Natural history and predictors for progression in pediatric keratoconus
- PMID: 36973341
- PMCID: PMC10042985
- DOI: 10.1038/s41598-023-32176-5
Natural history and predictors for progression in pediatric keratoconus
Abstract
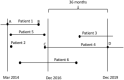
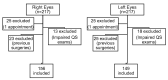
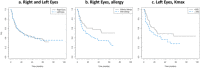
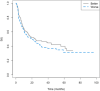
We studied the demographic and clinical predictors associated with keratoconus progression in a pediatric population. Retrospective cohort study. We evaluated 305 eyes without previous surgeries from 168 patients, 9 to < 18 years old, and with a minimum 36-month follow-up in a hospital corneal ambulatory. We used Kaplan-Meyer survival curves; the dependent variable (main outcome measure) was the interval time (months) until the event, defined as an increase of 1.5 D in the maximum keratometry (Kmax), obtained with Pentacam. We evaluated the predictors: age (< or ≥ 14 years), sex, keratoconus familial history, allergy medical history, and the baseline tomographic parameters: mean keratometry (Km), Kmax (< or ≥ 55 D); and thinnest pachymetry (TP). We used log-rank tests and compared median survival times for right (RE)/left eyes (LE) and better (BE)/worse eyes (WE). A p value < 0.05 was considered significant. The patients' mean ± SD age was 15.1 ± 2.3 years old; 67% were boys, 30% were < 14 years, 15% had keratoconus familial history, and 70% were allergic. The general Kaplan-Meyer curves showed no differences between RE/LE or BE/WE. RE with allergy and LE with Kmax ≥ 55 D had smaller survival times ((95%CI 9.67-32.1), p 0.031 and (95%CI 10.1-44.1), p 0.042, respectively). For BE and WE, Kmax ≥ 55 D had smaller survival times ((95% CI 6.42- ), p 0.031 and (95%CI 8.75-31.8), p 0.043, respectively). Keratoconus progression was similar between RE/LE and BE/WE. Steepest corneas are predictors of faster progression. Allergy is also a predictor of keratoconus progression in RE.
© 2023. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures
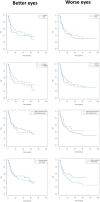
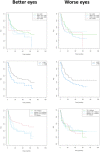
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

