2022. PMID: 35464156 Free PMC article.
-
A combination of Beers and STOPP criteria better detects potentially inappropriate medications use among older hospitalized patients with chronic diseases and polypharmacy: a multicenter cross-sectional study.BMC Geriatr. 2023 Jan 25;23(1):44. doi: 10.1186/s12877-023-03743-2. BMC Geriatr. 2023. PMID: 36694126 Free PMC article.
-
Frailty and Potentially Inappropriate Prescribing in Older People with Polypharmacy: A Bi-Directional Relationship?Drugs Aging. 2022 Aug;39(8):597-606. doi: 10.1007/s40266-022-00952-z. Epub 2022 Jun 29. Drugs Aging. 2022. PMID: 35764865 Free PMC article. Review.
-
Polypharmacy in chronic diseases-Reduction of Inappropriate Medication and Adverse drug events in older populations by electronic Decision Support (PRIMA-eDS): study protocol for a randomized controlled trial.Trials. 2016 Jan 29;17:57. doi: 10.1186/s13063-016-1177-8. Trials. 2016. PMID: 26822311 Free PMC article. Clinical Trial.
-
The influence of patients' beliefs about medicines and the relationship with suboptimal medicine use in community-dwelling older adults: a systematic review of quantitative studies.Int J Clin Pharm. 2024 Aug;46(4):811-830. doi: 10.1007/s11096-024-01727-9. Epub 2024 May 5. Int J Clin Pharm. 2024. PMID: 38704779 Free PMC article.
Cited by
-
Association between continuity of care and inappropriate prescribing in outpatient care in Germany: a cross-sectional analysis conducted as part of the LoChro trial.BMJ Open. 2024 Jul 22;14(7):e082245. doi: 10.1136/bmjopen-2023-082245. BMJ Open. 2024. PMID: 39038858 Free PMC article.
-
Integrative Analysis of Drug Co-Prescriptions in Peritoneal Dialysis Reveals Molecular Targets and Novel Strategies for Intervention.J Clin Med. 2025 May 26;14(11):3733. doi: 10.3390/jcm14113733. J Clin Med. 2025. PMID: 40507495 Free PMC article.
-
Multicenter study in Turkiye of unsuppressed viremia in people living with human immunodeficiency virus: aegean experience.BMC Infect Dis. 2025 Apr 23;25(1):587. doi: 10.1186/s12879-025-10988-2. BMC Infect Dis. 2025. PMID: 40269772 Free PMC article.
-
Determinants of and interventions for Proton Pump Inhibitor prescription behavior: A systematic scoping review.BMC Prim Care. 2024 Jun 11;25(1):208. doi: 10.1186/s12875-024-02459-5. BMC Prim Care. 2024. PMID: 38862886 Free PMC article.
-
Predictors of 15-year transitions across living and care settings in a population of Swedish older adults.Age Ageing. 2025 Jan 6;54(1):afaf006. doi: 10.1093/ageing/afaf006. Age Ageing. 2025. PMID: 39864066 Free PMC article.
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

