Virtual healthcare solutions for cardiac rehabilitation: a literature review
- PMID: 36974268
- PMCID: PMC10039430
- DOI: 10.1093/ehjdh/ztad005
Virtual healthcare solutions for cardiac rehabilitation: a literature review
Abstract
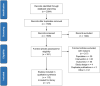
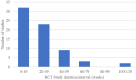
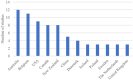
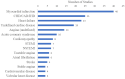
Graphical AbstractAdherence to cardiac rehabilitation following a primary event has been demonstrated to improve quality of life, increase functional capacity, and decrease hospitalizations and mortality. Mobile technologies offer an opportunity to improve both the quality and utilization of cardiac rehabilitation, and recent clinical studies investigated this technology. This literature review summarizes the current use of mobile health, wearable activity monitors (WAMs), and other multi-component technologies deployed to support home-based virtual cardiac rehabilitation. The methodology was adapted from the Cochrane Handbook for Systematic Reviews of Interventions. We identified 2094 records, of which 113 were eligible for qualitative analysis. Different virtual cardiac rehabilitation solutions were implemented in the studies: (i) multi-component interventions in 48 studies (42.5%), (ii) WAMs in 27 studies (23.9%), (iii) web-based communications solutions, and (iv) mobile apps, both in 19 studies (16.4%). Functional capacity was the most frequently reported primary outcome (k = 37, 32.7%), followed by user adherence/compliance (k = 35, 31.0%), physical activity (k = 27, 23.9%), and quality of life (k = 14, 12.4%). Studies provided a mixed assessment of the efficacy of virtual cardiac rehabilitation in attaining either significant improvements over baseline or significant improvements in outcomes compared with conventional rehabilitation. Efficacy outcomes with virtual cardiac rehabilitation sometimes improve on the centre-based outcomes; however, superior clinical efficacy may not necessarily be the only outcome of interest. The promise of virtual cardiac rehabilitation includes the potential for increased user adherence and longer-term patient engagement. If these outcomes can be improved, that would be a significant justification for using this technology.
Keywords: Cardiac rehabilitation; Self-care; Telemedicine; Virtual healthcare; eHealth; patient empowerment.
© The Author(s) 2023. Published by Oxford University Press on behalf of the European Society of Cardiology.
Conflict of interest statement
Conflict of interest: K.C.S.L. and A.U. report employment by Sanofi and may hold shares and/or stock options in the company. B.B. reports contract employment by Evidinno Outcomes Research Inc. F.K. is currently employed by Charité—Universitätsmedizin and has an ownership interest in Zentrum für kardiovaskuläre Telemedizin GmbH. F.K. has received research funding grants from the German Federal Ministry of Education and Research and grants from the Federal Ministry of Economic Affairs and Energy for conducting research and clinical trials in remote patient management. F.K. has received personal fees (honoraria) for lectures from Boston Scientific, Sanofi-Aventis Deutschland GmbH, Biotronik SE & Co. KG, Novartis, Linde/Saúde, Roche Pharma AG, Amgen GmbH, and Astra Zeneca outside the submitted work. F.K. is co-holder of the patents PCT/EP2020/058700, European Patent Application No. 19166382.2, No. 19166425.9, and No. 19175720.2. F.K. has received personal fees for advisory boards from Abbott, Sanofi-Aventis Deutschland GmbH, and Biotronik Se & Co. KG. F.K. is a member of the European Society of Cardiology (ESC), German Cardiac Society (DGK), German Society for Internal Medicine (DGIM), and German Centre for Cardiovascular Research (DHZK). S.S.M. reports research support from American Heart Association (20SFRN35380046, 20SFRN35490003, 878924, 882415), PCORI (ME-2019C1-15328), National Institutes of Health (R01AG071032, P01 HL108800), the David and June Trone Family Foundation, and Pollin Digital Health Innovation Fund, the PJ Schafer Cardiovascular Research Fund, Sandra and Larry Small, CASCADE FH, Apple, Google, and Amgen. Under a license agreement between Corrie Health and the Johns Hopkins University, the University owns equity in Corrie Health, and the University and S.S.M. are entitled to royalty distributions related to the technology. In addition, S.S.M. is a co-founder of and holds equity in Corrie Health. This arrangement has been reviewed and approved by Johns Hopkins University in accordance with its conflict-of-interest policies. S.S.M. reports consulting in the last 24 months with Amgen, AstraZeneca, DalCor, iHealth, Kaneka, NewAmsterdam, Novartis, Novo Nordisk, Sanofi, and 89bio. The authors report no other conflicts of interest.
Figures

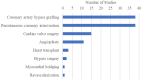
References
-
- Wenger NK. Current status of cardiac rehabilitation. J Am Coll Cardiol 2008;51:1619–1631. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
